ARCHIVED FACEBOOK POSTS
The Sister Study is on Facebook!
We are excited to let you know that we have created a private Facebook group for the Sister Study to provide a forum for Sister Study participants, colleagues and friends of the study. This private group is by invitation only and not a public forum. We saw the need to have a more dynamic way of communicating with our Sister Study community than just the Sister Study website. We see the Facebook group as a real-time forum where we can post study updates, announcements, and new research findings or plans.
We know that Facebook has been in the news lately because of how they use their users' data. We want you to know that, as a research study funded by a government entity, we will abide by all NIEHS privacy policies.![]() We will not share your information with third parties. We ourselves will never post any personal and/or identifiable information on Facebook. If you decide to use your own real name, be mindful that you are responsible for that information. We will provide guidelines for what not to post, such as personal health information, treatment recommendations, and product endorsements or posts with an intent to sell. Our staff will monitor the group to make sure that policies are followed and remove inappropriate material.
We will not share your information with third parties. We ourselves will never post any personal and/or identifiable information on Facebook. If you decide to use your own real name, be mindful that you are responsible for that information. We will provide guidelines for what not to post, such as personal health information, treatment recommendations, and product endorsements or posts with an intent to sell. Our staff will monitor the group to make sure that policies are followed and remove inappropriate material.
We
invite you to follow this direct link https://www.facebook.com/groups/niehssisterstudy/ ![]() if you would like to join.
if you would like to join.
We hope you find this additional communication method helpful and that you enjoy connecting with other study participants, colleagues and friends of the study.
Facebook Posts
Younger age at menarche is an established risk factor for both breast and uterine cancer. Earlier age at onset of breast development (thelarche) has also been linked to increased breast cancer risk, but less is known about its associations with uterine cancer. This is particularly important to study given that there have recently been rapid declines in age at thelarche and increases in uterine cancer incidence rates. Among 34,152 Sister Study participants who still had their uterus at enrollment, 445 women reported a new uterine cancer diagnosis. Earlier ages at thelarche and menarche were associated with increased risk of uterine cancer. These findings suggest that younger ages at thelarche and menarche, markers of earlier and potentially prolonged exposure to estrogen in the absence of progesterone during puberty, may enhance susceptibility to uterine carcinogenesis.
Learn more here:
Pubertal timing and incident uterine cancer in the Sister Study cohort. ![]()
Do you remember taking dust samples when you enrolled in the Sister Study? We asked all participants to swab the tops of door frames from three different rooms with alcohol wipes so that we could measure what environmental chemicals were present in your home. In a newly published study, we report results for a small sample of women: 40 with hormone receptor positive breast cancer and 40 without. Overall, there were 189 chemicals that showed up in different quantities for women with or without breast cancer. This included several suspected endocrine disrupting chemicals that were more common in homes of women who later developed breast cancer. Higher levels of some chemicals were associated with frequent personal care product use. Although based on a small number of women, these results provide insights into how environmental chemicals present in the home may affect breast cancer risk and can also help researchers identify possible sources of exposure.
A few weeks back we shared research on hair straighteners/chemical relaxers and cancer risk. Did you know this study was also featured as an NIEHS Paper of the Month and highlighted in broader NIH commentary? The research from 46,000+ Sister Study participants found that use of these products was linked to higher incidence of thyroid cancer, non-Hodgkin lymphoma, and pancreatic cancer. The study's findings have sparked further discussion across NIH and professional networks about how everyday exposures might relate to health risks and the importance of follow-up research to understand these associations more fully.
Link to NIEHS Paper of the Month:
Hair straightener/relaxer use may be linked to pancreatic cancer, thyroid cancer. ![]()
Link to full article:
Use of hair straighteners and chemical relaxers and incidence of non-reproductive cancers. ![]()
World Cancer Day is recognized each year on February 4th to raise awareness about cancer and to encourage its prevention, early detection, and treatment. Today and every day we are deeply grateful to our Sister Study participants and their families for your longstanding commitment to the Sister Study.
For many years, you have shown your dedication by generously sharing detailed information about your health and your family's health, and by saying 'yes' when we invite you to participate in new and exciting special efforts. Each year that you provide this information, you help investigators better understand factors related to cancer risk and improve knowledge that benefits future generations. Woman by woman...Sister by sister...you are still making a difference.

Meet Eva Bauer, you may recognize Eva's name from emails or letters you receive throughout the year from the Sister Study. Over her five years with the study, Eva has taken on many roles. In her current role as the Program Manager, she leads the study team and oversees many of the activities that make the Sister Study possible. This includes everything from collecting and processing participant health data, retention activities, helping to share important research findings to leading our new and exciting Anniversary Biospecimen Collection effort!
Eva has spent most of her career working in cancer research and is deeply committed to advancing women's health research. She completed her undergraduate and graduate studies at the University of Washington and the University of North Carolina, experiences that helped shape her passion for supporting long-term research efforts like the Sister Study.
Outside of work, Eva enjoys spending time outdoors, especially visiting National Parks, hiking, and kayaking. She enjoys traveling and is a lifelong learner who loves reading and visiting museums. On the weekends, you might find Eva in her kitchen trying out new recipes. She's currently working on perfecting her cinnamon rolls and banana bread! She also loves spending time with her loved ones, especially her two pups, Rex and Rascal.
A message from Eva: "I am so grateful to be a part of the Sister Study community! Two of my favorite parts of my role are having the opportunity to connect with our wonderful and dedicated participants and working with such a passionate and talented team of scientists, study staff, and collaborators. I am continuously impressed by what our team accomplishes together, especially the groundbreaking findings our study has produced that have made a meaningful impact on women's health research. None of this would be possible without our amazing participants who complete health update questionnaires, provide biospecimens, and continue to participate in the study."
A recent post shared by NIEHS highlights how the Sister Study is helping us better understand environmental contributors to breast cancer.
Learn more here:
Five Things to Know About Breast Cancer Research. ![]()
Sister Study investigators led the largest US-based study to date of the association between outdoor air pollution exposure and breast cancer risk. The investigation pooled data from 5 large cohorts, including the Sister Study, that had estimated levels of exposure to 3 types of air pollution based on participants’ residences. Nitrogen dioxide (NO2), which is often considered a measure of exposure to traffic-related air pollution, was positively associated with breast cancer overall. Ozone and air pollution made up of small particles (PM2.5) were both positively associated with the occurrence of hormone receptor negative breast cancers. This landmark study provides confirmation of a link between NO2 and breast cancer and presents new evidence that PM2.5 and ozone may be specifically linked to hormone receptor negative disease.
Learn more here:
Air Pollutants and Breast Cancer Risk: A Parallel Analysis of Five Large US Prospective Cohorts. ![]()
In an analysis that included nearly 68,000 women from 13 cohorts including the Sister Study, investigators looked at how variants in breast cancer predisposition genes (e.g., BRCA1, BRCA2, PALB2, CHEK2), family history, and other known risk factors impact breast cancer risk in the general US population. Pathogenic variants were rare, ranging from 1% in breast cancer-free women with no family history to 9% in women with breast cancer and a first-degree family history. Women with a pathogenic variant and a first-degree family history of breast cancer had an estimated 23% risk of breast cancer by age 50 years and a 51% risk between age 50 and 80 years, compared with an estimated 9% risk by age 50 years and 30% risk between ages 50 and 80 years in women with a pathogenic variant but no family history. Risk among pathogenic variant carriers varied according to the affected gene and established risk factors. Women with pathogenic variants can use these risk estimates to guide screening and prevention decisions.
Learn more here:
Pathogenic Variants, Family History, and Cumulative Risk of Breast Cancer in US Women. ![]()
Use of hair straighteners and chemical relaxers has been associated with increased incidence of breast, uterine, and ovarian cancers, but their association with non-reproductive cancers has not been investigated. Among 46,287 women from the Sister Study, use of hair straighteners /chemical relaxers was associated with a higher incidence of thyroid cancer, non-Hodgkin's lymphoma, and pancreatic cancer, with little to no evidence of links to melanoma, lung cancer, leukemia, colorectal cancer or kidney cancer. Further research is needed to confirm these findings, but these results provide additional evidence that use of chemical hair products may increase cancer risk.
Learn more here:
Use of hair straighteners and chemical relaxers and incidence of non-reproductive cancers. ![]()
Uterine fibroids and endometriosis are two non-cancerous gynecological conditions that share some symptoms. Both conditions are influenced by hormones such as estrogen and there is some evidence they may be associated with ovarian cancer risk. Some women with these conditions have their uterus removed (hysterectomy), which could also impact their ovarian cancer risk. In the Sister Study, 34% of 40,928 eligible participants have reported a fibroid diagnosis, 13% reported having had endometriosis, and 7% reported having both. 20% of participants have had a hysterectomy. Women with fibroids had a 65% increased rate of developing ovarian cancer, compared to women without fibroids. Among women with fibroids, those who had a hysterectomy were less likely to develop ovarian cancer than those who did not. History of endometriosis was not associated with risk. Studying the joint effects of fibroids, endometriosis and hysterectomies adds to our understanding of ovarian cancer and may help inform decisions about how women with fibroids, endometriosis, and hysterectomies are treated and monitored.
Learn more here:
The independent and joint associations of hysterectomy and uterine fibroids or endometriosis with ovarian cancer incidence: results from a US-based cohort. ![]()
Hypertension, or high blood pressure, affects nearly a billion people globally and may be impacted air pollution. We used data from the US Environmental Protection Agency's 2005 National Air Toxics Assessment (NATA) database to estimate airborne levels of three widely used phthalates—chemicals commonly used in plastics—for 47,465 Sister Study participants. The NATA data incorporate information on industrial emissions and monitored air pollution levels to estimate exposures across the US. We found that women who lived in areas with high estimated levels of these phthalates were more likely to have been diagnosed with hypertension. The positive association between airborne phthalates and hypertension may be stronger among women who identify as a race/ethnicity other than non-Hispanic White.
Learn more here:
Airborne phthalate exposures and hypertension in the Sister Study. ![]()

Meet Angelica! She supervises the Survey Research Center team, which manages participant outreach and retention for the Sister Study.
Her favorite part of working on the Sister Study: "Over the past 20 years, I've had the privilege of seeing more than 50,000 amazing women come together to help uncover the causes of breast cancer. This work is especially meaningful to me because members of my own family have been affected by this disease. I'm so grateful to be part of this effort and to connect every day with Sisters from all walks of life who share the same goal—improving women's health for generations to come. My favorite part of what I do is hearing from our participants and sharing in this journey with all of you."
Sister Study investigators examined whether sleep health varied by sexual orientation or perceived discrimination due to sexual orientation. Compared to heterosexual women, women who self-identified as non-heterosexual were more likely to use sleep masks, and Black non-heterosexual women were more likely to use sleep medications. While poor sleep health was not more common among non-heterosexual women overall, perceived discrimination was shown to negatively impact sleep health. Sleep aid use may help reduce sleep disparities by sexual orientation.
Learn more here:
Sleep Health by Sexual Orientation among Women in the United States and Interrelations with Race/Ethnicity, Age, and Generational Cohort. ![]()
In collaboration with Sister Study researchers, a team of investigators from the National Heart, Lung, and Blood Institute (part of the National Institutes of Health) found that moderate and frequent use of commonly used ("everyday") personal care products, compared to low use, were associated with higher rates of newly diagnosed asthma, which had impacted 1,774 Sister Study participants since enrollment. Similar trends were observed for specific groups of products, including beauty products, hygiene-related products, and skincare products. This work adds to a growing body of literature, much of which comes from Sister Study investigations, that personal care products may contain chemicals or other agents that have adverse effects on health.
Learn more here:
Personal care product use and risk of adult-onset asthma: Prospective cohort analyses of U.S. Women from the Sister Study. ![]()

Meet Noelle! She's the Sister Study's go-to Graphics and Web Designer and has been part of the team for three years. Noelle brings creativity and heart to everything she designs—from newsletters to web graphics. She's the one who helps make our updates not only informative but beautiful! Dependable, adaptable, and always up for a new challenge, Noelle keeps our materials looking their best.
Her favorite part of working on the Sister Study: "My favorite part of working with the Sister Study is helping share the important discoveries and updates with participants. As a designer, I get to create newsletters and materials that connect the research team with all of you—the science more accessible and showing the impact of your long-term commitment!"
The Sister Study collected data on average sedentary time (hours per day spent sitting) as part of the first detailed follow-up questionnaire, which participants were asked to complete between 2008-2012. Women were categorized as sitting ≤5 hours/day, 6-9 hours/day, or ≥10 hours/day, on average, during weekdays. Increased sedentary time was associated with higher rates of postmenopausal breast cancer. However, the association was different for premenopausal breast cancer, where increased sedentary time was associated with a reduced risk. This paper adds to our understanding of possible differences between the causes of pre- and post-menopausal breast cancer.
Learn more here:
Sedentary Time and Breast Cancer Risk in the Sister Study Cohort. ![]()
Sister Study researchers often use participant-provided residential address information to estimate personal exposures to environmental factors, such as air pollution, extreme temperatures, or residential proximity to hazardous emissions or other environmental contaminants. In the enrollment questionnaire, participants were asked to provide details on their current address, longest lived address and childhood address. These timeframes were sufficient to capture lifetime exposures for many women, but exposures for women who moved frequently have been harder to estimate. To fill in these gaps, we used publicly available information to construct detailed residential histories. When we asked a subset of participants to validate these histories, we found that 95% of address locations and 82% of residence durations were accurately captured. By taking advantage of this information, we have now added a median of 25 years of residential history information without having to ask participants to remember and report all of their prior addresses. These more complete residence histories will be extremely valuable for investigating the health effects of environmental exposures over the life-course and potentially identifying periods when women may be more susceptible to the effects of environmental exposures.
Learn more here:
Accuracy of LexisNexis-derived retrospective address histories in the Sister Study cohort. ![]()
"Weight cycling" is a term used to describe when individuals repeatedly lose and then regain weight. For Sister Study participants, we defined weight cycling as losing and then regaining ≥20 pounds (9 kilograms) and used responses from the enrollment questionnaire to define how many times women had weight cycled up to that point. We found that increased weight cycling was associated with a lower risk of developing breast cancer, even after we accounted for differences in body weight. The strongest associations were observed in postmenopausal women and women who were obese at enrollment. However, weight cycling was not associated with risk of endometrial, ovarian, colorectal or kidney cancer. Weight cycling is not likely to be a risk factor for cancer overall and may be associated with a lower risk of breast cancer, possibly because women who experience weight cycling have had extended periods of time when they are not overweight or obese.
Learn more here:
Weight Cycling and Cancer Risk in the Sister Study. ![]()

October is Breast Cancer Awareness Month and we at the Sister Study would like to join our participants and friends of the study to remember those affected by breast cancer. With our ongoing research, we honor those we have lost and those who continue to fight against breast cancer. We are grateful to those of you who participate in research like the Sister Study so we can work together toward solutions. Thank you.
Some types of per- and polyfluoroalkyl substances (PFAS)—also known as "forever chemicals" because of persistence in both the environment and human bodies—have been phased out and replaced by other substances with unknown health impacts. Sister Study investigators analyzed blood samples provided by 200 participants at 2 time points—2007-08 and 2013-14—to get a better understanding of what substances were present and how levels changed over time. They detected 24 previously known PFAS and 1,802 additional substances with PFAS-like properties. The amounts of additional PFAS-like chemicals increased over time. Levels of all PFAS were correlated with chemicals involved in lipid and amino acid metabolism, but novel PFAS were additionally correlated with carbohydrate, vitamin and endocrine metabolism. The results from this preliminary study will be used to inform a larger study of the association of PFAS and breast cancer in the Sister Study cohort.
Learn more here:
Novel and legacy per- and polyfluoroalkyl substances in humans: Long-term temporal variability and metabolic perturbations. ![]()
Between study enrollment and September 2021, 291 Sister Study participants were diagnosed with ovarian cancer. Puberty events such as menarche (first period) and thelarche (onset of breast development) are indicators of hormonal changes. Although many hormonal factors have been linked to ovarian cancer risk, Sister Study investigators did not see any association between age at thelarche or age at menarche and the occurrence of overall ovarian cancer. A possible link between earlier thelarche and menarche and increased incidence of clear cell carcinoma of the ovary may warrant further investigation, especially given trends towards earlier thelarche in the US population.

Many of you may not realize it, but Sha-Mel has been an important part of your Sister Study journey from the very beginning! He was the person who sent out your original baseline kits, and today he's the one making sure you receive your Anniversary Biospecimen Collection Kits, along with every questionnaire and letter you've received over the past 19 years. Behind the scenes, Sha-Mel coordinates with a team to carefully prepare, package, and ship thousands of study materials each month, ensuring they arrive on time and ready for you to use.
His favorite part of working on the Sister Study: Reading your thank you notes and seeing the impact this research has on participants like you. These notes remind him just how meaningful this study is—and how special each of you are to it.
Existing breast cancer prediction models may not generalize to younger women, who have been under-represented in the samples used to develop such models. Data from the Sister Study and 18 other prospective cohorts were used to develop a prediction model for premenopausal breast cancer, which included known or suspected risk factors. The relative contribution of each factor was similar to prediction models developed to predict breast cancer in all women, highlighting the need to identify factors that more specifically predict breast cancer risk in premenopausal women.
Learn more here:
Development and validation of a risk prediction model for premenopausal breast cancer in 19 cohorts. ![]()
Among 45,746 women from the Sister Study there was no association between history of diagnosed depression and breast cancer. However, antidepressant use, especially the use of selective serotonin reuptake inhibitors (SSRIs), was associated with reduced risk of breast cancer. This association was strongest in women with normal range or lower body mass index (<25 kg/m2). This research contributes to our understanding of breast cancer risk and the long-term health effects of antidepressants.
Learn more here:
Depression, antidepressant use, and breast cancer incidence in the Sister Study cohort. ![]()
Iron is necessary for bodily function, but abnormal levels can increase the risk of some chronic diseases. We measured levels of iron or iron-related proteins (ferritin and transferrin) in blood samples collected at enrollment from 1,260 randomly-selected Sister Study participants. We also used the blood samples to assess each participant's "biological age" based on chemical markers attached to DNA ("DNA methylation"). Ferritin was positively associated with biological age, but iron and transferrin were not, meaning that accelerated biological aging does not explain the link between high iron and increased risk of chronic disease.
Learn more here:
Association Between Body Iron Status and Biological Aging. ![]()
Patients with diverticulitis are often told to avoid eating nuts and seeds, but a recent Sister Study analysis showed that higher dietary intake of nuts, seeds, and corn was not linked to an increased risk for developing diverticulitis and that overall healthy dietary patterns (which sometimes include nuts and seeds) were associated with a lower occurrence of diverticulitis.
Learn more here:
Summary for Patients: Diet and Risk for Incident Diverticulitis in Women. ![]()

Meet Irina Khodush, who has been with the Sister Study since day one—22 years and counting! Irina plays a critical role in shaping how we collect and manage participant data. Her dedication over the past two decades has helped ensure the information you provide is accurate, organized, and ready for researchers to use in advancing women's health. As the Data Processing Manager, Irina helps develop data collection instruments and oversees all data processing activities once the data is collected.
Favorite part of working on the Sister Study: "Each year, we prepare a package of data sets for the annual data release. It's my favorite part of the Sister Study—seeing the final product of everything the participants and our team accomplish together. It would be impossible without the wholehearted dedication of our participants. From completing health updates to volunteering for additional study activities like cancer validation and specimen collection, their continued support and encouragement means so much."
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Sisters Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!

Meet Matthew Carter, one of the amazing people behind the data that drives the Sister Study. His behind-the-scenes work helps ensure the data we collect is accurate, organized, and accessible for researchers—making research discoveries possible every day. Matt is one of the programmers and data managers supporting the Sister Study. He is responsible for cleaning and processing participant data and manages the Sister Study Diagnosis Database, which contains nearly three million records of participant diagnoses.
Favorite part of working on the Sister Study: "I'm continually impressed and humbled by the dedicated cohort of women who continue to participate in the study—some for more than 20 years. The data collected over the life of the Sister Study will be used for decades to come to advance research on a wide range of health outcomes, including breast cancer. It's truly an honor to be part of such an important effort."
Summary: Central body fat is not associated with premenopausal breast cancer after accounting for the previously established inverse association between BMI and breast cancer before menopause.
Among premenopausal women, higher body mass index (BMI) is known to be associated with lower breast cancer risk, although the underlying biological mechanisms behind this association remain unclear. In a study that included the Sister Study and 13 other prospective cohorts (440,179 women total), researchers investigated the role of central (around the trunk and upper body) and peripheral (around the hips and lower body) adiposity (body fat) with breast cancer occurring prior to menopause. Waist circumference and other measures of central adiposity were inversely associated with premenopausal breast cancer risk. However, this association was no longer seen once BMI was added to statistical models. Overall, the analysis did not support an association between central adiposity and premenopausal breast cancer risk beyond the previously established inverse association between BMI and premenopausal breast cancer.
Learn more here:
Central and peripheral adiposity and premenopausal breast cancer risk: a pooled analysis of 440,179 women . ![]()
Summary: Living near low to moderate greenspace rather than high greenspace was associated with a higher prevalence of moderate or poor sleep health.
Sleep is essential for overall health. Greenspace, which includes parks and other areas with grass, trees, or other vegetation, may contribute to sleep health by improving mood, reducing sleep disruptors (e.g., poor air quality, noise), and promoting physical activity. In the Sister Study, greenspace was measured by linking participants' addresses to a NASA-derived satellite-based measure of green space. Overall, living near low to moderate greenspace rather than high greenspace was associated with a higher prevalence of moderate or poor sleep health.
Learn more here:Greenspace proximity in relation to sleep health among a racially and ethnically diverse cohort of US women .
Estrogen plus progestin hormone therapy is an established risk factor for breast cancer in postmenopausal women, but less is known about the association between hormone therapy use and breast cancer in younger women, who may use hormone therapy following gynecologic surgery or to relieve peri-menopausal symptoms. Sister Study investigators recently studied this topic using pooled data from 10 international cohorts. They found that unopposed estrogen therapy use was inversely associated with breast cancer before age 55 and that estrogen plus progestin hormone therapy use was positively associated with breast cancer before age 55, especially for longer-term use and among women without hysterectomy or bilateral oophorectomy. These results are similar to prior studies of hormone use and later-onset breast cancer, but provide novel evidence for informing clinical recommendations for hormone therapy use in young women.
Learn more here:
Breast cancer risk in younger women may be influenced by hormone therapy. ![]()
Having higher birth weight or a mother who experienced high blood pressure or diabetes when pregnant was associated with an increased incidence of thyroid cancer in adult women.
A new Sister Study analysis examined whether exposures during the prenatal period and at birth could influence a woman's risk of developing thyroid cancer later in life. The study used information reported by participants about their parents' health and behaviors before and during pregnancy, as well as their own birth characteristics. Researchers found that women whose mothers had high blood pressure or diabetes when pregnant with them were more likely to develop thyroid cancer as adults. Higher birth weight was also associated with higher risk. Further research with more detailed information on early-life conditions is needed to confirm these findings and better understand the biological mechanisms involved.
Learn more here:
In-utero and newborn factors and thyroid cancer incidence in adult women in the Sister Study cohort. ![]()
Self-reported height and weight can reliably be used to estimate BMI categories across socioeconomic, racial, and ethnic groups.
Women often under-report their weight and over-report their height, which reduces the accuracy of any studies using self-reported estimates to calculate body mass index. Further, differences in reporting may vary by factors such as socioeconomic status and race and ethnicity, which could produce differential misclassification and bias results for some subgroups more than others. We assessed agreement between self-reported and objectively-measured weight, height, and BMI, collected upon enrollment in the Sister Study. Among 18,638 included participants, weight and height were both generally underreported, with self-reported weight less accurately reported by Black and Latina participants and for those who completed a college education. However, when women were placed into BMI categories based on their self-reported versus objectively-measured BMI, there was high agreement across measures for all groups. These results demonstrate that self-reported data can reliably be used to estimate BMI categories across socioeconomic, racial, and ethnic groups.
Learn more here:
Agreement between self-reported and measured weight, height, and derived BMI by educational attainment across racial and ethnic groups of US women . ![]()
Truncating mutations (i.e., mutations that led to a shortened protein) near the start or end of BRCA2 were associated with higher breast cancer risk than truncating mutations in the middle of the gene.
ATM, BRCA1, BRCA2, CHEK2, and PALB2 are genes that confer high risk breast cancer, but risk differences by mutation type and location have not been well described. The Sister Study contributed to a large collaborative study that included 32,247 women with and 32,544 women without breast cancer. The study's most notable findings were for BRCA2, where investigators found that truncating mutations (i.e., mutations that led to a shortened protein) near the start of the gene (exons 1-10) or near the end of the gene (exons 13-27) were associated with higher breast cancer risk than truncating mutations in the middle of the gene (exon 11). However, exon 11 mutations were associated with increased risk of ER-negative breast cancer, as well as later-onset breast cancer. These findings have been replicated in other studies and the results can be used to improve individualized risk prediction and clinical management for women carrying BRCA2 truncating mutations.
Learn more here:
Association of gene variant type and location with breast cancer risk in the general population . ![]()
Trauma in early life may contribute to changes in DNA and, potentially, health risks later in life.
In this study, we assessed whether women who experienced different types of psychological or physical trauma during early life had detectable differences in DNA methylation, a type of chemical modification to DNA that can affect how a particular gene is translated into a protein. Using DNA extracted from baseline blood samples from a subset of Sister Study participants, we identified 108 areas of the genome that differed between those who did and did not experience any early life trauma. Overall trauma or high betrayal trauma—where the perpetrator was someone close to the participant—had the strongest associations with DNA methylation. Two of the identified areas contained genes related to heart health and weight gain. These results suggest that trauma in early life may contribute to variability in DNA methylation and, potentially, health risks later in life.
Learn more here:
DNA methylation-predicted plasma protein levels and breast cancer risk . ![]()

Name: Dr. Vicky Stevens
Role: Laboratory Director
Vicky is one of the leaders of the Anniversary Biospecimen Collection where we are collecting blood, urine, & stool.
Favorite part of working on the Sister Study: "As a long time cancer researcher and a breast cancer survivor myself, I know how important this study is. My favorite part of working on the Sister Study is constantly witnessing the amazing dedication and effort put forward by all of you Sisters to discover causes of breast cancer and other women's health conditions."
Sister Study scientists examined how certain epigenetic predictors of protein levels in blood were associated with breast cancer. They identified several markers linked to disease risk, including associations with eight proteins that play a role in immune response. Many of the markers had stronger associations with estrogen receptor-negative tumors. The observed links between predicted protein levels and breast cancer risk contribute new evidence to the hypothesis that changes to the immune system may impact breast cancer development.
Learn more here:
DNA methylation-predicted plasma protein levels and breast cancer risk. ![]()
Earlier studies have found that the children of very young mothers had lower fertility, possibly because of socioeconomic disadvantage during childhood. In a recent Sister Study investigation, researchers explored whether women born of young mothers had worse gynecologic health. They found that compared to women with older mothers, women born of mothers younger than 25 had a higher risk of having gynecologic surgery (including bilateral oophorectomy or hysterectomy) before the age 40. There were no links between number of births and participants' mothers' ages. This study adds to prior evidence that daughters of young mothers have worse gynecologic health.
Learn more here:
Risk of major gynecologic surgery before age 40 among daughters of young mothers. ![]()
This week is National Women's Health week! The Sister Study would like to recognize our amazing team members and participants this week! We are committed to supporting the health and well-being of women every day!
This week can serve as a reminder to take steps to make your health and the health of women in your family and community a priority.
Learn more here:
National Women's Health Week 2025. ![]()
Genome-wide association studies have identified approximately 200 sites (also know as polymorphisms) associated with breast cancer risk, but the biological processes affected by these genetic variations are not well understood. In a large, pooled analysis that included 172,737 female breast cancer cases and 242,009 controls, some of them from the Sister Study, researchers identified 332 genetic regions associated with breast cancer, including 131 novel sites. For 50 of the sites, a single variant (i.e., a DNA base-pair change) was identified as being the cause of increased breast cancer risk. This included genes on the PI3K/AKT, TNF/NF-κB, p53 and Wnt/β-catenin pathways. This scientific approach helped to link inherited genetic variations with specific biological effects that may directly impact breast cancer risk; the identification of such targets is key to developing new approaches to prevention and treatment.
Learn more here:
Refining breast cancer genetic risk and biology through multi-ancestry fine-mapping analyses of 192 risk regions. ![]()
A recent Sister Study investigation examined whether hazardous chemicals found in industrial air pollution are linked to breast cancer risk. Using the U.S. Environmental Protection Agency's Toxics Release Inventory, which tracks emissions from industrial facilities, researchers examined 28 chemicals released into the air near participants' homes in the decade before the study began. They found that higher levels of certain chemicals, like nickel compounds and trichloroethylene, were associated with an increased risk of developing breast cancer later in life. However, most of the chemicals studied showed no clear link to breast cancer, suggesting that while a few specific pollutants may contribute to risk, industrial air pollution as a whole does not appear to be a major driver of breast cancer incidence. Because exposure levels among women in the Sister Study were relatively low, further research is needed to determine whether stronger associations exist in populations with a greater burden of exposure to industrial pollution and to better evaluate long-term health effects.
Learn more here:
Industrial Air Emissions and Breast Cancer Incidence in a United States-wide Prospective Cohort. ![]()
Certain genetic alterations of the BRCA2 gene are known to increase individuals' risk of several cancers, including breast and ovarian cancer. However, some BRCA2 mutations are considered 'variants of uncertain significance' because their direct impacts on risk are unknown. Scientists conducted an in-depth examination of some of these BRCA2 variants using gene-editing techniques in the laboratory to alter the DNA of human cells. By comparing the behavior of these cells to those with BRCA2 mutations that are better understood, researchers were able to classify almost all (91%) of the 'variants of uncertain significance' as pathogenic (harmful)/likely pathogenic or benign/likely benign. These classifications can be used to improve clinical management of individuals with BRCA2 variants.
Learn more here:
Functional evaluation and clinical classification of BRCA2 variants. ![]()

Introducing the Sister Study Advocate team! Cari, Nyasia, Storme, and Genesis are here to offer personalized support for our participants. As your dedicated Advocates, they're here to guide and encourage you throughout the study, helping make the process as smooth and manageable as possible. Whether you're completing questionnaires or need assistance, they're committed to ensuring your participation is both fulfilling and meaningful.
The Advocate Team is currently helping manage the 2025 Detailed Follow-Up and Annual Health Update. Don't forget to complete your questionnaires—we're here to support you every step of the way! Woman by woman...Sister by sister...Together we are making a difference.
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Siblings Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
This week is National Public Health Week! For over 20 years, Sister Study participants and their families have helped advance public health research! Every year that you generously provide more information allows investigators to better understand many chronic diseases. Every new finding helps pave the way for healthy beginnings and hopeful futures for generations to come.
The Sister Study team thanks our participants and their families for over 20 years of dedication to research!
Sisters! Beginning in October 2024, we started reaching out to ask you to complete either your Annual Health Update or your more in-depth Detailed Health Update (which is requested every three years). Please check your email or postal mail to complete your questions.
As a thank you for your dedication, we are entering all participants who complete their health update survey into a $500 gift card drawing! The earlier you submit your survey, the better your chances, as you'll be entered into each monthly drawing throughout the 2024-2025 health update collection period.
- Please note: approximate odds of winning are 1 in 5,000 to 1 in 48,000 depending on when you complete your health update.
A recent paper titled "Hair straightener use during adolescence may increase risk of fibroids" published by several Sister Study investigators was chosen as a Paper of the Month by the NIEHS!
NIEHS researchers recently published a study of the association between chemical hair straightener/relaxer use and uterine fibroids among Black women. They found that frequent use of hair straighteners in early adolescence (ages 10-13 years) was linked to a higher risk of developing fibroids before age 36. The link was potentially stronger for women born between 1928-1945 and 1965-1974, possibly due to changes in hair straightener product formulations over time. A weaker connection was found among women born between 1955-1964, possibly due to the popularity of wearing Afros and other natural hairstyles in the 1970s.
Similar positive associations were observed among non-Hispanic White women, despite lower usage rates. This study highlights concerns over endocrine-disrupting and carcinogenic chemicals found in hair products and their potential role in hormone-related diseases.
Learn more here:
Hair straightener use during adolescence may increase risk of fibroids. ![]()
Trauma in early life (before age 18) affects overall stress and is thought to be associated with increased risk of adverse pregnancy outcomes, such as gestational diabetes and hypertensive disorders of pregnancy (HDP). In the Sister Study cohort, we found that 47% of participants reported at least one type of early-life trauma and 31% reported high multiple early-life traumas. Women reporting physical trauma had the highest risk of gestational diabetes and HDP. Relative to low trauma, we also observed an elevated risk of gestational diabetes and HDP for women reporting high multiple early-life traumas. This work suggests the type and quantity of co-occurring early-life traumas does matter and that it is important to consider patterns of traumatic experiences when studying adverse pregnancy outcomes.
Learn more here:
Association of Early-life Trauma With Gestational Diabetes and Hypertensive Disorders of Pregnancy. ![]()
In this NIH article, Dr. Eric Topol discusses AI's transformative potential in medicine, highlighting its ability to revolutionize diagnostics and patient care. He explains how AI—powered by advanced graphics processing units—an detect medical conditions, such as cancer and heart disease, often more accurately than humans.
Learn more here:
Topol Discusses Potential of AI to Transform Medicine. ![]()
As February, National Cancer Prevention Month, comes to an end, we want to share our appreciation for our Sister Study participants.
According to the NIH, in 2024, roughly two million people were diagnosed with cancer in the United States. Nearly half of those diagnoses are breast, prostate, lung, pancreas, or colon cancers. And yet, more than 40 percent of all cancer diagnoses can be linked to a preventable cause.
In 2024, an estimated 310,720 women and 2,790 men were diagnosed with breast cancer, which makes it among the most common cancer diagnosis.
National Cancer Prevention Month focuses on the things we can control to lessen our odds of developing cancer. Five of the top recommendations for lessening our risk include:
- Regular exercise
- Maintaining a healthy weight
- Eating healthy foods
- Quitting or never starting smoking
- Limiting alcohol use
To learn more about cancer prevention and statistics in the United States, please reference these AACR and NCI articles.
AACR National Cancer Prevention Month. ![]()
NCI Cancer Stat Facts. ![]()
Artificial Intelligence (AI) can improve diagnostics, drug development, and patient care but may also perpetuate bias, especially when trained on data that lacks diversity. In this NIH article, Dr. Maia Hightower discusses the potential and challenges of using AI in healthcare.
Learn more here:
Hightower Discusses Responsible AI in Health Care . ![]()
A publication led by Sister Study investigators was recently recognized as a NIEHS Intramural Paper of the Month! The study, titled "Air pollution exposure may be linked to ovarian cancer," sheds light on the potential connection between environmental factors and women's health. We are incredibly proud of this achievement and the impact it has on ongoing research!
Check out their groundbreaking work, along with the other recognized papers, using the link below:
Air pollution exposure may be linked to ovarian cancer. ![]()

Dr. Katherine (Katie) Pullella recently joined the Sister Study team to conduct research on cancer epidemiology and environmental health. She earned her PhD in Nutritional Sciences from the University of Toronto in 2024, where she studied the relationship between arsenic exposure and breast cancer risk in the Canadian population. Now a postdoctoral fellow in Dr. Alexandra White's Environment and Cancer Epidemiology Group at NIEHS, Katie's first Sister Study project is to explore how levels of arsenic in community water sources may (or may not) impact breast cancer risk. She has big plans for future Sister Study projects aimed to better understand how environmental exposures can impact cancer development, with the ultimate goal of informing cancer prevention strategies and public health interventions.
The Sister Study contributed data to a large study of variants in established breast cancer risk genes (ATM, BARD1, BRCA1, BRCA2, CDH1, CHEK2, PALB2, RAD51C, and RAD51D) and ductal carcinoma in situ (DCIS), a pre-invasive form of breast cancer. Between 4.6% - 6.5% of women with DCIS were found to have a mutation in one of these "pathogenic" genes. Women with DCIS were less likely to have mutations in BRCA1, BRCA2, and PALB2 than women with invasive breast cancer, but mutations in ATM, BRCA1, BRCA2, CHEK2, and PALB2 were strongly associated with an increased risk of DCIS. Approximately 23% of women with DCIS who had a pathogenic mutation developed breast cancer in the second breast within 15 years. This research suggests that multigene panel testing may be appropriate for women with DCIS to help guide clinical decision-making.
Learn more here:
Pathogenic Variants in Cancer Susceptibility Genes Predispose to Ductal Carcinoma In Situ of the Breast. ![]()
Carotenoids are dietary compounds found in fruits and vegetables. High levels of carotenoids in blood have been shown to be associated with decreased risk of several diseases. Sister Study investigators sought to better understand the role of genetic factors in determining the relationship between fruit and vegetable consumption and carotenoid concentrations in blood to gain insights in how to better prevent chronic diseases. This was investigated using data from 519 postmenopausal women who had previously been genotyped and had their blood carotenoid levels assessed. We found that genetic variants near the beta-carotene oxygenase 1 (BCO1) gene were associated with lutein and zeaxanthin levels, but no other strong genetic predictors were identified for any of the other 4 carotenoids (alpha-carotene, beta- carotene, cryptoxanthin, or lycopene).
Several years ago, we asked some of the younger Sister Study participants to allow us to obtain and read their previous mammograms. The mammograms we received were used to study changes in breast density over time in relation to breast cancer risk. The mammography study included 323 women who had been diagnosed with breast cancer before age 60 and 899 women without breast cancer as of age 60. Women's breasts tend to decrease in density as women age, but these changes happen at different rates across women. We found that having stable or increasing mammographic density was associated with increased breast cancer risk, compared to women who lost breast density over time. These findings may help guide clinical recommendations for incorporating mammographic density trajectories in risk assessments, including support for increased monitoring of women who do not experience breast density loss over time.
Known genetic risk variants for epithelial ovarian cancer only account for 40% of inherited risk In a large, pooled analysis that included data from the Sister Study, investigators examined whether the number of copies of specific genetic markers carried by an individual (referred to as "copy number variants" or "CNVs") is related to her risk of developing ovarian cancer. CNVs at established breast and ovarian cancer-related genes, including BRCA1, RAD51C and BRCA2 were associated with ovarian cancer risk, as were 4 rare CNVs in novel locations. These results indicate that CNVs in these regions may contribute additional risk beyond what we already knew about these genes and identify possible targets for clinical genetic testing.
Learn more here:
Copy Number Variants Are Ovarian Cancer Risk Alleles at Known and Novel Risk Loci. ![]()
Since we began analyzing the data provided by our generous Sister Study sisters, our researchers have published over 300 scientific papers! These findings contribute to improvements in our understanding of the environmental and genetic causes of breast cancer and other important issues in women's health. We are proud of what we have accomplished together with our study sisters!
Thank you for sticking with us!
To view our study findings:
Sister Study Research Articles. ![]()
Childhood adversity has been associated with metabolic syndrome and type 2 diabetes risk in adulthood. A Sister Study investigation considered the role of race and ethnicity in these relationships and whether the link with type 2 diabetes was due to metabolic syndrome. Metabolic syndrome refers to having a combination of conditions including obesity—especially abdominal obesity—high cholesterol or triglyceride levels, high blood pressure and high blood sugar. More than 3,000 women reported new type 2 diabetes diagnoses since enrollment, including 2,479 non-Hispanic White women, 461 Black / African American women, and 281 Latina women. About half of study participants reported a traumatic childhood event such as being in an accident, or experiencing a major storm, family illnesses or deaths, or sexual or physical abuse. Having a traumatic childhood event was associated with a 13% higher risk of type 2 diabetes, with the strongest associations seen among Latina women (64% increase). This relationship was partially explained by increased prevalence of metabolic syndrome among those with traumatic childhood events.
A large collaborative research project sought to answer the question: is the optimal approach to breast cancer screening for women with ATM, CHEK2, and PALB2 pathogenic variants? These are genes that are strongly linked with increased breast cancer risk, although the risks are not as great as they are for BRCA1/2. The researchers estimated that annual mammography from age 40 to 74 years reduced breast cancer mortality by 36% to 39% in women with these variants. Screening via annual magnetic resonance imaging (MRI) before age 40, followed by annual screening with both MRI and mammography after age 40 was estimated to reduce breast cancer mortality by 54%- 60%. However, the use of both annual MRIs and mammographies before age 40 did not meaningfully reduce mortality, and also increased the number of false-positive screenings. This modeling analysis, which includes data from Sister Study participants, suggests that starting MRI screening before age 40 may substantially reduce breast cancer mortality for women with moderate- to high-risk pathogenic variants for breast cancer.
Learn more here:
Good Housekeeping: Can Dying Your Hair Raise Your Risk for Breast Cancer? Experts Explain. ![]()
Breast Cancer Screening Strategies for Women With ATM, CHEK2, and PALB2 Pathogenic Variants: A Comparative Modeling Analysis. ![]()
Outdoor air pollution has been linked to various cancers, including lung, breast, and uterine cancers, but its association with ovarian cancer, a gynecologic cancer with poor survival, has been less studied. In the Sister Study, we estimated participants' exposure to air pollutants—nitrogen dioxide (NO2), particulate matter (PM2.5), and ozone (O3)—based on residential addresses. Our analysis found that higher NO2 levels, which are often an indication of high traffic pollution, were linked to an increased risk of ovarian cancer. The relationship between ovarian cancer and exposure to PM2.5 or O3 was less consistent. These findings suggest that air pollution, particularly NO2, may play a role in ovarian cancer development.
Learn more here:
Outdoor Air Pollution Exposure and Ovarian Cancer Incidence in a United States–Wide Prospective Cohort Study. ![]()
One of the main aims of the Sister Study is to identify environmental risk factors for breast cancer. To achieve this, we learn from and build upon earlier studies of chemicals that are suspected to be harmful but are not established carcinogens. Chemicals of current concern are the so called "forever chemicals": per- and polyfluoroalkyl substances (PFAS) that are found in water, air, fish, and soil as well as many different consumer and commercial products .PFAS have been found in the blood of people all over the world. In preparation for investigating PFAS in the Sister Study, several investigators reviewed the results of prior studies. Some of these showed that higher blood concentrations of certain PFAS may be associated with increased future breast cancer risk, but the authors noted inconsistencies across studies and identified some major limitations. They concluded that the association between PFAS exposure and breast cancer is not yet established and identified some areas where additional or more in-depth research is needed.
Learn more here:
Exposure to per- and polyfluoroalkyl substances and breast cancer risk: a systematic review and meta-analysis of epidemiologic studies. ![]()
We know that breast cancer risk can be influenced by both genetic and non-genetic factors, but our understanding of the combined effects of these various factors is limited. The Sister Study recently contributed to a study that used data on (1) rare, pathogenic variants of genes associated with high risk of breast cancer (e.g., BRCA1, BRCA2, and CHEK2), (2) more common genetic mutations, and (3) various epidemiologic factors to predict breast cancer risk. The authors illustrate how epidemiologic risk factors (including reproductive history, lifestyle, and clinical factors) can help determine who has the highest risk among women who are known to be at increased risk due to their genetic profile. As an example, having a mutation in the CHEK2 gene was highly predictive of risk overall (>20% lifetime risk), but adding information on other genetic and non-genetic factors could further divide CHEK2 carriers into those who would (or would not) most benefit from regular MRI screening. More details on specific combinations of risk factors are provided in the published manuscript.
Learn more here:
Development of a Breast Cancer Risk Prediction Model Integrating Monogenic, Polygenic, and Epidemiologic Risk. ![]()
Serum iron levels can be important contributors to health outcomes, but it is not often feasible to measure blood iron in all study participants. Researchers examined whether factors measured in the Sister Study questionnaires, such as diet, supplement use, recency of blood donation, and medical conditions, could be used to predict iron status. However, none of the examined factors were strongly predictive. Any future prediction models should consider unmeasured factors, including but not limited to: concurrent environmental exposures, temporal factors, and genetic variations in absorption and storage.
Learn more here:
Development and validation of a prediction model for iron status in a large U.S. cohort of women. ![]()
Experience of traumatic events—including sexual, physical, or emotional abuse, and financial hardships—is thought to influence breast cancer risk, but such events rarely occur in isolation, and little is known about how co-occurring traumas, particularly during early life, may impact breast cancer risk. Sister Study participants reported whether they experienced certain traumatic experiences during childhood and adolescence. Using that data, we identified six distinct patterns of early-life trauma in the cohort. About half of all Sister Study participants disclosed at least one traumatic experience before age 18. We reported that experiencing either sexual trauma and household dysfunction or medium levels of early-life trauma was suggestively associated with greater risk of developing breast cancer compared to experiencing low levels of early-life trauma. Furthermore, breast cancer risk due to early-life trauma appeared lower among participants who reported constant childhood social support. This research suggests that different types of early-life traumatic experiences may contribute to various levels of risk of breast cancer.
Learn more here:
Latent class models of early-life trauma and incident breast cancer. ![]()
October is Breast Cancer Awareness Month and we at the Sister Study would like to join our participants and friends of the study to remember those affected by breast cancer. With our ongoing research, we honor those we have lost and those who continue to fight against breast cancer. We are grateful to those of you who participate in research like the Sister Study so we can work together toward solutions. Thank you.
Sister Study investigators examined how geography and neighborhood-level environmental and socioeconomic factors may contribute to breast cancer incidence. The lowest breast cancer rates were observed in the South and Southeast US, with a greater rates in the Northwest, Midwest, and Northeast. Of the measures considered, nitrogen dioxide (NO2; an indicator of traffic-related air pollution), light at night, and the area deprivation index (a measure of neighborhood level socioeconomic factors) were the most important residential-level predictors of breast cancer risk overall. These plus measures of the chemical composition of air pollution (specifically fine particulate matter, PM2.5) and greenspace were strong predictors of estrogen receptor positive breast cancer. These results support a role of environmental exposures in breast cancer incidence and suggest variability by breast cancer subtype.
Learn more here:
Understanding the role of environmental and socioeconomic factors in the geographic variation of breast cancer risk in the US-wide Sister Study. ![]()
Uterine fibroids and endometriosis are two non-cancerous gynecological conditions that share some symptoms. Both conditions are influenced by hormones such as estrogen and there is some evidence they may be associated with ovarian cancer risk. Some women with these conditions have their uterus removed (hysterectomy), which could also impact their ovarian cancer risk. In the Sister Study, 34% of 40,928 eligible participants have reported a fibroid diagnosis, 13% reported having had endometriosis, and 7% reported having both. 20% of participants have had a hysterectomy. Women with fibroids had a 65% increased rate of developing ovarian cancer, compared to women without fibroids. Among women with fibroids, those who had a hysterectomy were less likely to develop ovarian cancer than those who did not. History of endometriosis was not associated with risk. Studying the joint effects of fibroids, endometriosis and hysterectomies adds to our understanding of ovarian cancer and may help inform decisions about how women with fibroids, endometriosis, and hysterectomies are treated and monitored.
Learn more here:
The independent and joint associations of hysterectomy and uterine fibroids or endometriosis with ovarian cancer incidence: results from a US-based cohort. ![]()
As we commemorate 20 years of the Sister Study, we are launching a new Anniversary Biospecimen Collection (ABC) initiative to obtain blood, urine, and stool samples from our participants. The samples you provided when you joined the study have provided valuable insights related to breast cancer and other health outcomes, but they only provide a snapshot of a single point in time, and we know that much has changed for each of you over the past 20 years.
Right now, we are starting with a small group of women to test our processes and make sure everything is working. We are planning to expand to a larger group in the near future and will reach out to you when it's your turn to participate. So far, 100% of the recruited participants have committed to providing all 3 biospecimens. We are so heartened by this enthusiastic response! These new samples will help Sister Study researchers better study how changes in exposures and biological processes over time affect disease risk, quality of life, and for those who have been diagnosed with breast cancer, health and survival after diagnosis.
We hope you will say yes when we call on you to participate in the 20th Anniversary Biospecimen Collection!
Most papers looking at genetic risk factors for breast cancer compare genetic profiles of women with and without breast cancer. However, comparing genetic factors between women with different types of breast cancer may reveal differences in the causes of specific breast cancer subtypes. Results from a large pooled analysis that included Sister Study participants identified several potentially important genetic differences between Luminal A breast cancers (estrogen receptor [ER] positive and/or progesterone receptor [PR] positive and human epidermal growth factor receptor-2 [HER2] negative) and triple-negative breast cancers (ER-negative, PR-negative, HER2-negative). The authors used the results to develop genetic risk scores that may be useful for predicting breast cancer subtype.
Learn more here:
Case-Case Genome-Wide Analyses Identify Subtype-Informative Variants That Confer Risk for Breast Cancer. ![]()

The Sister Study is once again hosting undergraduate- and graduate-level researchers as part of the NIH summer internship program. This year's Sister Study projects include studies examining the following: whether personal talc use is associated with lung cancer risk (Maya Desmukh), if age at puberty is associated with ovarian cancer risk (Sydney Lash), the relationship between vitamin D biomarker levels and epigenetic markers (Mitali Joshi), if the use of hair straighteners/relaxers is associated with the risk of non-hormonal cancers (Jared Bailey), how to predict who experiences pregnancy complications (Daniel Goldblatt), whether genetic risk scores for breast cancer are associated with anti-depressant use (Riddhik Basu), and an investigation of gene-by-gene interaction in relation to risk of young-onset breast cancer (Marvel Hanna). The students will be presenting their work at NIEHS at the end of July and many will go on to publish their work in scientific journals.
Industrial facilities across the United States release millions of pounds of toxic chemicals, including metals, that may be associated with adverse health outcomes. In a sample of 1556 women who identified as non-Hispanic Black (33%) or non-Hispanic White (67%), Sister Study investigators showed that living near metal-releasing facilities was not associated with higher toenail metal concentrations overall. However, Black women were more likely to reside near metal emitting facilities and among Black women, higher chromium emissions were associated with higher toenail chromium levels. There was also a strong link between exposure to lead and lead in toenails among Black women residing in socioeconomically deprived areas. No associations were observed among White participants.
Learn more here:
Residential proximity to toxic metal-emitting industrial sites and toenail metal concentrations in a United States-wide prospective cohort. ![]()
The age at which girls go through puberty can vary considerably and has been linked to health outcomes later in life. For example, earlier puberty is associated with an increased risk of developing breast cancer. Information collected from Sister Study participants was recently included in a study of the genetic factors associated with age at puberty onset. Study authors identified more than 1,000 genetic variants potentially linked to pubertal age. These results are being used to identify some of the key genes and biological pathways that impact puberty and its links to disease later in life.
Learn more here:
Understanding the genetic complexity of puberty timing across the allele frequency spectrum. ![]()
Hypertension (high blood pressure) has been linked to stress from social factors, including discrimination. In the Sister Study, participants reported whether they had ever perceived job discrimination based on their race, gender, age, sexual orientation, or health status: 11% reported job discrimination in the past 5 years, with those who self-reported poor health or inclusion in minoritized groups (e.g., based on race/ethnicity or sexual orientation) more likely to report job discrimination. Overall, 19% of women reported being diagnosed with hypertension during follow-up, and women who experienced job discrimination more likely to develop hypertension. Interventions to address job discrimination could potentially improve workplace equity and health.
Learn more here:
Multiple forms of perceived job discrimination and hypertension risk among employed women: Findings from the Sister Study. ![]()

Dazhe Chen earned his PhD in epidemiology from the University of North Carolina at Chapel Hill in 2022 where he worked with Dr. Sandler to study heart disease risk in oil spill clean-up workers following a major oil spill in the Gulf of Mexico. Following graduation, he joined Dr. Dale Sandler's group at NIEHS as a postdoctoral fellow . Dr. Chen's research focuses on the identification of modifiable risk factors for autoimmune disorders and other chronic diseases with an eye towards disease prevention. In his first Sister Study research project, he examined the association between early-life pesticide exposures and inflammatory bowel disease. In future projects, Dr. Chen plans to use Sister Study data to explore other modifiable risk factors for inflammatory bowel disease, including the use of specific medications, and to explore possible links between autoimmune diseases and cancer.
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. On National Sisters Day, we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
Crohn's disease and ulcerative colitis, collectively known as Inflammatory Bowel Disease (IBD), are autoimmune diseases of the digestive tract that have few known risk factors. Many pesticides are toxic to the human immune system and may contribute to autoimmunity, and children are especially vulnerable to pesticide exposures. Pesticides are also thought to affect the gut microbiome and changes in the microbiome have been linked to other digestive diseases. In a newly published Sister Study paper, researchers explored the association between pesticide exposure during childhood and adolescence and the incidence of IBD. Women who were directly exposed to pesticides had higher rates of IBD, especially those who personally used pesticides. This study provides novel evidence suggesting that early-life pesticide exposure may contribute to the development of iIBD. Further research is needed to investigate the association in other populations.
Learn more here:
Childhood and adolescent residential and farm pesticide exposures and inflammatory bowel disease incidence in a U.S. cohort of women. ![]()
In a collaborative project that included information from Sister Study participants, researchers studying genetic risk factors for ovarian cancer conducted investigations of what variants might play a role in causing specific types ("histotypes") of ovarian cancer. The researchers confirmed the importance of 27 genetic regions that had been reported in prior studies and also identified several new regions or interest. Each of these novel regions was investigated in great detail, including consideration of how each genetic variant may affect gene regulation, transcription, and expression. This work aids in our understanding of the direct links between genetic mutations and disease risk.
Learn more here:
Integrative multi-omics analyses to identify the genetic and functional mechanisms underlying ovarian cancer risk regions. ![]()
The Sister Study contributed to a large genetic study of breast cancer that included 40,138 women with African ancestry (18,034 cases, 22,104 non-cases). In the study, 12 genetic variants were identified as being strongly associated with breast cancer risk. This included a rare mutation in the ARHGEF38 gene and a more common variant on chromosome 2 that was specifically associated with triple-negative breast cancer. Based on these results, the investigators created a genetic risk score that more successfully predicted risk among women of African ancestry than previous genetic risk scores that had been developed using data primarily from women of European ancestry.
Learn more here:
Genome-wide association analyses of breast cancer in women of African ancestry identify new susceptibility loci and improve risk prediction. ![]()
Tea and coffee are widely consumed beverages, and both have previously been found to have different relationships with certain cancers. The Sister Study was one of 15 studies contributing to the Biliary Tract Cancers Pooling Project, a collaborative effort put together to investigate risk factors for gallbladder and bile duct cancers. Study investigators found that Individuals who drank tea had lower incidence of gallbladder and intrahepatic bile duct cancer. The study was not able to determine if this association varied for different types of tea because not every contributing study had that information. Coffee consumption was positively associated with gall bladder cancer, but not the other biliary tract cancers. Further research is warranted to replicate the observed positive association between coffee and gall bladder cancer.
Learn more here:
Association of tea and coffee consumption and biliary tract cancer risk: The Biliary Tract Cancers Pooling Project. ![]()
Measures of biological aging have been linked to some chronic diseases and cancers. We explored whether the use of chemical hair products—such as dyes and straighteners—is related to a genomic marker of biological age known as "epigenetic age'. In previous research from the Sister Study, we identified positive associations between the use of chemical hair products and breast, ovarian, and uterine cancers. However, in this study we found negligible associations between these products and epigenetic age. This suggests a need for further research to identify the biological processes underlying the potential link between chemical hair products and cancer.
Learn more here:
Associations between use of chemical hair products and epigenetic age: Findings from the Sister Study. ![]()
Women with African ancestry are underrepresented in genetics research. In a large study that included Sister Study participants with African ancestry, researchers examined the links between breast cancer risk and how genes are read and transcribed into proteins. Models for predicting gene transcription were built using data from normal breast tissue, and then applied to generate estimates of gene expression in 18,034 breast cancer cases and 22,104 controls, all of whom had African ancestry. Six genes were identified as being associated with breast cancer risk, including four genes not previously reported (CTD-3080P12.3, EN1, LINC01956 and NUP210L). Most of these genes showed a stronger association with risk of estrogen-receptor (ER) negative or triple-negative than ER-positive breast cancer. These genes have low frequency in the population, are associated with very small increases in risk, but his study sheds new light on the genetic basis of breast cancer and highlights the value of conducting research among women with African ancestry.
Learn more here:
Using genome and transcriptome data from African-ancestry female participants to identify putative breast cancer susceptibility genes. ![]()
With collaborators at the Environmental Protection Agency, we studied whether measures of neighborhood greenery were associated with body size among Sister Study participants living in or near certain US cities for which detailed land-use and greenery measures were available. We found that more tree cover was associated with a decreased odds of being overweight or obese. Herbaceous cover (including grasses, shrubs, and other plants) was also associated with lower odds of being overweight or obese in arid climates (Western states, excluding the Pacific coast), but with higher odds in temperature climates (Southern states). These findings add to a growing body of evidence that greenery design in urban planning can support public health.
Learn more here:
Types and spatial contexts of neighborhood greenery matter in associations with weight status in women across 28 U.S. communities. ![]()
Researchers have identified many genetic variants associated with breast cancer risk. The combined effects of these variants can be summarized using something called a polygenic risk score (PRS). The idea is that many genetic variants are individually associated with very small increases in risk, but their combined effects may be a powerful tool for identifying individuals at high risk of developing breast cancer. However, most PRSs were developed in women of European ancestry and are less accurate predictors in women of African ancestry. Using data from 9,235 women with breast cancer and 10,184 women without breast cancer, including many participants from the Sister Study and Two Sister Study, a team of researchers set out to develop a better PRS for women with African ancestry. The new PRS was better able to predict breast cancer occurrence among women of African ancestry, compared to previous.
Learn more here:
Polygenic risk scores for prediction of breast cancer risk in women of African ancestry: a cross-ancestry approach. ![]()
Some fruits and vegetables as well as vitamin supplements contain carotenoids, such as α-carotene, β-carotene, β-cryptoxanthin, lutein/zeaxanthin, and lycopene, which may protect against chronic diseases including cancer. In a newly published Sister Study paper, we evaluated associations between carotenoids and biological markers of inflammation and oxidative stress, which is a measure of the balance between antioxidants and oxidative damage in human tissues. Some carotenoids measured in blood had an inverse association with oxidative stress measures, meaning that they may have antioxidant effects. Others were inversely associated with both inflammation and oxidative stress measures. β-carotene supplements, but not dietary carotenoid estimates, were associated with lower levels of inflammation and oxidative stress. This work helps to identify the role of individual nutrients in maintaining and promoting good health.
Learn more here:
Association of dietary and plasma carotenoids with urinary F2-isoprostanes. ![]()
One consequence of climate change may be increased ultraviolet (UV) light exposure. UV exposure is an established risk factor for skin cancer, but as a major source of vitamin D it may also help protect against some cancers. Sister Study investigators used statistical models to estimate participants' UV exposure level based on their addresses at enrollment. Estimated UV exposure was not associated with breast cancer risk overall, but those with higher estimated UV levels were less likely to develop estrogen receptor negative disease. These results provide evidence that higher UV exposure may help prevent some types of breast cancer, possibly due to the link between UV and vitamin D.
Learn more here:
Residential ultraviolet radiation and breast cancer risk in a large prospective cohort. ![]()
CancerNetwork® spoke with Dr. Fumiko Chino, Assistant Attending Radiation Oncologist at Memorial Sloan Kettering Cancer Center regarding results of a recent Sister Study publication from the Journal of Clinical Oncology which highlighted the association of ovarian cancer with talcum powder (talc) use. Dr. Chino shared her expertise in why having a cohort population study like Sister Study is so important in enhancing cancer outcomes. She says, "These types of studies require a lot of effort and require a lot of time and dedication from the volunteers who are enrolled. My main message when we get good information from a study like this cohort study is that it is my profound gratitude for the women who enrolled on the study and did these sequential surveys. They gave a lot of themselves, sharing some of their personal information to try to help the larger good." The study found that of the 50,884 women enrolled, there was a positive correlation between ovarian cancer and genital talc use.
Learn more here:
Ovarian Cancer Linked to Genital Talcum Powder Use. ![]()
Ovarian cancer is a rare cancer, with a lifetime risk of approximately 1% in US women. This makes it a very difficult disease to study and the Ovarian Cancer Cohort Consortium (OC3) ![]() was established to allow researchers to pool together data from 23 large cohorts from all over the world, including the Sister Study. The consortium currently includes 1.3 million women, among whom 7,314 developed ovarian cancer since joining one of the studies. Sister Study investigators previously led OC3 projects examining associations between genital powder use and ovarian
was established to allow researchers to pool together data from 23 large cohorts from all over the world, including the Sister Study. The consortium currently includes 1.3 million women, among whom 7,314 developed ovarian cancer since joining one of the studies. Sister Study investigators previously led OC3 projects examining associations between genital powder use and ovarian ![]() and uterine
and uterine ![]() cancer, and have contributed to many other published and ongoing projects.
cancer, and have contributed to many other published and ongoing projects.
Learn more about the OC3 here:
Ovarian Cancer Cohort Consortium. ![]()
Collaborators at the Pennsylvania State University College of Medicine used clinical information shared by Sister Study participants who had been diagnosed with stage I, II or III breast cancer to determine how exercise affects response to breast cancer treatments. Of the 180 women who were prescribed neoadjuvant (i.e., pre-surgical) chemotherapy, 45 (25%) achieved a pathological complete response, meaning no residual cancer remained after treatment. In an assessment of how pre-diagnosis physical activity levels affected treatment and response, the researchers did not see any association between physical activity levels and participants' response to treatment or their ability to complete their prescribed course of treatment. More research is needed to better understand what factors influence participants' tolerance and response to chemotherapy.
Learn more here:
Pre-diagnosis physical activity and chemotherapy treatment response in breast cancer survivors . ![]()
This study examines the association between the use of intimate care products, such as genital talc and douching, and the risk of hormone-related cancers such as ovarian, breast, and uterine cancers. Genital talc use was found to be associated with the risk of ovarian cancer and the association was particularly strong among women who used talc frequently or during periods of significant hormonal changes or reproductive activity. These findings contribute significant insights into the ongoing debate about the safety of intimate care products and underscore the need for further research and potential reevaluation of these products' safety.
Learn more here:
Intimate Care Products and Incidence of Hormone-Related Cancers: A Quantitative Bias Analysis. ![]()
Some environmental exposures follow seasonal patterns, and failing to account for seasonal effects may introduce measurement error into studies that rely on biological samples to estimate exposure. Most Sister Study participants provided toenail samples when they enrolled in the study - these have been used to study metals and other elements. A detailed evaluation of element concentrations across the calendar year revealed that there were seasonal trends in toenail concentrations of iron, aluminum, vanadium, chromium, manganese, cobalt, arsenic, molybdenum, cadmium, tin, and lead, all of which highest around mid-August. These results highlight the importance of accounting for season when using samples taken at a single time-point to estimate long-term exposure levels.
Learn more here:
Seasonal patterns in trace elements assessed in toenails. ![]()
A high body mass index (BMI) is known to be associated with decreased risk of breast cancer before menopause, but increased risk after menopause. In a collaborative project that included the Sister Study and 15 other cohorts with information on women younger than 55, researchers tried to better understand when this reversal occurred. The results indicated that BMI was consistently inversely associated with breast cancer throughout the ages of interest, implying that BMI is not associated with increased breast cancer risk until some time after age 55.
Learn more here:
BMI and breast cancer risk around age at menopause. ![]()
Women with a history of breast cancer are known to have an increased risk for developing heart disease and other chronic diseases later in life, but the reasons for this are not always well understood. A newly published Sister Study investigation evaluated whether changes in blood composition, as measured by the relative frequency of certain cell types, might offer some clues. Using blood samples collected from 410 women enrolled in the Sister Study, including 185 breast cancer survivors, investigators found that breast cancer survivors had lower relative percentages of specific types of white blood cells, including eosinophils, total CD4+ helper T cells, and memory B cells, than women without breast cancer, and higher relative percentages of circulating naive B white blood cells. There was some evidence that these changes were related to specific breast cancer treatments, as having had radiotherapy was associated with decreased total CD4+ T cell levels, while chemotherapy was associated with increases in naive B cell levels. These findings help elucidate some of the long-term health consequences of breast cancer and its treatment and someday could help identify women who might benefit from more frequent or focused health follow-up after treatment.
Learn more here:
Circulating Leukocyte Subsets Before and After a Breast Cancer Diagnosis and Therapy . ![]()
Many every day personal care products contain chemicals that have the potential to disrupt hormone pathways or have been associated with health risks. Use of these products often starts during adolescence, when rapidly developing breast tissue may be more susceptible to the effects of harmful environmental chemicals. In a newly published Sister Study paper, researchers examined whether using common products during this critical period may affect women's breast cancer risk. Overall, there were no consistent patterns in the types of products that were associated with breast cancer. The types and frequency of products used varied by race and ethnicity. Among Black and Hispanic women, frequent nail polish-related products and perfume use were possibly associated with increased likelihood of developing breast cancer. Frequent use of lipstick, nail products, pomade, perfume, makeup remover, and acne/blemish products during adolescence were also potentially associated with breast cancer risk in at least one racial/ethnic group. More research is needed to confirm these novel findings.
Learn more here:
Personal Care Product Use during Puberty and Incident Breast Cancer among Black, Hispanic/Latina, and White Women in a Prospective US-Wide Cohort . ![]()
Sister Study investigators examined the associations between two measures of air pollution exposure and uterine cancer. Participants' exposure to particulate matter less than 2.5 µm in diameter (PM2.5) and nitrogen dioxide (NO2) were estimated for home addresses using monitoring and other data. Results indicated that an increase of 5 parts per billion of NO2 was associated with a 23% increase in the rate of uterine cancer, with even stronger associations seen among participants living in urban areas (53% increase). PM2.5 was not associated with uterine cancer. These findings add further evidence that NO2, a marker of vehicular traffic exposure, has important long-term health consequences, and support the need for policy and other interventions designed to reduce air pollutant exposure.
Learn more here:
Outdoor air pollution exposure and uterine cancer incidence in the sister study . ![]()
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Siblings Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
Fibroids and endometriosis are benign conditions of the uterus that share some features with cancer. Sister Study investigators examined whether breast cancer was more common in women with these conditions. The results showed that fibroids were positively associated with breast cancer rates, with potentially stronger associations among Black participants and women who had had a hysterectomy. Endometriosis was not associated with breast cancer. Evaluating women's fibroid history may be useful for breast cancer risk prediction (and screening decisions).
Learn more here:
Association of fibroids, endometriosis, and gynecologic surgeries with breast cancer incidence and hormone receptor subtypes. ![]()
Iron levels may be important markers of health and can be measured in toenails more easily than blood. However, very few studies have compared blood and toenail iron levels. In a sample of 146 Sister Study participants, investigators found that toenail iron measures were not correlated with blood measures. This implies that the iron found in toenails may be from a different source or reflect a different time period than iron found in blood.
Learn more here:
Toenail and serum levels as biomarkers of iron status in pre- and postmenopausal women: correlations and stability over eight-year follow-up. ![]()
The Sister Study contributed information to a large study of genetic risk factors for breast cancer among women with African ancestry. This large collaborative analysis made use of results from both family-based and non-family-based studies of breast cancer. The study's most novel finding was the identification of specific genetic variants on the third chromosome that were strongly associated with estrogen receptor negative breast cancer. These variants are thought to play a role in regulating protein levels in mammary (breast) tissues.
Learn more here:
Novel breast cancer susceptibility loci under linkage peaks identified in African ancestry consortia. ![]()
Many Sister Study participants take dietary supplements, including vitamin D and calcium, but the health impacts of doing so are not fully understood. In a recent analysis of more than 13,000 women who were premenopausal at enrollment, we examined whether vitamin D and calcium intake was associated with timing of "natural" menopause (i.e., when menstrual cycles stop without surgical or medical interventions). With the possible exception of combined use of a multivitamin plus a vitamin D supplement, which was associated with slightly earlier age at menopause, none of the vitamin D or calcium intake measures had a meaningful association with age at menopause.
Learn more here:
Vitamin D status and supplementation, calcium supplementation, and timing of natural menopausey. ![]()
Exposure to air pollution can be approximated by linking addresses to maps generated from air monitoring data and other geographic information. In a new Sister Study investigation of the association between air pollution and Parkinson's disease, researchers found that higher exposure to nitrogen dioxide (NO2) was positively associated with the development of Parkinson's disease. NO2 air pollution primarily comes from burning fuel, so levels are higher in areas with high traffic. Exposure to fine particulate matter with a diameter ≤2.5 µm (often referred to as PM2.5), a type of air pollution associated with respiratory diseases and some cancers, was not associated with Parkinson's disease in this study.
Learn more here:
Air Pollutants and Risk of Parkinson's Disease among Women in the Sister Study. ![]()
The Sister Study was included in a pooled analysis assessing how reproductive and hormonal factors may be related to thyroid cancers among women. Among 1,000,000 women, 2,142 of whom developed thyroid cancer, the following factors were positively associated with thyroid cancer risk: younger age at menarche, menopause before age 40 or after age 54, ever use of menopausal hormone therapy, history of hysterectomy or bilateral oophorectomy, short-term (versus long-term) oral contraceptive use, and being premenopausal. Number of births and lifetime number of ovulatory cycles were not associated with risk. This large study provides evidence that reproductive and hormonal factors may contribute to thyroid cancer risk in women.
Learn more here:
Association of hormonal and reproductive factors with differentiated thyroid cancer risk in women: a pooled prospective cohort analysis. ![]()
A recent Sister Study paper explored how everyday beauty, hygiene, and skincare products could be linked to breast, ovarian, and uterine cancers. The study found that certain combinations of products, particularly in hygiene and beauty categories, might increase the risk for ovarian or breast cancers. Interestingly, skincare product combinations were linked to lower risks for breast cancer. The Sister Study questionnaire asked about types of products, such as shampoos or lotions, but did not include questions about specific brands or formulations. Even so, this research provides new insights into a possible impact of our daily personal care product choices on our health and suggests the need for more research on the health effects of these everyday products.
Learn more here:
Use of personal care product mixtures and incident hormone-sensitive cancers in the Sister Study: A U.S.-wide prospective cohort. ![]()
Socioeconomic position (SEP) is a measure of the social and economic resources that help define how "well-off" someone is within society. It includes factors like income, educational attainment, and the ability to get enough food to eat. In a recent Sister Study project, researchers studied the relationship between childhood SEP and adult obesity. We reported that lower childhood SEP was associated with greater risk of being obese as an adult, even after accounting for adult SEP. Furthermore, experiencing improved SEP as an adult compared to childhood did not reduce the risk of being obese in adulthood. This suggests that childhood SEP may be an important risk factor for adult obesity, independent of adult resources.
Learn more here:
Early life socioeconomic position contributes to adult obesity independent of adult socioeconomic factors: Findings from the sister study cohort. ![]()
In animals, excess iron levels in blood have been shown to promote tumor growth, and iron deficiency has been associated with reduced or slowed tumor growth. In a study that included 2,494 women who were diagnosed with breast cancer since enrollment, Sister Study investigators recently reported that iron levels measured in blood collected when women joined the study (i.e., before they developed breast cancer) were not strongly associated with breast cancer tumor size. While iron levels may still affect tumor growth after onset, our results suggest that circulating levels of iron before breast cancer diagnosis are unrelated to tumor size at diagnosis.
Learn more here:
Associations Between Serum Iron Biomarkers and Breast Cancer Tumor Size. ![]()
Using dietary information reported on the enrollment questionnaire, all Sister Study participants were assigned scores that indicated how closely their eating patterns followed specific dietary recommendations, including the Mediterranean diet, Dietary Approaches to Stop Hypertension (DASH), the alternative Healthy Eating Index, and the Healthy Eating Index 2015. In a recently published study, we showed that, in general, having a healthy diet was associated with lower concentrations of specific biomarkers of oxidative stress in urine samples collected at the time of dietary assessment. As high oxidative stress may contribute to the progression of some types of cardiovascular disease, cancer, and metabolic disorders, this research illustrates a possible biological pathway underlying the relationship between healthy eating and reduced chronic disease risk.
Learn more here:
Association between healthy dietary patterns and markers of oxidative stress in the Sister Study. ![]()
February 4th is World Cancer Day. World Cancer Day is an international day marked on February 4 to raise awareness of cancer and to encourage its prevention, detection, and treatment.
Today and every day we are grateful for our Sister Study participants and their families for their selfless contributions to research.
You have shown your dedication for many years by consistently sharing valuable in-depth details about your health and your family's health, and by responding to so many of the various requests with which we approach you. Every year that you generously provide more information allows investigators to better understand factors related to cancer risk.
The Sister Study team thanks our participants and their families for 20 years of contributions to cancer research.
Sister Study researchers investigated whether the association between racial and ethnic discrimination and hypertension varied by levels of attained education. Approximately half of all participants had at least a college degree when they enrolled in the Sister Study. Black / African American women with at least a college degree reported the highest burden of race and ethnicity-based discrimination, with 83% of women with hypertension reporting experiencing everyday discrimination (e.g., unfair treatment at a business), compared to 64% of women with hypertension and a high school degree or less. Everyday discrimination was associated with higher hypertension risk among Black women with college or higher education, but not among Black women with some college but no degree. Educational attainment did not modify the association between everyday discrimination and hypertension among other racial and ethnic groups. Discrimination-related hypertension may disproportionately affect Black women with the highest levels of educational attainment.
Learn more here:
Racial and Ethnic Discrimination and Hypertension by Educational Attainment Among a Cohort of US Women. ![]()
Cannabis (marijuana) is widely used but its long terms effects on health are not fully understood. Information from the Sister Study and six other large cohorts was combined to examine how lifetime cannabis use was associated with certain changes to DNA. Overall, 9436 participants (7795 European and 1641 African ancestry) were included. After accounting for the effects of cigarette smoking, sites in or near 4 genes (ADGRF1, ADAM12, ACTN1, and LINC01132) were found to be strongly associated with lifetime cannabis use. These findings may serve as a starting point for further research on the mechanisms through which cannabis exposure impacts health outcomes.
Learn more here:
Trans-ancestry epigenome-wide association meta-analysis of DNA methylation with lifetime cannabis use. ![]()
Having green spaces in urban environments is known to have important health benefits. These benefits are thought to be achieved, in part, because of increased opportunities for recreational physical activity. Using national land cover data, each Sister Study participant was assigned a score that captured their proximity to green spaces. Compared to those with the lowest level of greenness, participants with the highest level of greenness were more likely to garden, participate in sports, run, walk, and engage in conditioning exercises. These findings suggest that greenness may promote physical activity and provide support for building and maintaining green environments as a way to improve human health and wellbeing.
Learn more here:
Neighborhood greenness and participation in specific types of recreational physical activities in the Sister Study. ![]()
Out of nearly 3,400 publications by NIEHS researchers and grantees in 2023, institute leaders selected 30 as Papers of the Year. Three of these were led by Sister Study investigators!
Why breast cancer incidence varies across the United States
Environmental exposures and neighborhood-level socioeconomic factors may contribute to geographic disparities in breast cancer incidence, according to NIEHS researchers and their collaborators. Together, the results provide additional evidence for a role of environmental exposures in breast cancer incidence and suggest that geographic-based risk factors may vary according to breast cancer subtype.
Read the full summary here:
Why breast cancer incidence varies across the United States. ![]()
Indoor wood-burning may be linked to lung cancer in U.S. women
Indoor wood-burning from stoves and fireplaces is associated with the development of lung cancer among women in the U.S., according to researchers from NIEHS, including the institute's Division of Translational Toxicology. These findings are some of the first prospective evidence in the U.S. demonstrating that even occasional exposure to indoor wood smoke is associated with a higher incidence of lung cancer, including among never smokers.
Read the full summary here:
Indoor wood-burning may be linked to lung cancer in U.S. women. ![]()
Exploring the link between early-life trauma and diabetes
The association between traumatic childhood experiences and type 2 diabetes varies by race and ethnicity, according to NIEHS researchers and their collaborators. According to the authors, the study suggests that Latina women may be an understudied population at a particularly high risk of type 2 diabetes associated with early-life trauma. In addition, tailored prevention and intervention efforts that protect youth from trauma and inhibit likely mediators such as metabolic abnormalities may help ease the burden of type 2 diabetes among women.
Read the full summary here:
Exploring the link between early-life trauma and diabetes. ![]()
See all NIEHS Papers of the Year here:
2023 Papers of the Year. ![]()
Sister Study researchers investigated sleep quality among cancer survivors compared to similarly aged women without cancer history. Sleep quality was assessed based on usual sleep duration, sleep medication usage, insomnia symptoms, long sleep-latency onset (≤30 min to fall asleep), frequent night awakenings (waking ≤3/night, ≤3 times/week), and frequent napping (≤3 times/week), as well as a composite outcome of ≤1 sleep disturbances. Results indicated that sleep disturbances were generally not more common among cancer survivors compared to those without cancer. However, cancer survivors diagnosed more than 2 years prior were more likely to report ≤1 sleep disturbance compared to survivors reporting 0-2 years from diagnosis. Addressing sleep disturbances in longer-term cancer survivors may improve their health and well-being.
Learn more here:
Sleep disturbances among cancer survivors. ![]()
Serum iron levels can be important contributors to health outcomes, but it is not often feasible to measure blood iron in all study participants. Researchers examined whether factors measured in the Sister Study questionnaires, such as diet, supplement use, recency of blood donation, and medical conditions, could be used to predict iron status. However, none of the examined factors were strongly predictive. Any future prediction models should consider unmeasured factors, including but not limited to: concurrent environmental exposures, temporal factors, and genetic variations in absorption and storage.
Learn more here:
Development and validation of a prediction model for iron status in a large U.S. cohort of women. ![]()
There is strong evidence that neighborhood greenery promotes better mental health, but greenery may not be evenly distributed within a neighborhood. Using data from the Sister Study, researchers examined whether the previously observed inverse correlations between residential tree cover and depressive symptoms varied across residential areas in accordance with measures of housing inequality. Overall, tree cover was higher in neighborhoods historically considered by realtors and lending agencies to have greater financial viability. Higher tree cover was associated with reduced risk of experiencing depressive symptoms, with the strongest associations observed in hazardous or "red-lined" neighborhoods. These findings support a remediation strategy to expand neighborhood greenery as a way to improve mental health and other public health priorities.
Learn more here:
Association of Redlining and Natural Environment with Depressive Symptoms in Women in the Sister Study. ![]()
As we have described previously, women's "biological age" can be estimated by measuring levels of blood DNA methylation (a specific chemical change) at certain genetic sites. A new Sister Study publication reported that ambient particulate matter <2.5 µm and <10 µm in diameter (PM2.5 and PM10) and nitrogen dioxide (NO2) were associated with higher biological age among Black women, but not non-Hispanic White women. This research highlights the importance of considering differences in associations and correlated environmental exposures by race, especially given that Black participants had higher median air pollution exposure than non-Hispanic White participants, and because few prior studies of biological age have included participants of color.
Learn more here:
Air pollution and epigenetic aging among Black and White women in the US. ![]()
Sister Study investigators examined how geography and neighborhood-level environmental and socioeconomic factors may contribute to breast cancer incidence. The lowest breast cancer rates were observed in the South and Southeast US, with a greater rates in the Northwest, Midwest, and Northeast. Of the measures considered, nitrogen dioxide (NO2; an indicator of traffic-related air pollution), light at night, and the area deprivation index (a measure of neighborhood level socioeconomic factors) were the most important residential-level predictors of breast cancer risk overall. These plus measures of the chemical composition of air pollution (specifically fine particulate matter, PM2.5) and greenspace were strong predictors of estrogen receptor positive breast cancer. These results support a role of environmental exposures in breast cancer incidence and suggest variability by breast cancer subtype.
Learn more here:
Understanding the role of environmental and socioeconomic factors in the geographic variation of breast cancer risk in the US-wide Sister Study. ![]()
Poor sense of smell, or poor olfaction, is common in older adults and may be linked to adverse health conditions. To better understand how environmental factors may contribute to poor olfaction, Sister Study researchers examined the association between air pollution measures and olfaction among a sample of participants who completed a Brief Smell Identification Test in 2018-2019. Overall, none of the examined air pollutants were strongly associated with poor olfaction.
Learn more here:
Ambient Air Pollutants and Olfaction among Women 50-79 Years of Age from the Sister Study. ![]()
Olfactory impairment (i.e., poor sense of smell) and Parkinson's disease may share common genetic and environmental risk factors. Among 3358 Sister Study participants who provided samples for genetic analysis and completed a Brief Smell Identification Test (administered in 2018-2019), researchers calculated genetic risk scores for Parkinson's disease based on genotypes from 90 different genetic variants. As expected, the risk score was strongly associated with the risk of having Parkinson's Disease. Additionally, women with the highest 25% of estimated genetic risk were also more likely to have olfactory impairment. These preliminary data suggest that Parkinson's Disease and poor olfaction share some genetic components.
Learn more here:
Polygenic risk score for Parkinson's disease and olfaction among middle-aged to older women. ![]()
Sister Study researchers were interested in how diet may be related to risk of type 2 diabetes, and what role socioeconomic factors may play in that association. Participants who completed the 110-item food frequency questionnaire during enrollment were given scores based on how closely their diets aligned to each of 4 healthy eating indices (alternate Mediterranean diet, Dietary Approaches to Stop Hypertension, alternative Healthy Eating Index, and Healthy Eating Index 2015). The four diets all involve eating lots of fruits and vegetables, whole grains, and nuts and legumes, and discourage intake of red meats and fats. Eating a healthy diet based on any of these indices was associated with lower rates of being diagnosed with type 2 diabetes after enrollment. These associations were stronger among women with higher educational attainment, higher income, and living in less deprived neighborhoods, suggesting that factors other than diet are more important among groups with lower socioeconomic status.
Learn more here:
Dietary patterns, socioeconomic disparities, and risk of type 2 diabetes in the Sister Study. ![]()
The Sister Study contributed data to a very large study examining the combined effects of genetic and non-genetic (i.e., "environmental") factors. The study included 72,285 breast cancer cases and 80,354 controls of European ancestry. More than 7 million genetic factors were considered in combination with 7 established demographic, lifestyle, and reproductive risk factors for breast cancer. Two independent pairs were identified: the combined effect of adult height and a genetic variant in the LINGO2 gene was associated with breast cancer overall, and the combined effects of age at first period and a genetic variant in the SPATA13 gene was associated with estrogen receptor positive breast cancer. Overall, however, gene-by-environment interactions made a very small contribution to understanding breast cancer risk. Of note, the study was limited in its exploration of environmental risk factors.
Learn more here:
A genome-wide gene-environment interaction study of breast cancer risk for women of European ancestry. ![]()
Because women using genital talc use or douche may be exposed to potentially harmful chemicals, Sister Study researchers investigated whether these practices may be associated with risk of uterine fibroids, a non-cancerous gynecologic condition. Prior to age 35, 29% of Black / African American and 9% of non-Hispanic White Sister Study participants had been diagnosed with uterine fibroids. Genital talc use during early adolescence (ages 10-13) was positively associated with having had a fibroid before age 35, but douching during early adolescence was not independently associated with fibroids. Combined use of genital talc and douche was positively associated with fibroids before age 35 among Black women. This research shows how chemical exposures from intimate care products used during early adolescence may influence fibroid development.
Learn more here:
Association of genital talc and douche use in early adolescence or adulthood with uterine fibroids diagnoses. ![]()
Sarah Feng embraced unknown, new opportunities as she transitioned from skating to environmental health.
Please enjoy this story about Sarah and her work on the Sister Study as a summer intern studying early life radiation exposure and incident breast cancer:
Scientific Journeys: From ice skating championships to NIEHS. ![]()
The Sister Study is proud to recognize our outstanding postdoctoral fellows, Che-Jung Chang, Jennifer Ish, Kemi Ogunsina, Jennifer Woo, Dazhe Chen, and Meklit Tesfaye. A postdoctoral fellow is a training-focused position bridging the student experience with the full-time professional role. Each fellow's unique research interests utilize the information you and other Sister Study participants have provided us over the course of the study to advance research not only for breast cancer, but women's health as a whole.
If you are interested in reading some of our Postdoctoral fellows' recent findings, you can see a full list of Sister Study publications here:
Sister Study Publications. ![]()
This ten-minute video commemorates the 20th anniversary of the NIEHS-led Sister Study to discover the environmental and genetic causes of breast cancer. The video showcases how the Sister Study got started, what it has accomplished, and shines a spotlight on the 50,000 study participants who make it all possible.
Watch the video here:
Sister Study 20th Anniversary Video. ![]()
October is Breast Cancer Awareness Month and we at the Sister Study would like to join our participants and friends of the study to remember those affected by breast cancer. With our ongoing research, we honor those we have lost and those who continue to fight against breast cancer. We are grateful to those of you who participate in research like the Sister Study so we can work together toward solutions. Thank you.
The NIEHS Sister Study will turn 20 this year. Watch this 30-second video trailer about the progress being made to discover the environmental and genetic causes of breast cancer. Stay tuned for the full ten-minute video coming out October 2.
Watch the trailer here:
20th Anniversary Video Trailer. ![]()
Epidemiological studies conducted mostly in low- and middle-income countries have observed a positive association between indoor wood burning and lung cancer, but usage patterns differ in the United States. 62% of Sister Study participants reported having an indoor wood-burning fireplace or stove in their longest-lived adult residence and 20% used those fireplaces or stoves at least 30 days per year. Lung cancer is far less common than breast cancer in U.S. women and in this cohort, with 347 medically confirmed cases. Compared to those without a wood-burning fireplace/stove, women who burned wood indoors 30 or more days/year had an elevated rate of lung cancer. Results were similar in analyses limited to women who never smoked. These results provide further confirmation that indoor woodburning may contribute lung cancer risk.
Polygenic risk scores (PRSs) can be used to predict breast cancer risk based on the combined effects of many genetic markers that each confer very small increases in breast cancer risk. Most large genetic studies of breast cancer have been performed in individuals of European ancestry, and it is unclear how well the existing PRSs work among women of different backgrounds, including among Ashkenazi Jewish women who have a higher chance of being positive for BRCA1 or BRCA2. Using a PRS developed in women of European ancestry—including women from the Sister Study, the research found that the PRS performed well in Ashkenazi Jewish women from Israel in terms of identifying Ashkenazi Jewish women with elevated risk of breast cancer.
Thyroid cancer incidence has increased worldwide. Increasing rates of obesity may play a role, and Sister Study researchers sought to further investigate how body mass index, other measures of body size, and certain metabolism-related conditions may be related to thyroid cancer. 259 Sister Study participants have been diagnosed with thyroid cancer since enrollment. Higher body mass index, higher waist circumference, and higher waist-to-hip ratio were positively associated with thyroid cancer occurrence, as were lipid disorders such as high cholesterol, borderline diabetes, hypertension (high blood pressure), and polycystic ovary syndrome. These findings provide insights into potential biological mechanisms linking obesity and thyroid cancer.
Learn more here:
Obesity, obesity-related metabolic conditions, and risk of thyroid cancer in women: results from a prospective cohort study (Sister Study). ![]()
Parkinson's disease (PD), a neurodegenerative disease that affects the nervous system, including movement and speech, is one of the many health conditions we ask about in our follow-up questionnaires. Rates of PD increase with age, and while it is more common in men, many older women are also affected. It is second most common age-related neurodegenerative disorder after Alzheimer's disease. Environmental exposures may contribute to PD risk, but population studies have been difficult because, until now, physicians and researchers believed that PD cases could only be identified if all potential study participants underwent a clinical examination. Recent work in the Sister Study demonstrates that with a few simple additional pieces of information about symptoms and/or use of PD medications, it is possible to make use of self-reported information to identify persons with PD who can participate in epidemiologic research studies. This will greatly enhance our ability to identify risk factors for this debilitating condition.
Learn more here:
Parkinson's Disease Case Ascertainment in the Sister Study: A Cohort for Environmental Health Research. ![]()
Loss of sense of smell increases with aging and is associated with some neurodegenerative diseases, including Parkinson's disease. Researchers were curious whether regular use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin, may be associated with poor olfaction (sense of smell). A few years ago, 3406 Sister Study participants completed the 12-item Brief Smell Identification Test. Poor olfaction was defined as a test score of ≤9 correctly identified smells. Overall, NSAID use was not associated with poor olfaction, but long-term regular use of aspirin or ibuprofen was associated with poor olfaction among women who never regularly used other types of NSAIDs. These preliminary findings warrant independent confirmation.
Prenatal exposure to diethylstilbestrol (DES) has been linked to several adverse health outcomes. Using data from the Sister Study and a National Cancer Institute DES Cohort Study, researchers explored if women exposed to DES while in utero had different DNA methylation patterns (i.e., different chemical markers attached to their DNA) than those not exposed to DES. They found that DES exposure was associated with changes in 6 genes: EGF, EMB, EGFR, WNT11, FOS, and TGFB1, all of which are related to changes in cell growth and specialization. These findings support the idea that methylation-related chemical changes in DNA could explain some adverse health outcomes associated with DES exposure.
Learn more here:
In utero exposure to diethylstilbestrol and blood DNA methylation in adult women: Results from a meta-analysis of two cohort studies. ![]()
Thank you to all the sisters who have already shared their reasons for joining Sister Study! We are so grateful for your ongoing support of the study and love hearing from you all!
The 20th Anniversary flyers are now available for printing on our Sister Study Website! Click the links below to access printable PDFs. We would love to see your reason for participating in the study! Please email us with your photos at update@sisterstudy.org or share with us on Facebook. By submitting a photo, you are consenting to your photo being shared by the Sister Study on the website, Facebook group and other communication modes.
If you'd like to participate and need a printed copy of the flyer, please send us a direct message on Facebook or email us at update@sisterstudy.org. We will mail you one.
We are so grateful for all of our participants! Thank you for your continued contributions to research!
Find the flyers here:
The Sister Study 20th Anniversary. ![]() The Sister Study is important to me because....
The Sister Study is important to me because.... ![]() I continue to participate in the Sister Study because....
I continue to participate in the Sister Study because.... ![]()
Certain genetic factors may contribute to the risk of several types of cancer. In a recent collaborative study that included nearly 1 million individuals with and without cancer, investigators identified 15 genetic mutations associated with all 12 types of cancer studied (breast, colorectal, endometrial, esophageal, glioma, head and neck, lung, melanoma, ovarian, pancreatic, prostate, and renal). Another 77 genetic sites were associated with at least 2 of the cancer types. Overall, these results suggest that some genetic risk variants are shared among cancers, though much of cancer heritability is cancer-specific.
Learn more here:
Genome-wide analyses characterize shared heritability among cancers and identify novel cancer susceptibility regions. ![]()
An estimated 21 million Americans live within a mile of a Superfund site. To learn more about how that proximity might affect health, Sister Study investigators looked at metal biomarker levels among women who lived near a Superfund site and published their findings in an Environmental Health Perspectives research letter. They reported that non-Hispanic Black women were likely to have higher levels of certain metals than their non-Hispanic White counterparts—even when they lived the same distance from a site.
Learn more here:
The Price of Proximity: Black Women Disproportionately Exposed to Superfund Metals. ![]()
August 7th is National Sisters Day: With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Sisters Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
For the summer of 2023, 5 graduate or undergraduate students are working with the Sister Study research team as part of the National Institutes of Health summer internship program. These interns complete an 8-12 week research project which culminates in a poster session sharing their preliminary findings. Many of the students go on to publish their work as research papers. Our young researchers picked a wide variety of topics to study, including: measures of outdoor greenspace and sleep health, historic air pollution exposure and breast cancer risk, noise pollution and breast cancer risk, hairdresser's occupational exposures and risk of hormone-related diseases, and early life radiation exposure and breast cancer risk. The undergraduate student studying early life radiation and breast cancer, Ms. Sarah Feng, took second place at the institute-wide communication challenge event!
The pregnancy complications preeclampsia and preterm birth may affect future breast cancer risk in different ways, even though women with preeclampsia are more likely to have a preterm birth. A very large study was needed to disentangle these relationships. In a recently published paper, Sister Study investigators led an analysis of data from 6 different cohort studies, including the Sister Study, to try to understand how preeclampsia and preterm birth may be linked to breast cancer occurring prior to menopause. They found that women who experienced preeclampsia were less likely to develop premenopausal breast cancer. While preterm birth was not associated with premenopausal breast cancer among all women, it was associated with higher rates of premenopausal breast cancer among those who experienced preeclampsia or gestational hypertension (high blood pressure during pregnancy). This study helps to clarify the complicated relationships between certain pregnancy complications and premenopausal breast cancer risk and may help to identify high risk women.
Learn more here:
Hypertensive conditions of pregnancy, preterm birth, and premenopausal breast cancer risk: a premenopausal breast cancer collaborative group analysis. ![]()
Click to watch a new interview with Dr. Alexandra White, Sister Study Investigator, about her team's recent publication regarding chemical hair straighteners!
Chemical Hair Straighteners Study. ![]()

Meet Dr. Sarah Cohen, the Sister Study's new Project Director! In this role, she will oversee all aspects of the study's data, laboratory, and manuscripts using our rich data resource. She will provide scientific oversight to the study team, and will work closely with the study investigators at NIEHS to continue to build on the amazing legacy of this important study.
Sarah recently joined the team spending the last decade leading a consulting practice in the private sector. She has designed and directed research studies in the US and around the world that covered a variety of topics including cardiovascular disease, diabetes, cancer screening, infant feeding, critical care nutrition, physical activity, and potential health effects of environmental exposures. Sarah has also spent over twenty years as an investigator on the Million Person Study which is the first and largest study of its kind to investigate the health effects of low-dose radiation on American workers and veterans throughout the 20th century. She started her career as an investigator on the Southern Community Cohort Study which is a large study in the American South designed to better understand the root causes of cancer health disparities.
Sarah attended the University of North Carolina at Chapel Hill for her undergraduate and doctoral degrees, and in between, spent two years at the University of Michigan earning a master's degree and learning that she isn't cut out for cold weather. Sarah currently lives in Durham, North Carolina, with her family including her husband Josh (who works at Duke's Fuqua School of Business but remains a Tarheel fan like the rest of the family!), her daughter and two sons, and two cats. Sarah loves to cook, visit Farmer's Markets, and read cookbooks. She is also an avid runner with a group of local women. Renovating houses is also one of her passions—ask her about her love for wallpaper! She also loves to read fiction and hear your book suggestions, and she adores seeing Broadway musicals both on tour in Durham and in New York whenever she gets the chance.
Welcome to the team, Sarah!
You may hear about this press release announced July 19th, made possible by our amazing Sister Study participants. Thank you, and thanks to the many researchers committed to learning more about breast cancer.
Women Treated for Breast Cancer May Age Faster Than Cancer-free Women NIH study finds radiation shows strongest association, less for surgery and endocrine treatments
NEWS: Women diagnosed and treated for breast cancer have increased biological aging compared to women who remain free of breast cancer, according to a new study by NIEHS researchers and their collaborators.
Biological age differs from chronological age in that it considers not only the time elapsed, but also numerous biological and physiological factors like genetics, lifestyle, nutrition, and comorbidities.
Among women diagnosed with breast cancer, the association with faster biological aging was most pronounced for those who received radiation therapy, while surgery showed no association with biological aging.
This finding suggests that developing cancer is not what increases the aging effect.
Learn more here:
Women Treated for Breast Cancer May Age Faster Than Cancer-free Women
. ![]()
With our 20 year anniversary celebration just around the corner, we wanted to give our amazing participants the opportunity to share their reasons for joining and continuing to participate in this vital study! We have multiple flyers that we encourage you to print out and fill in with your own personal reasons for being a part of Sister Study.
We would love you see your reasons why! Please feel free to snap a photo of you and your flyer and send it to us via email at update@sisterstudy.org. By submitting a photo, you are consenting to your photo being shared by the Sister Study on the website, Facebook group and other communication modes.
If you'd like to participate and need a printed copy of the flyer, please send us a direct message on Facebook or email us at update@sisterstudy.org. We will mail you one.
We are so grateful for all of our participants! Thank you for your continued contributions to research!
Find the flyers here:
The Sister Study 20th Anniversary. ![]() The Sister Study is important to me because....
The Sister Study is important to me because.... ![]() I continue to participate in the Sister Study because....
I continue to participate in the Sister Study because.... ![]()
High blood pressure, or hypertension, is common in older individuals and is a major risk factor for cardiovascular disease. In a new Sister Study investigation, researchers examined whether biological age, which was measured using certain genetic markers found in blood, was associated with hypertension. They found that 3 different measures of "methylation-based biological age" were positively associated with a history of hypertension. Further, among women without hypertension at enrollment, those with higher biological age were more likely to receive a new diagnosis of hypertension during follow-up. These findings provide further evidence that biological age markers may be useful tools for predicting the occurrence of chronic diseases and understanding how chronic diseases affect the body.
Learn more here:
Methylation-Based Biological Age and Hypertension Prevalence and Incidence. ![]()
Some of you may be familiar with Dr. Susan Love and her lifelong work on behalf of women with breast cancer. We therefore wanted to share the sad new that she passed away on Sunday 7/2/2023. Dr. Susan Love was a renowned breast surgeon and women's advocate who leaves a profound legacy through the Dr. Susan Love Foundation for Breast Cancer Research. In 2007, when we were still recruiting participants for the Sister Study, we approached Dr. Love about collaborating and accessing her newly established Army of Women database of women interested in being contacted for research opportunities. She instantly agreed by giving us access to her excellent staff to facilitate contacting women who had joined her "Army". Dr. Love also collaborated on a press release making public her endorsement and recruitment support of the Sister Study. Many women joined the Sister Study as a result of these efforts. We are grateful for her contribution to the Sister Study, and grateful for her courage, selflessness and foresight in supporting women's health and fighting against breast cancer
Learn more here:
The Dr. Susan Love Foundation for Breast Cancer Research. ![]()
A recent Sister Study paper investigated the relationship between exposure to light at night and various measures of sleep quality. Light at night exposure was based on participants' responses to questions about lights on while they slept, including a TV, a light in the room, a light outside their room, or a nightlight. Compared to sleeping with no light in the bedroom, sleeping with a TV on was correlated with several measures of poor sleep health, including shorter sleep duration, inconsistent sleep time, and overall poor sleep scores.
Learn more here:
Exposure to indoor light at night in relation to multiple dimensions of sleep health: Findings from the Sister Study. ![]()
Thank you if you have already completed your 2022-2023 Annual Health Update! In October 2022 we began contacting all Sisters about completing your Annual Health Update. We have now received a response from 81.6% of our participants!
This Facebook post is to remind you to please check your emails or postal mail and complete your Annual Health Update as soon as you can.
We are deeply grateful for your continued participation! If you have not received your AHU or have any questions or issues, please contact our Help Desk toll-free at 877-4SISTER (877-474-7837) or email us at update@sisterstudy.org. We will gladly help you!
REMINDER
Enter our $500 Drawing upon Completing your Health Update:
- To show our appreciation, when you complete your health update, you will be entered into a $500 gift card drawing. The earlier you complete your survey, the better your odds, as you will then be entered in each monthly drawing that follows in the 2022-2023 health update collection period.
- Approximate odds of winning are 1 in 5,000 to 1 in 48,000 depending on when you complete your health update.
- If you win but do not want the gift card, please feel free to decline.
Thank you in advance for continuing to complete these valuable questionnaires!
If you have not yet and would like to complete this year's questionnaire online, please click the link below:
The Sister Study Annual Health Update. ![]()
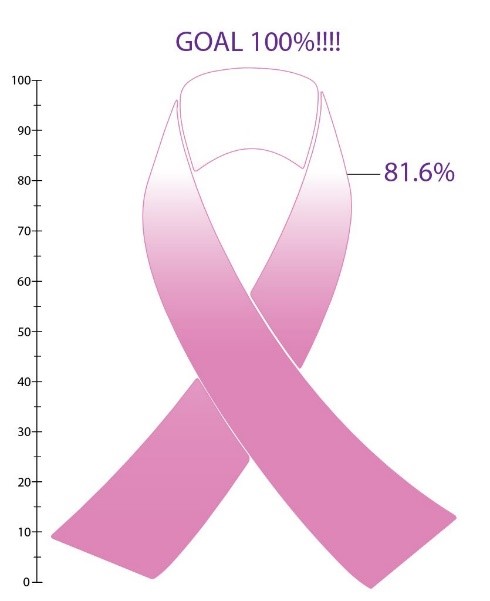
More than 73 million people in the United States live within 3 miles of a Superfund site, which can be sources of exposure to chemicals in hazardous waste. Since these sites tend to be in areas of lower socioeconomic status or with higher proportions of people of color, they can contribute to exposure or health disparities. Sister Study investigators recently found that among non-Hispanic Black women, residential proximity to one or more Superfund sites was associated with higher toenail concentrations of antimony, lead, and cadmium. Antimony and lead were also positively associated with Superfund site proximity among non-Hispanic White women. These findings demonstrate that living near Superfund sites may increase internal levels of chemicals with known or potential adverse health effects.
Learn more here:
Residential Proximity to Metal-Containing Superfund Sites and Their Potential as a Source of Disparities in Metal Exposure among U.S. Women. ![]()
Sister Study investigators and researchers from Duke University examined the association between poor sleep patterns and risk of developing hypertension (high blood pressure). They found that women with insomnia (difficulty falling or staying asleep) or insomnia plus short sleep (<7 hours per night) were more likely to develop hypertension. These associations were stronger among younger and premenopausal women but did not differ by race/ethnicity. This research demonstrates how poor sleep may impact other aspects of health.
Learn more here:
A prospective study of multiple sleep dimensions and hypertension risk among white, black and Hispanic/Latina women: findings from the Sister Study. ![]()
The main reason is that some things may change—you might lose or gain weight, start a new hobby, be prescribed a new medication, or develop a new medical condition, and we want to do our best to capture that information! Other times we realize that we did not originally ask the question in the best way and want you to provide additional or clarifying information. For example, we asked about your personal care product use (hair dyes, make-up, talc products, etc.) at enrollment, but focused specifically on use in your early adolescence and in the year before you joined. In later questionnaires, we asked about your recent use (after you joined) and also tried to capture information about your lifetime use by asking about what products you used during each decade of your life.
If you have not yet and would like to complete this year's questionnaire online, please click the link below:
The Sister Study Annual Health Update. ![]()
Many of our participants tell us they joined Sister Study as a way to honor and support their sisters. Since enrollment, the majority of our questionnaires have focused on you, rather than your sister; Why?
Sister Study investigators are most interested in learning about you and your life! One of the hardest parts about studying a disease like breast cancer is that if we want to learn how to prevent it, we have to get more information about women's lives before they develop cancer. That also means we have to enroll a lot of women because we don't know who will go on to develop breast cancer and who will not.
When you first joined the study, we asked many questions about your sister with breast cancer. This included questions about when she diagnosed, what type of breast cancer she had, and what kind of treatment she received. Additionally, some of the sister pairs (including at least one sister with breast cancer and one without) participated in the Two Sister Study, a companion study focused on young-onset breast cancer. We continue to check in with all of the Two Sister Study ![]() participants.
participants.
Scientists who want to study what happens to women after they are diagnosed with breast cancer often recruit participants from a hospital or clinic—it is much easier to find and track patients this way! That being said, we are certainly interested in learning more about breast cancer survivorship. However, rather than trying to track down the original affected sister, we use the data we are already collecting from our own Sister Study participants, many of whom have unfortunately developed breast cancer themselves.
Learn more here:
Evidence for familial clustering in breast cancer age of onset
. ![]()
Health-Related Quality of Life Outcomes Among Breast Cancer Survivors. ![]()
Age- and treatment-related associations with health behavior change among breast cancer survivors
. ![]()
This week is National Women's Health week. The Sister Study would like to recognize our amazing team members and participants this week! We are committed to supporting the health and well-being of women every day!
This week can serve as a reminder to take steps to make your health and the health of women in your family and community a priority.
Please click the link below to find out more about healthy habits and important women's health screening information:
National Women's Health Week. ![]()
Polychlorinated dibenzo-p-dioxins and dibenzofurans ("dioxins") are persistent organic pollutants frequently produced during the combustion of chlorinated organic compounds. Some are known to be carcinogenic. Though dioxin levels have declined following their regulation in the 1990s, few studies have evaluated whether dioxin may be associated with breast cancer risk. We used publicly available data on industrial emissions at facilities located near Sister Study participant's homes to estimate participants' dioxin exposure levels. We then evaluated associations between estimated dioxin exposure and breast cancer risk. We found that long-term exposure to airborne dioxin emissions within 3 km of participants' residences was associated with increased breast cancer risk. This association was strongest for emissions from municipal solid waste facilities. These findings indicate that living in proximity to industrial emissions facilities may be linked to higher breast cancer rates.
Learn more here:
Residential proximity to dioxin emissions and risk of breast cancer in the sister study cohort. ![]()
In a recent Sister Study publication, we examined whether gynecological surgery was related to women's risk of developing breast cancer. Since many women who undergo a hysterectomy (removal of the uterus) or bilateral oophorectomy (removal of both ovaries) often take hormone therapy, we also considered the combined effects of surgery and hormone therapy. We found that having had a bilateral oophorectomy was associated with a lower incidence of breast cancer, both overall and when accompanied by unopposed estrogen hormone therapy. In contrast, hysterectomy without bilateral oophorectomy was associated with higher incidence of breast cancer, particularly for women who also took estrogen plus progestin hormone therapy. This work was led by a summer intern, Sharonda Lovett, who is currently completing her PhD in Epidemiology.
Learn more here:
Hysterectomy, bilateral oophorectomy, and breast cancer risk in a racially diverse prospective cohort study. ![]()
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Siblings Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
Today is the World Health Organization's 75th annual World Health day! Each year a theme is selected that highlights a priority area of public health. This year's theme is Health for All. World Health Day provides an opportunity for individuals in every community to get involved in activities that can lead to better health.
Sister Study participants and their families have been contributing to public health research for nearly 20 years! Every year that you generously provide more information allows investigators to better understand many chronic diseases. Every new finding allows our researchers to support improvement of health for all.
The Sister Study team thanks our participants and their families for nearly 20 years of contributions to research!
Learn more here:
75 years of improving public health. ![]()

Introducing our Sister Study Supervisor team! Maria, Brenda, Cari, Reneicha, Angelica, Yolanda, and Nicole are responsible for the management of participant outreach and retention. The supervisor team is dedicated to ensuring your contributions and responses to the Sister Study are documented and managed correctly each year. Their focus is always on providing the best experience possible for our participants.
Please help us recognize the hard work of the Sister Study our supervisors!
Polychlorinated dibenzo-p-dioxins and dibenzofurans ("dioxins") are persistent organic pollutants frequently produced during the combustion of chlorinated organic compounds. Some are known to be carcinogenic. Though dioxin levels have declined following their regulation in the 1990s, few studies have evaluated whether dioxin may be associated with breast cancer risk. We used publicly available data on industrial emissions at facilities located near Sister Study participant's homes to estimate participants' dioxin exposure levels. We then evaluated associations between estimated dioxin exposure and breast cancer risk. We found that long-term exposure to airborne dioxin emissions within 3 km of participants' residences was associated with increased breast cancer risk. This association was strongest for emissions from municipal solid waste facilities. These findings indicate that living in proximity to industrial emissions facilities may be linked to higher breast cancer rates.
Learn more here:
Residential proximity to dioxin emissions and risk of breast cancer in the sister study cohort. ![]()
The Sister Study has been publishing a lot on how personal care products such as hair straighteners/relaxers and talcum powder may have adverse health effects. However, we were not sure how consistently women could report on what products they used. In a study that focused on douching and application of talc to the genital area, we compared how Sister Study participants responded to questions about use on the enrollment survey (2003-2009) relative to how they responded to similar questions included on the fourth follow-up questionnaire (2017-2019). We found that most women were able to provide consistent responses, with 90% providing the same response about ever douching at both time points, and 87% providing the same answer about ever using talc in the genital area. We hope that this information, along with the new data we collected about use during each decade of life, will help us better understand how use of these products may impact health.
Learn more here:
Douching and genital talc use: Patterns of use and reliability of self-reported exposure. ![]()
Contralateral breast cancer is a second breast cancer diagnosis in the opposite breast from the original tumor. In an investigation that included Sister Study participants, researchers sought to estimate the risk of contralateral breast cancer among women known to be carriers of higher risk pathogenic variants in established breast cancer-related genes (ATM, BRCA1, BRCA2, CHEK2, or PALB2). They found that women diagnosed with breast cancer and known to carry mutations in BRCA1, BRCA2, CHEK2, but not ATM were at substantially increased risk of contralateral breast cancer and may benefit from enhanced surveillance and risk reduction strategies. To help put this in context, the estimated 10-year risk of developing contralateral breast cancer among premenopausal women was estimated to be 33% for those with BRCA1 mutations, 27% for those with BRCA2 mutations, and 13% for those with CHEK2 mutations. The 10-year risk of developing contralateral breast cancer among postmenopausal mutation carriers was 12% for BRCA1, 9% for BRCA2, and 4% for CHEK2.
Learn more here:
Contralateral Breast Cancer Risk Among Carriers of Germline Pathogenic Variants in ATM, BRCA1, BRCA2, CHEK2, and PALB2. ![]()
The Sister Study would like to know important changes in your health or contact information!
- Have you moved or changed your telephone number or e-mail address?
- Have you been diagnosed with cancer or another major illness?
- Have you had any major injuries or surgeries?
- Would you like to share any other information with the study?
Please use this link ![]() to send your updates to the Sister Study. You can also call us toll-free at 877-4SISTER (877-474-7837) or email us at update@sisterstudy.org.
to send your updates to the Sister Study. You can also call us toll-free at 877-4SISTER (877-474-7837) or email us at update@sisterstudy.org.
- Please be mindful that we cannot protect your personal information via email format.
If you receive a call back from our Sister Study team members, your caller ID will display "877-474-7837." This is the toll-free number for the Sister Study.
If you have been diagnosed with breast cancer or any other type of cancer, please visit our I Was Diagnosed With... ![]() page to learn more.
page to learn more.

Please help us recognize Irina Khodush, our Sister Study Data Processing Manager! Irina has been a part of Sister Study since its inception in 2003! She is a key member of our team and we are so grateful for her commitment to the study. Irina is responsible for data receipt, organization, and verification. She is dedicated to ensuring your continued contributions to the Sister Study are documented accurately and the resulting data used by our investigators are cleaned and organized effectively.
Please help us recognize Irina's hard work and expertise!

Genetic data from the Sister Study was pooled with data from many other studies to examine how the combined effects of multiple mutations within the same gene might contribute to breast cancer risk. The investigators found that among women of European descent, 14 genes were significantly associated with breast cancer risk. Two of these, FMNL3 and AC058822.1, had never before been linked to breast cancer. In an analysis that additionally included individuals of Asian, African, and Latin American and Hispanic ancestry, investigators observed a very strong association between breast cancer and ESR1, the gene that encodes estrogen receptors. While the information about these genes is not yet clinically useful, the findings highlight the importance of studying genetic risk factors in diverse populations and considering the combined impact of multiple mutations within the same gene.
Learn more here:
Aggregation tests identify new gene associations with breast cancer in populations with diverse ancestry. ![]()
To show our appreciation for our dedicated Sister Study participants, we enter all participants who complete their health update survey each year into a $500 gift card drawing! The earlier you complete your survey, the better your odds, as you will then be entered in each monthly drawing that follows in the 2022-2023 health update collection period.
- Please note: approximate odds of winning are 1 in 5,000 to 1 in 48,000 depending on when you complete your health update.
If you have not yet and would like to complete this year's questionnaire online, please click the link below:
The Sister Study Annual Health Update. ![]()
While many studies have separately examined genetic and environmental (including behavioral) risk factors for breast cancer, relatively few have considered how these factors interact. For example, it is not known whether individuals with specific genetic variants might be more susceptible to the carcinogenic effects of alcohol or hormone therapy use. The Sister Study contributed data to a large study (46,060 cases and 47,929 non-cases total) of women with European ancestry that examined interactions between genetic profiles and established breast cancer risk factors. No strong interactions were identified, with the possible exception of variants in the C13orf45 gene and age at first full-term pregnancy. The overall study results suggest that gene-by-environment interactions play a limited role in determining breast cancer risk, though the study was not designed to detect small interaction effects or to consider specific subgroups.
Learn more here:
A genome-wide gene-based gene-environment interaction study of breast cancer in more than 90,000 women. ![]()
According to the NIH, in 2022, roughly 1.9 million people were diagnosed with cancer in the United States. Nearly half of those diagnoses are breast, prostate, lung, pancreas, or colon cancers. And yet, more than 40 percent of all cancer diagnoses can be linked to a preventable cause.
An estimated 287,850 women and 2,710 men will be diagnosed with breast cancer, which makes it the most common cancer diagnosis.
As February, National Cancer Prevention Month, comes to an end, we want to share our appreciation for our Sister Study participants.
National Cancer Prevention Month focuses on the things we can control to lessen our odds of developing cancer. Five of the top recommendations for lessening our risk include:
- Regular exercise
- Maintaining a healthy weight
- Eating healthy foods
- Quitting or never starting smoking
- Limiting alcohol use
To learn more about cancer prevention and statistics in the United States, please reference these AACR and NCI articles.
AACR National Cancer Prevention Month. ![]()
NCI Cancer Stat Facts. ![]()
Known genetic risk variants for epithelial ovarian cancer only account for 40% of inherited risk In a large, pooled analysis that included data from the Sister Study, investigators examined whether the number of copies of specific genetic markers carried by an individual (referred to as "copy number variants" or "CNVs") is related to her risk of developing ovarian cancer. CNVs at established breast and ovarian cancer-related genes, including BRCA1, RAD51C and BRCA2 were associated with ovarian cancer risk, as were 4 rare CNVs in novel locations. These results indicate that CNVs in these regions may contribute additional risk beyond what we already knew about these genes and identify possible targets for clinical genetic testing.
Learn more here:
Copy Number Variants Are Ovarian Cancer Risk Alleles at Known and Novel Risk Loci. ![]()

Introducing our Sister Study Advocate team! Ani, Genesis, Lakisha, Cari, Pam, and Storme are responsible for participant outreach and retention. Many of you may know or have worked with a member of our advocate team previously. They are dedicated to ensuring your continued contributions to the Sister Study are documented and managed correctly as well as providing the best experience possible for our participants.
Please help us recognize the hard work of the Sister Study Advocate team!
The advocate team is currently helping manage the newly launched 2022 Annual Health Update. Don't forget to complete your Annual Health update!
Today is World Cancer Day. World Cancer Day is an international day marked on February 4 to raise awareness of cancer and to encourage its prevention, detection, and treatment.Today and every day we are grateful for our Sister Study participants and their families for their selfless contributions to research.
You have shown your dedication for many years by consistently sharing valuable in-depth details about your health and your family's health, and by responding to so many of the various requests with which we approach you. Every year that you generously provide more information allows investigators to better understand factors related to cancer risk.
The Sister study team thanks our participants and their families for nearly 20 years of contributions to cancer research.
Since we began analyzing the data provided by our generous Sister Study sisters, our researchers have published over 250 scientific papers! These findings contribute to improvements in our understanding of the environmental and genetic causes of breast cancer and other important issues in women's health. We are proud of what we have accomplished together with our study sisters!
Thank you for sticking with us!
To view our study findings:
Sister Study Research Articles. ![]()
Out of nearly 3,300 publications by NIEHS researchers and grantees in 2022, institute leaders selected 32 as Papers of the Year. Two of these were led by Sister Study investigators!
Dr. Mary Diaz-Santana and her team investigated gestational diabetes and risk of type 2 diabetes in their paper titled Persistence of Risk for Type 2 Diabetes After Gestational Diabetes Mellitus ![]() The results of their analyses suggested that developing diabetes during pregnancy, especially multiple pregnancies, increases the risk of subsequent type 2 diabetes for decades.
The results of their analyses suggested that developing diabetes during pregnancy, especially multiple pregnancies, increases the risk of subsequent type 2 diabetes for decades.
Dr. Che-Jung Chang and her team studied the potential link between hair straighteners and relaxers and risk of developing uterine cancer in their paper titled Use of Straighteners and Other Hair Products and Incident Uterine Cancer ![]() Dr. Chang and her team found a positive association between the use of hair straightening and relaxing products and uterine cancer incidence. According to the authors, this study provides the first epidemiologic evidence of a relationship between the use of straightening and relaxing products and uterine cancer.
Dr. Chang and her team found a positive association between the use of hair straightening and relaxing products and uterine cancer incidence. According to the authors, this study provides the first epidemiologic evidence of a relationship between the use of straightening and relaxing products and uterine cancer.
Special thanks to all of our Sister Study participants, without whom these findings would not be possible. We are always grateful for your continued participation and generosity in sharing your health updates year to year!
Please help us recognize these Sister Study investigators and their teams for their outstanding research in 2022!
If you'd like to read more about the other papers selected for the NIEHS Papers of the year, please click the link below.
2022 Papers of the Year. ![]()
Childhood adversity has been associated with metabolic syndrome and type 2 diabetes risk in adulthood. A Sister Study investigation considered the role of race and ethnicity in these relationships and whether the link with type 2 diabetes was due to metabolic syndrome. Metabolic syndrome refers to having a combination of conditions including obesity—especially abdominal obesity—high cholesterol or triglyceride levels, high blood pressure and high blood sugar. More than 3,000 women reported new type 2 diabetes diagnoses since enrollment, including 2,479 non-Hispanic White women, 461 Black / African American women, and 281 Latina women. About half of study participants reported a traumatic childhood event such as being in an accident, or experiencing a major storm, family illnesses or deaths, or sexual or physical abuse. Having a traumatic childhood event was associated with a 13% higher risk of type 2 diabetes, with the strongest associations seen among Latina women (64% increase). This relationship was partially explained by increased prevalence of metabolic syndrome among those with traumatic childhood events.
Learn more here:
Ethnic Differences in Associations Between Traumatic Childhood Experiences and Both Metabolic Syndrome Prevalence and Type 2 Diabetes Risk Among a Cohort of U.S. Women

Introducing our Epidemiology team! Aimee D'Aloisio, Adeline Ho, Katiana Bougouma, Silvia Chapa, and Laura Darwin are responsible the aggregation and dissemination of Sister Study data. They work with our investigators to provide data and support analyses for new publications.
Katiana, Adeline, and Silvia recently joined the epidemiology team in November and are already assisting in the creation and review of new datasets. Please welcome them to the Sister Study team!
Thank you to our participants for their continued support of the Sister Study and thank you to the Epidemiology team for their critical role in furthering this essential research.

Introducing our Healthcare Providers Team! Bre Macon and Mercedes Anderson work with Sister Study participants and their healthcare providers to obtain medical records and other vital diagnosis information.
When you authorize the Sister Study to receive medical records about your cancer or other diagnoses, we are able to collect much more detailed information that improves our data and our investigator's analyses. This improved data increases our ability to identify connections between exposures and many chronic diseases.
Thank you to our participants for their continued support of the Sister Study and thank you to Bre and Mercedes for their diligence in furthering this essential research.
Researchers from the Sister Study have developed a new risk prediction score that may improve how we identify women at higher risk for developing breast cancer. The new risk score is based on measures of naturally occurring chemical modifications to DNA, known as DNA methylation, that can be assessed in the cells collected from a simple blood sample. In the Sister Study analysis, the investigators used blood samples that were provided at study enrollment and found that the new DNA methylation-based risk score helped predict whether or not a woman developed breast cancer during follow-up, especially when it was combined with existing information on other genetic or lifestyle factors. Though these results are novel and promising, further investigation and replication is needed to see if this will be useful in a clinical setting.
Learn more here:
Blood DNA methylation profiles improve breast cancer prediction. ![]()
Outdoor air pollution is thought to be associated with many cardiovascular diseases, including hypertension. We conducted a cross-sectional analysis to explore the association between hypertension and predicted exposure to specific components of air pollution that are caused by combustion of fossil fuels or other energy sources. Estimates of combustion-related air pollution exposure at Sister Study participant's home residences were extracted from the from the 2005 National Air Toxics Assessment database. Women were considered to have hypertension if they had a high systolic (≥140 mm Hg) or diastolic (≥90 mm Hg) blood pressure or were taking antihypertensive medication. High exposure to diesel emissions, 1,3-butadiene, acetaldehyde, benzene, formaldehyde and NO2 were associated with higher prevalence of hypertension, as was higher exposure to all the measured pollutants together. Stronger associations were observed among women reporting races/ethnicities (Hispanic/Latina, non-Hispanic Black and other) other than non-Hispanic White.
Learn more here:
Fossil-fuel and combustion-related air pollution and hypertension in the Sister Study. ![]()
Hypertension is an important public health issue because it is a risk factor for cardiovascular disease and affects most people over the age of 60. Characteristics of a person's immune system may be associated with their risk of developing hypertension. Using data from the Sister Study, we estimated the proportion of each type of white blood cell each participant had circulating in her body, finding that minor differences in those proportions were associated with later development of hypertension. Additionally, we found that having a history of hypertension was associated with a larger proportion of neutrophils, which are a type of white blood cells that cause inflammation. This study helps to clarify the immunological changes associated with hypertension and may be useful in the future for helping preventing the condition.
Learn more here:
Peripheral Immune Cell Composition is Altered in Women Before and After a Hypertension Diagnosis. ![]()

Kalimah Fleming (not pictured), Erica Parker, Eva Bauer, and Sarah Watson are responsible for study management, day to day development and tracking of participant outreach, and other vital efforts that keep the Sister Study running smoothly. They are currently tracking and managing the newly launched 2022 Annual Health Update. Please help us recognize the hard work of the Sister Study Operations and Retention team!
In late August, NIEHS held an event to highlight current breast cancer research and efforts to evaluate how combined exposures can influence the disease. Sister Study Investigator Dr. Lexie White, head of the NIEHS Environment and Cancer Epidemiology Group, co-chaired the event.
During the workshop Dr. White shared some of her Sister Study research on air pollution and breast cancer and Sister Study PI, Dr. Dale Sandler gave an overview of the Sister Study and how studies like ours can answer questions about the effects of environmental exposures. Two of our Sister Study post-doctoral fellows also shared some of their ongoing research focused on how mixtures of industrial emissions and personal care products may be related to breast cancer risk.
The workshop focused on understanding exposure mixtures and their impact on breast cancer risk. "We know that single exposure analysis does not accurately reflect real-life exposure patterns because people are exposed to multiple chemicals simultaneously," said Dr. White. "Analyzing one chemical exposure at a time can result in an underestimation of risk.
Learn more here:
Role of complex exposures in breast cancer highlighted during workshop. ![]()
In a paper published this morning in the Journal of the National Cancer Institute, Sister Study investigators Drs. Lexie White and Che-Jung Chang and their team found that women who used chemical hair straightening products were at higher risk for uterine cancer compared to women who did not report using these products.
"To our knowledge this is the first epidemiologic study that examined the relationship between straightener use and uterine cancer," said Dr. White. "More research is needed to confirm these findings in different populations, to determine if hair products contribute to health disparities in uterine cancer, and to identify the specific chemicals that may be increasing the risk of cancers in women."
The publication has been making headlines across media outlets for its important findings suggesting increased risk of uterine cancer.
Learn more here:
News Release: Hair straightening chemicals associated with higher uterine cancer risk. ![]()
The New York Times: Hair Straighteners May Pose a Small Risk for Uterine Cancer, Study Finds. ![]()
People: Hair-Straightening Chemicals Linked to Uterine Cancer in a New Study that Warns Black Women. ![]()
The Washington Post: Chemical hair-straightening linked to uterine cancer, study warns Black women. ![]()

Introducing a few members of our Sister Study Fulfillment Team! Last year, our fulfillment team sent out nearly 90,000 pieces of mail! Ken, Sha-Mel, Mrs. Sharron, and the rest of the fulfillment team have outstanding attention to detail and efficiency with their work. They are currently gearing up for the 2022/2023 Annual Health Update. Please help us recognize the hard work of the Sister Study Fulfillment Team!
The age that menopause occurs is determined by the number of remaining ovarian follicles, often referred to as the ovarian reserve. Ovarian follicles are formed in very early life; the number of follicles is greatest at birth and decreases with age and menstruation, but environmental factors could also lead to decreased ovarian reserve. In a Sister Study investigation, we examined possible associations between prenatal and childhood exposure to the farm environment and Anti-Müllerian hormone (AMH), a blood-based biological marker of ovarian reserve, in women ages 35-54 years. We found that women whose mothers worked or resided on a farm while they were pregnant had lower AMH levels. The data also suggested that childhood contact with pesticide-treated livestock or buildings was also associated with lower AMH. These findings raise concern that aspects of prenatal farm exposure may result in reduced adult ovarian reserve.
Learn more here:
Early-life Farm Exposure and Ovarian Reserve in a US Cohort of Women. ![]()
Nighttime light, either from inside your bedroom or outside your residence and shining in, is thought to increase the risk of breast cancer by disrupting the body's natural 24-hour (or circadian) rhythms, which serve a wide variety of biologic functions. To evaluate this in the Sister Study, we used questionnaire information on sources of indoor light exposure and estimated levels of outdoor light at night using satellite data. We then estimated how these light exposures were related to the risk of breast cancer. Sleeping with a television on or at least one light on in the bedroom was associated with a very small (9%) increase in breast cancer risk, although it is possible that this finding is due to chance. Living in an area with more outdoor light at night (e.g., from streetlamps or buildings) was not associated with an increased risk of breast cancer once we accounted for other co-occurring environmental exposures, such as air pollution and noise. So, while getting black-out curtains for your bedroom will likely help you sleep better, it is unlikely to reduce your risk of breast cancer.
Learn more here:
Light at night and the risk of breast cancer: Findings from the Sister study. ![]()

Meet our Sister Study Graphics Specialist, Noelle Rousseau! Noelle joined the Sister Study team in March of 2022, and is originally from Raleigh, NC. She works diligently to design the Sister Study flyers, newsletters, and website. Noelle is working hard to update the Sister Study website with our latest findings and publications. Please help us welcome Noelle!
Learn more here:
Check out the Sister Study website!. ![]()
Telomeres are long sections of DNA at the end of chromosomes that protect our genes. Telomeres tend to get shorter over time, making telomere length an attractive marker of cellular aging. The rate of shortening may be faster in early life, making Sister Study researchers wonder if certain exposures early in life play a role in telomere shortening. Following up on earlier reports, the researchers looked at the association between telomere length, which was measured in blood samples collected from a sample of Sister Study participants at enrollment, and data on 20 different types of traumatic experiences (such as physical or sexual abuse, major accidents or illnesses, or losses from natural disasters). They found that that experience of high early life trauma was associated with shorter telomere length in adulthood. These associations were not explained by trauma that was reported in adulthood, which reinforces the important role of early life experiences in shaping lifetime health.
Learn more here:
Early life trauma and adult leucocyte telomere length. ![]()
Sharonda is a PhD student in epidemiology at Boston University School of Public Health. She got started working with the Sister Study through the highly competitive NIH Summer Internship Program and has spent the last two summers studying important women's health issues. Her specific projects include examining the impact of gynecologic surgery (e.g. hysterectomies and oophorectomies) and hormone therapy use on breast cancer risk; and evaluating the extent to which experiencing trauma before age 18 may be related to pregnancy complications like gestational diabetes and hypertensive disorders. Both research topics highlight the importance of investigating how social and environmental factors influence health across the life course. In her future research, Sharonda hopes to further integrate her interests in cancer and trauma.
There are a few reasons why we might ask similar questions on multiple questionnaires from year to year. The main reason is that some things may change—you might lose or gain weight, start a new hobby, be prescribed a new medication, or develop a new medical condition, and we want to do our best to capture that information! Other times we realize that we did not originally ask the question in the best way and want you to provide additional or clarifying information. For example, we asked about your personal care product use (hair dyes, make-up, talc products, etc.) at enrollment, but focused specifically on use in your early adolescence and in the year before baseline. In later questionnaires, we asked about your recent (post-baseline) use and also tried to capture information about your lifetime use by asking about what products you used during each decade of your life.
August 7, 2022 is National Sisters Day: With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. On National Sisters Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
Heart disease is the leading cause of death for women in the United States. Over the years, we have asked you questions about your cardiovascular health and disease history. In August, we began requesting medical records to confirm diagnoses and obtain needed details about reported heart conditions such as results of tests performed and disease subtypes. Our goal is to identify preventable environmental causes of cardiovascular disease. We have reached out to some of you for more information about your health history. If you were contacted and returned your authorization forms, we thank you! However, if you have not yet done so we encourage you to sign and mail your forms soon. We are excited to let you know that we are working with cardiovascular disease experts to study environmental contributors to stroke, heart attack, and congestive heart failure. Dr. Joseph Engeda will be using data collected from medical records to study these cardiovascular conditions. Thank you again for your contributions to the Sister Study. We could not do this research without your willingness to participate!
We would like to introduce you to Dr. Kemi Ogunsina, the Sister Study's newest post-doctoral fellow. Dr. Kemi Ogunsina recently earned her doctoral degree in Epidemiology from the University Of Miami Miller School Of Medicine, Miami Florida. She joined Dr. Dale Sandler's group as a post-doctoral fellow at the National Institute of Environmental Health Sciences. Dr. Ogunsina's research focus is on cancer prevention and control, including health disparities. For her first Sister Study research project she is studying health disparities in the association of between fibroids and use of genital talc or douche. She will also be assessing the interplay between reproductive factors, environmental exposure to endocrine disrupting chemicals, and risk of thyroid diseases.

The Sister Study Team has staff across the nation, including in California, Ohio, Georgia, North Carolina, and Maryland! This photo only shows a small group of our staff that is local to North Carolina. Pictured are staff from our Advocate, Data Processing, Epidemiology, Help Desk, Fulfilment, and Operations Teams. As Sister Study participants, your primary contacts are our Help Desk Team and Advocates. Our Data Processing Team is busy processing your questionnaires as you return them to us. Our Epidemiology Team coordinates with researchers to support collaborations and publish papers. Our Fulfilment Team sends out over 100,000 pieces of mail each year to Sister Study participants. Our Operations Team supports the day to day of the Sister Study such as creating and updating the study website, answering participant questions, collecting medical records, and supporting participant retention. Together, we are here to serve you!
Experience of traumatic events—including sexual, physical, or emotional abuse, and financial hardships—is thought to influence breast cancer risk, but such events rarely occur in isolation, and little is known about how co-occurring traumas, particularly during early life, may impact breast cancer risk. Sister Study participants reported whether they experienced certain traumatic experiences during childhood and adolescence. Using that data, we identified six distinct patterns of early-life trauma in the cohort. About half of all Sister Study participants disclosed at least one traumatic experience before age 18. We reported that experiencing either sexual trauma and household dysfunction or medium levels of early-life trauma was suggestively associated with greater risk of developing breast cancer compared to experiencing low levels of early-life trauma. Furthermore, breast cancer risk due to early-life trauma appeared lower among participants who reported constant childhood social support. This research suggests that different types of early-life traumatic experiences may contribute to various levels of risk of breast cancer.
Learn more here:
Latent class models of early-life trauma and incident breast cancer. ![]()
Every summer, the National Institute of Environmental Health Sciences proudly hosts early career researchers participating in the NIH Summer Internship program. This year, eight interns from colleges and graduate schools across the country will be working on Sister Study-related research projects, studying topics such as air pollution, early life trauma, uterine fibroids, and diabetes. We look forward to seeing what they find and reporting the results back to you!
Learn more here:
Summer Internship Program in Biomedical Research. ![]()
Pregnancy is considered a "window of susceptibility" for breast cancer risk because changes to the breast during pregnancy may alter susceptibility to developing the disease later in life. Associations between pregnancy conditions and breast cancer risk may provide insight into how pregnancy relates to later cancer development. Some previous studies have found that women who experienced a gestational hypertensive disorder, including gestational hypertension, pre-eclampsia and eclampsia, have a reduced risk of breast cancer. In a recent analysis, Sister Study investigators examined whether history of a gestational hypertensive disorder was associated with breast cancer risk among women who have given birth at least once. They found that having a history of a gestational hypertensive disorder was not associated with breast cancer risk.
Learn more here:
Gestational hypertensive disorders and maternal breast cancer risk in a nationwide cohort of 40,720 parous women. ![]()
Meet Eva Bauer, the Sister Study's new Operations and Retention Manager. She leads the operationalization of all Sister Study efforts, including participant health update, data collection and special projects. In addition, she and her team work on tending to participant needs, answering questions, and reducing participant burden. Eva brings excellent health communication and project management skills, and works collaboratively across all of our study teams to keep us moving forward. She graduated from the University of North Carolina with her Master of Public Health. She is interested in chronic diseases, primarily cancer, women's health, public health and health services research, and health disparities. She joined the Sister Study in February 2021 and just recently took on this new role. Outside of work, Eva enjoys spending time with her family and friends as well as playing with her French Bulldogs Rascal and Rex. In her free time, you can find her doing Pilates, trying new restaurants and recipes, traveling or spending time outdoors. Some of Eva's favorite places she has traveled to include Istanbul, Gdansk and Whistler. Welcome, Eva, to the Sister Study team!
In addition to trying to better understand the causes of breast cancer, Sister Study researchers are interested in learning more about breast cancer survivors, including what factors might influence their health-related quality of life. In a recent study of 2,453 breast cancer survivors, we found that those with higher cancer stages, more concurrent conditions, surgical complications, or who were dissatisfied with their breast surgery or experienced breast cancer recurrences or new tumors had lower quality of life scores. Those with lower scores were more likely to die from their disease, even after controlling for disease stage and other factors. This research helps identify what areas are most important for improving care and survival rates of those diagnosed with breast cancer.
Learn more here:
Health-related quality of life outcomes among breast cancer survivors. ![]()
Sister Study investigators and researchers from Duke University examined the association between poor sleep patterns and risk of developing hypertension (high blood pressure). They found that women with insomnia (difficulty falling or staying asleep) or insomnia plus short sleep (<7 hours per night) were more likely to develop hypertension. These associations were stronger among younger and premenopausal women but did not differ by race/ethnicity. This research demonstrates how poor sleep may impact other aspects of health.
Learn more here:
A prospective study of multiple sleep dimensions and hypertension risk among white, black and Hispanic/Latina women: findings from the Sister Study. ![]()
Loss of sense of smell—or olfactory impairment—has been in the news because it is a common symptom of SARS CoV-2/COVID-19 infection. But olfactory impairment is important on its own—it increases with age and is a symptom of some neurodegenerative diseases, such as Parkinson's disease and Alzheimer's disease. Loss of sense of smell itself may have consequences, such as making food taste bad or not being able to smell smoke in a fire. Some Sister Study participants were invited to participate in further studies of sense of smell, including home "scratch and sniff" tests using a special booklet. An early report from that study found that women who were unable to accurately name the test scents usually under-reported how much difficulty that had smelling things. The olfactory impairment data are now being used to study environmental factors that might increase the likelihood of losing one's sense of smell. This work is being led by Sister Study collaborator, Dr. Honglei Chen at Michigan State University.
Learn more here:
Assessment of Self-reported Sense of Smell, Objective Testing, and Associated Factors in Middle-aged and Older Women. ![]()
Radon, which occurs naturally in the environment, can breakdown into radioactive particles called isotopes. These isotopes can bind to particles in air pollution. This allows the radioactive isotopes to be inhaled, which may lead increased cancer risk in exposed tissues. Building on previous Sister Study work showing that living in areas of higher exposure to air pollution was related to a higher risk of breast cancer, a new Sister Study investigation evaluated whether exposure to airborne radioactive particles was also associated with breast cancer risk. Investigators found that living in areas with higher airborne particle radioactivity was associated with a higher risk of ER-negative breast cancer. These results suggest that exposure to radioactive particles may be one way in which air pollution contributes to breast cancer risk.
Learn more here:
Exposure to Particle Radioactivity and Breast Cancer Risk in the Sister Study: A U.S.-Wide Prospective Cohort. ![]()
Gestational diabetes is a type of diabetes that develops during pregnancy. We used data from the Sister Study to better understand how the risk of developing type 2 diabetes is impacted by history of gestational diabetes. We observed that having had gestational diabetes was associated with an increased risk of developing type 2 diabetes, and that this risk remained elevated for more than 35 years after the affected pregnancy. We also observed that as the number of times a woman had gestational diabetes increased, the risk of developing type 2 diabetes also increased. Women with a history of gestational diabetes might want to discuss diabetes screening strategies with their physicians.
Learn more here:
Persistence of Risk for Type 2 Diabetes After Gestational Diabetes Mellitus. ![]()
A large collaborative research project sought to answer the question: is the optimal approach to breast cancer screening for women with ATM, CHEK2, and PALB2 pathogenic variants? These are genes that are strongly linked with increased breast cancer risk, although the risks are not as great as they are for BRCA1/2. The researchers estimated that annual mammography from age 40 to 74 years reduced breast cancer mortality by 36% to 39% in women with these variants. Screening via annual magnetic resonance imaging (MRI) before age 40, followed by annual screening with both MRI and mammography after age 40 was estimated to reduce breast cancer mortality by 54%- 60%. However, the use of both annual MRIs and mammographies before age 40 did not meaningfully reduce mortality, and also increased the number of false-positive screenings. This modeling analysis, which includes data from Sister Study participants, suggests that starting MRI screening before age 40 may substantially reduce breast cancer mortality for women with moderate- to high-risk pathogenic variants for breast cancer.
Learn more here:
Good Housekeeping: Can Dying Your Hair Raise Your Risk for Breast Cancer? Experts Explain. ![]()
Breast Cancer Screening Strategies for Women With ATM, CHEK2, and PALB2 Pathogenic Variants: A Comparative Modeling Analysis. ![]()
In the US, Hispanic/Latina women are more likely to be diagnosed with a later stage of breast cancer than non-Hispanic White women. Efforts to increase screening and reduce this disparity could be more effective if we understood the factors that contribute to this disparity. We wondered if birthplace played a role. We asked about screening methods, including mammography, ultrasound, and magnetic resonance imaging (MRI) on the initial Sister Study questionnaire. We categorized women as recently screened (≤2 years ago), formerly screened (>2 years ago), or never screened, finding that compared to US-born non-Hispanic/Latina White women, US-born Hispanic/Latina women were more likely to be formerly screened for breast cancer and foreign-born Hispanic/Latina women were more likely to have never received breast cancer screening. The intersectional identity of foreign-born Hispanic/Latina women amounts to unique barriers to accessing preventive healthcare services in the US.
Women with a strong family history of breast cancer have a higher risk of getting breast cancer themselves, but it is unclear whether environmental risk factors for breast cancer have stronger associations within higher risk groups. Building on prior Sister Study research ![]() showing there may be an association betweenair pollution and breast cancer risk
showing there may be an association betweenair pollution and breast cancer risk ![]() , newly published results indicate that nitrogen dioxide (NO2) concentrations are positively associated with breast cancer risk among those with very high family-based risk scores (>90th percentile), but not in those with lower estimated family risk scores. This research demonstrates that women with strong family histories of breast cancer may benefit more from interventions to reduce exposure to NO2.
, newly published results indicate that nitrogen dioxide (NO2) concentrations are positively associated with breast cancer risk among those with very high family-based risk scores (>90th percentile), but not in those with lower estimated family risk scores. This research demonstrates that women with strong family histories of breast cancer may benefit more from interventions to reduce exposure to NO2.
Learn more here:
Air Pollution and Breast Cancer: An Examination of Modification By Underlying Familial Breast Cancer Risk. ![]()
Anti-Müllerian hormone (AMH) is a blood-based measure of ovarian reserve that is indicative of a woman's reproductive life-span. In a recently published study, Sister Study investigators examined whether various measures of outdoor air pollution were associated with AMH concentrations among 883 Sister Study participants who were premenopausal at enrollment. They did not observe a consistent link between any of the air pollution measures and AMH, an indication that air pollution may not directly affect ovarian reserve.
Learn more here:
Outdoor air pollution and anti-Müllerian hormone concentrations in the Sister Study. ![]()
The Sister Study contributed to a large, pooled analysis looking at how some of the more commonly studied genetic mutations (or "variants") may be related to the risk of specific breast cancer subtypes. In a sample of more than 200,000 women, 10 of the 173 variants examined were associated with all of the subtypes, but many others were associated with either estrogen receptor positive breast cancer or triple-negative breast cancer, but not both. This work helps to deepen our understanding of the role of genetics in determining the risk of specific breast cancer subtypes.
Learn more here:
Common variants in breast cancer risk loci predispose to distinct tumor subtypes. ![]()
Thelarche is a term for the start of breast development during puberty. Thelarche often begins up to 2 years before the onset of menses. A previous Sister Study report showed that earlier age at thelarche is associated with increased breast cancer risk, but little is known about factors that influence the timing of thelarche. In a recent analysis, Sister Study investigators identified early-life factors associated with early thelarche, which they defined as age 10 or younger. They found that multiple prenatal factors were associated with early thelarche, including maternal gestational hypertensive disorder, diethylstilbestrol (DES) use, smoking during pregnancy, being firstborn, and being born to a teenage mother. This work helps us better understand how the early-life environment influences the timing of puberty and may also affect adult breast cancer risk.
Learn more here:
Early-life exposures and age at thelarche in the Sister Study cohort. ![]()
In addition to the known breast cancer genes, BRCA1 and BRCA2, other inherited genes are also important in breast cancer. Some are considered pathogenic, meaning they are predictive of an elevated breast cancer risk. In a very large study that included Sister Study participants, investigators found that the frequencies of inherited genetic mutations in 12 known pathogenic breast cancer genes did not vary by race (5.65% in Black women versus 5.06% in non-Hispanic white women). The biggest racial difference was seen for CHEK2, which was more common in non-Hispanic white women with breast cancer (1.29%) than Black women with breast cancer (0.38%). BRCA2 and PALB2 mutations were slightly more common in Black cases. The findings suggest that policy changes related to genetic testing should not be based on race and that all efforts should be made to ensure equal access and uptake to genetic testing.
The prevalence of hypertension (high blood pressure) varies by race/ethnicity. Many studies have shown that lower individual socioeconomic status is associated with higher risk of hypertension, but less is known about the association between neighborhood level socioeconomic factors and hypertension. Using an established measure that summarizes across many different census variables we found that women living in more disadvantaged neighborhoods had a higher prevalence of hypertension. Compared with non-Hispanic White women in the least disadvantaged neighborhoods, self-identified non-Hispanic Black woman with higher neighborhood disadvantage had the highest prevalence of hypertension. Physical activity tended to moderate some of the hypertension risk associated with neighborhood factors.
Learn more here:
Association between neighbourhood deprivation and hypertension in a US-wide Cohort. ![]()
Vitamin D may help prevent some cancers and other chronic diseases, but its relationship with breast cancer is not established. Vitamin D supplement use was common in the Sister Study. At the time of enrollment, 64% of participants reported regularly taking f a vitamin D-containing supplement We found that recent use of vitamin D-containing supplements (within the last 2-3 years) was associated with a reduced risk of breast cancer. Supplement use was less common among Black women (56%) and Latinas (50%) than non-Hispanic White women (66%), but we did not see clear differences in the relationship between vitamin D supplement use and breast cancer by race/ethnicity. Our findings are consistent with the hypothesis that vitamin D is inversely associated with breast cancer risk across all racial/ethnic groups.
Learn more here:
Vitamin D Supplement Use and Risk of Breast Cancer by Race-Ethnicity. ![]()
Most of what we know about the role of genes that confer high risk of breast cancer (BRCA1, BRCA2, CDH1, CHEK2, ATM, and PALB2) is based on their association with invasive ductal carcinoma, the most common form of breast cancer. Less is known about their role in invasive lobular carcinoma (ILC), which makes up about 10% of all breast cancers ![]() . In a recent collaborative study that includes some Sister Study participants, investigators showed that 5-6% of women with ILC have at least one mutation, or "pathogenic variant" in one of these known breast cancer risk genes. More specifically, pathogenic variants in CDH1, BRCA2, CHEK2, ATM, and PALB2 were associated with increased risk of ILC, but variants in BRCA1 were not. These results show that multigene panel testing is appropriate for women with ILC and to identify women at risk of ILC.
. In a recent collaborative study that includes some Sister Study participants, investigators showed that 5-6% of women with ILC have at least one mutation, or "pathogenic variant" in one of these known breast cancer risk genes. More specifically, pathogenic variants in CDH1, BRCA2, CHEK2, ATM, and PALB2 were associated with increased risk of ILC, but variants in BRCA1 were not. These results show that multigene panel testing is appropriate for women with ILC and to identify women at risk of ILC.
Learn more here:
Germline Pathogenic Variants in Cancer Predisposition Genes Among Women With Invasive Lobular Carcinoma of the Breast. ![]()
Sister Study investigators and researchers from Duke University examined the association between poor sleep patterns and risk of developing hypertension (high blood pressure). They found that women with insomnia (difficulty falling or staying asleep) or insomnia plus short sleep (<7 hours per night) were more likely to develop hypertension. These associations were stronger among younger and premenopausal women but did not differ by race/ethnicity. This research demonstrates how poor sleep may impact other aspects of health.
Learn more here:
A prospective study of multiple sleep dimensions and hypertension risk among white, black and Hispanic/Latina women: findings from the Sister Study. ![]()
The main reason is that some things may change—you might lose or gain weight, start a new hobby, be prescribed a new medication, or develop a new medical condition, and we want to do our best to capture that information! Other times we realize that we did not originally ask the question in the best way and want you to provide additional or clarifying information. For example, we asked about your personal care product use (hair dyes, make-up, talc products, etc.) at enrollment, but focused specifically on use in your early adolescence and in the year before you joined. In later questionnaires, we asked about your recent use (after you joined) and also tried to capture information about your lifetime use by asking about what products you used during each decade of your life.
Periodontal (gum) disease and tooth loss are common public health concerns and may be an indicator of more significant health problems. Researchers at the National Cancer Institute recently led an investigation of the associations of periodontal disease and tooth loss with mortality among Sister Study participants. They observed that women with periodontal disease, tooth loss, or both had higher overall mortality rates than women without those conditions. In terms of specific causes of death, having periodontal disease was associated with increased likelihood of dying from an infectious or parasitic disease, and having tooth loss was associated with increased risk of dying from cardiovascular, endocrine-related, or respiratory system diseases. This study supports the importance of maintaining good oral health.
Learn more here:
Associations of periodontal disease and tooth loss with all-cause and cause-specific mortality in the Sister Study. ![]()
Thanks to the health updates and other information you share year after year with the Sister Study, our researchers are able to publish papers such as this one. Please read about how a healthy diet may lower women's risk of age-related diseases and mortality.
Learn more here:
Diet holds key to slowing biological aging, researchers say. ![]()
Please welcome new Sister Study researcher Dr. Che-Jung Chang! Dr. Chang recently received her PhD in Environmental Health Science from Rollins School of Public Health, Emory University. She joined Dr. Alexandra White's group in September 2021 as a post-doctoral research fellow at the National Institute of Environmental Health Sciences. Her research will focus on how exposure to environmental pollutants play a role in developing and progressing reproductive cancers in women. For her first Sister Study research project, Dr. Chang will examine how personal care products, which may contain endocrine-disrupting chemicals, are related to female reproductive cancers.
Heart disease is the leading cause of death for women in the United States. Over the years, we have asked you questions about your cardiovascular health and disease history. In August, we began requesting medical records to confirm diagnoses and obtain needed details about reported heart conditions such as results of tests performed and disease subtypes. Our goal is to identify preventable environmental causes of cardiovascular disease. We have reached out to some of you for more information about your health history. If you were contacted and returned your authorization forms, we thank you! But if you haven't yet done so we encourage you to sign and mail your forms soon. We are excited to let you know that we are working with cardiovascular disease experts to study environmental contributors to stroke, heart attack, and congestive heart failure. Dr. Joseph Engeda, who recently joined the Sister Study team as an Epidemiologist, will be using data collected from medical records to study these cardiovascular conditions. Thank you again for your contributions to the Sister Study. We couldn't do this research without your willingness to participate!
While human papillomavirus (HPV) is the primary cause of cervical cancer, other factors may influence susceptibility and response to the virus. Using data from the Sister Study, we looked at whether genital talc use or douching were associated with the occurrence of cervical cancer. We observed a possible positive association between douching during adolescence and cervical cancer, but no association between adolescent talc use and cervical cancer. Recent (in the year before study enrollment) douching and to a lesser extent genital talc use were positively associated with incident cervical cancer, but the number of new cases was small. This research helps us understand some of the possible causes of cervical cancer and could help guide preventative strategies, particularly in areas with low HPV vaccination rates.
Learn more here:
The association between douching, genital talc use, and the risk of prevalent and incident cervical cancer. ![]()
Do you remember clipping your toenails and having them collected by our examiners when you enrolled in the Sister Study? We measured concentrations of 15 metals in the toenails from a subset of Sister Study women and studied whether those levels were associated with future breast cancer risk. We did not observe a relationship between most of the metals and breast cancer risk, either individually or as a combined metal exposure. One possible exception was that molybdenum, an essential element found in legumes, leafy vegetables, and milk, was associated with a reduced risk of breast cancer, particularly estrogen receptor negative breast cancer.
Learn more here:
Metals and Breast Cancer Risk: A Prospective Study Using Toenail Biomarkers. ![]()
On October 27, 2021, the FDA took several new actions to strengthen breast implant risk communication and help those who are considering breast implants make informed decisions. If you are considering breast implant or have received them in the past, we encourage you to talk to your personal doctor about these new recommendations.
Learn more here:
FDA Strengthens Breast Implant Safety Requirements and Updates Study Results. ![]()
This large collaborative study that included more than 26,000 women aimed to evaluate the importance of screening for known breast cancer genes in women over age 65. The study looked at the frequency of so called "pathogenic variants" (PVs), which are mutations in known breast cancer risk genes, including the most widely known BRCA1 and BRCA2 genes. PVs in BRCA1, BRCA2, and PALB2 were found in 3.4% of women diagnosed with estrogen receptor ER-negative, 1.0% with ER-positive, and 3.0% with triple-negative breast cancer. As expected, PVs in CHEK2, PALB2, BRCA1, and BRCA2 were associated with increased risks of breast cancer: remaining lifetime risks of breast cancer were ≥ 15% for those with PVs in BRCA1, BRCA2, and PALB2. While this remaining lifetime risk is not as great as it is for younger women, this study suggests that all women diagnosed with triple-negative breast cancer or ER-negative breast cancer should receive genetic testing and that women over age 65 years with BRCA1 and BRCA2 PVs and perhaps PALB2 and CHEK2 PVs should be considered for more advanced breast cancer screening such as with magnetic resonance imaging.
Learn more here:
Risk of Late-Onset Breast Cancer in Genetically Predisposed Women. ![]()
The age that menopause occurs is determined by the number of remaining ovarian follicles, often referred to as the ovarian reserve. Ovarian follicles are formed in very early life; the number of follicles is greatest at birth and decreases with age and menstruation, but environmental factors could also lead to decreased ovarian reserve. In a new Sister Study investigation, we examined possible associations between prenatal and childhood exposure to the farm environment and Anti-Müllerian hormone (AMH), a blood-based biological marker of ovarian reserve, in women ages 35-54 years. We found that women whose mothers worked or resided on a farm while they were pregnant had lower AMH levels. The data also suggested that childhood contact with pesticide-treated livestock or buildings was also associated with lower AMH. These findings raise concern that aspects of prenatal farm exposure may result in reduced adult ovarian reserve.
Learn more here:
Early-life Farm Exposure and Ovarian Reserve in a US Cohort of Women. ![]()
Researchers from the Sister Study have developed a new risk prediction score that may improve how we identify women at higher risk for developing breast cancer. The new risk score is based on measures of naturally occurring chemical modifications to DNA, known as DNA methylation, that can be assessed in the cells collected from a simple blood sample. In the Sister Study analysis, the investigators used blood samples that were provided at study enrollment and found that the new DNA methylation-based risk score helped predict whether or not a woman developed breast cancer during follow-up, especially when it was combined with existing information on other genetic or lifestyle factors. Though these results are novel and promising, further investigation and replication is needed to see if this will be useful in a clinical setting.
Learn more here:
Blood DNA methylation profiles improve breast cancer prediction. ![]()
Sister Study investigators teamed up with collaborators from Boston University and elsewhere to evaluate the potential association between gestational diabetes and young-onset breast cancer. For the analysis, we pooled data from 5 large cohort studies, including nearly 260,000 women, 6,842 of whom developed breast cancer before age 55. Women who had one or more children had a reduced risk of young-onset breast cancer, compared to women who never gave birth. Among women who gave birth, gestational diabetes was not associated with an increased risk of young-onset breast cancer.
Learn more here:
Gestational diabetes and risk of breast cancer before age 55 years. ![]()
October is Breast Cancer Awareness Month and we at the Sister Study would like to join our participants and friends of the study to remember those affected by breast cancer. With our ongoing research, we honor those we have lost and those who continue to fight against breast cancer. We are grateful to those of you who participate in research like the Sister Study so we can work together toward solutions. Thank you.
We would like to introduce you to Dr. Jennifer Ish, who recently earned her PhD in Epidemiology from the University of Texas Health Science Center School of Public Health and joined Dr. Alexandra White's group as a post-doctoral fellow at the National Institute of Environmental Health Sciences. Dr. Ish is interested in investigating the interplay between environmental, social, and psychosocial stressors and the mechanisms by which these factors influence the risk of adverse health outcomes in women and children. In her first project at NIEHS, she will be using data from the Sister Study to examine the effect of exposure to industrial air pollution on breast cancer risk. She will also investigate whether stress-related factors, such as race and neighborhood segregation, enhance susceptibility to toxic air emissions, potentially informing how air pollution contributes to disparities in breast cancer outcomes.
The Women's Health Awareness: Virtual Series "Real Talk With the Experts" is over, but you can learn more about the initiative here:
Women's Health Awareness.Almost 39,000 (76.6%) Sister Study participants have completed the special COVID-19 survey. Many of you have also completed either your Annual Health Update (85.6%) or your Detailed Health Update (84.0%). You are truly a dedicated and remarkable group! We thought it would interest you if we shared a bit on what we have learned thus far from the COVID-19 surveys:
- About 7.5% of responders have had COVID-19.
- Of those who have had COVID, approximately 5.6% tell us they were hospitalized as a result. Of those hospitalized, about 15.3% required rehab.
Thank you for helping our researchers learn how COVID-19 is impacting our Sister Study participants!
Overall dietary patterns may be stronger predictors of health than any individual food item or nutrients. Using the diet data you provided when you joined the Sister Study we studied three well-established healthy diets—the Dietary Approaches to Stop Hypertension (DASH) diet ![]() , the Mediterranean Diet
, the Mediterranean Diet ![]() and the Alternative Healthy Eating Index
and the Alternative Healthy Eating Index ![]() . We found that high adherence to the DASH diet scoring well on the Alternative Healthy Eating Index was associated with a reduced risk of breast cancer. There are common features of these healthy diets including eating lots of fruits and vegetables and limiting red meat.
. We found that high adherence to the DASH diet scoring well on the Alternative Healthy Eating Index was associated with a reduced risk of breast cancer. There are common features of these healthy diets including eating lots of fruits and vegetables and limiting red meat.
Learn more here:
Dietary index scores and invasive breast cancer risk among women with a family history of breast cancer. ![]()
In late July, the Sister Study summer interns presented their preliminary findings at the NIEHS virtual poster session. There were many fabulous projects, and several of our students won awards! We'd like to congratulate Yilda Macias ("COVID-19 and Vitamin D Supplement use by Race/Ethnicity in the Sister Study Cohort") and Rachel Thompson ("Associations between Serum Iron Biomarkers and Breast Cancer Tumor Size") for their 2nd place finishes. Sharonda Lovett ("Gynecologic Surgery, Hormone Therapy, and Incident Breast Cancer in the Sister Study") and Claire Ashley ("Use of Wood-Burning Stoves and Fireplaces and Select Cardiovascular Outcomes among Sister Study Participants") received honorable mentions. Stay tuned for more details on their findings - these students and their mentors are continuing to work on getting the results written up and submitted for publication.
We have shared a few recent articles using Sister Study data to analyze genes linked to breast cancer risk, including PALB2. Thanks to all the Sister Study participants whose data allows us to continue our research!
- The Sister Study contributed to a landmark study
 that examined how some of the genes with known links to cancer impact breast cancer risk in the general population. Most of the current information we have on risk associated with these genes comes from clinical studies of high risk patients and their families, not women in the general population. Variations in the BRCA1 and BRCA2 genes were associated with the highest risk of breast cancer, followed by variations in PALB2. Variations in the genes BARD1, RAD51C, and RAD51D were associated with increased risk of estrogen receptor negative and triple-negative breast cancer. This work helps us understand the overall impact of these rare mutations on women's risks of developing breast cancer.
that examined how some of the genes with known links to cancer impact breast cancer risk in the general population. Most of the current information we have on risk associated with these genes comes from clinical studies of high risk patients and their families, not women in the general population. Variations in the BRCA1 and BRCA2 genes were associated with the highest risk of breast cancer, followed by variations in PALB2. Variations in the genes BARD1, RAD51C, and RAD51D were associated with increased risk of estrogen receptor negative and triple-negative breast cancer. This work helps us understand the overall impact of these rare mutations on women's risks of developing breast cancer. - The breast cancer risk associated with cancer predisposition genes in African Americans is not well known, in part because few studies have been large enough to address this question. For that reason, researchers at Boston University and the Mayo Clinic collaborated with the Sister Study to analyze DNA from 5,054 African-American women with breast cancer and 4,993 African-American women without breast cancer. Their research focused on 23 cancer predisposition genes, including BRCA1, BRCA2, and PALB2. They found that the genes that greatly increase the risk of breast cancer in U.S. white women also greatly increase breast cancer risk among African-American women. Currently, rates of breast cancer genetic testing are substantially lower in African-American women with breast cancer than in white patients of the same ages. The authors cite differences in recommendations given to African American women as one of the drivers of this disparity.
- This large collaborative study
 that included more than 26,000 women aimed to evaluate the importance of screening for known breast cancer genes in women over age 65. The study looked at the frequency of so called
that included more than 26,000 women aimed to evaluate the importance of screening for known breast cancer genes in women over age 65. The study looked at the frequency of so called pathogenic variants
(PVs), which are mutations in known breast cancer risk genes, including the most widely known BRCA1 and BRCA2 genes. PVs in BRCA1, BRCA2, and PALB2 were found in 3.4% of women diagnosed with estrogen receptor ER-negative, 1.0% with ER-positive, and 3.0% with triple-negative breast cancer. As expected, PVs in CHEK2, PALB2, BRCA1, and BRCA2 were associated with increased risks of breast cancer: remaining lifetime risks of breast cancer were ≥ 15% for those with PVs in BRCA1, BRCA2, and PALB2. While this remaining lifetime risk is not as great as it is for younger women, this study suggests that all women diagnosed with triple-negative breast cancer or ER-negative breast cancer should receive genetic testing and that women over age 65 years with BRCA1 and BRCA2 PVs and perhaps PALB2 and CHEK2 PVs should be considered for more advanced breast cancer screening such as with magnetic resonance imaging.
One major area of interest for Sister Study researchers is the potential long-term health effects of personal care products, particularly those containing potentially harmful chemicals ![]() . We previously showed
. We previously showed ![]() that using permanent hair dye, straighteners, or perms
that using permanent hair dye, straighteners, or perms ![]() may be associated with an increased risk of breast cancer. In a recent examination of the association between hair products and ovarian cancer risk, we found that frequent use of hair straighteners/relaxers (>4 times/year) was associated with twice the risk of ovarian cancer compared to never users. This finding is particularly relevant for Black/African American women, who are more likely to use straighteners/relaxers.
may be associated with an increased risk of breast cancer. In a recent examination of the association between hair products and ovarian cancer risk, we found that frequent use of hair straighteners/relaxers (>4 times/year) was associated with twice the risk of ovarian cancer compared to never users. This finding is particularly relevant for Black/African American women, who are more likely to use straighteners/relaxers.
Learn more here:
Use of hair products in relation to ovarian cancer risk. ![]()
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Sisters Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
In one of the follow-up questionnaires, we asked Sister Study participants about their experiences with discrimination. We defined 'everyday' discrimination as being treated unfairly receiving while receiving a service, being treated as less intelligent or worthy, or experiencing people acting as if they were afraid of you. We defined 'major' discrimination as being specific to a particular event (e.g., being treated unfairly when renting or buying a house; being treated unfairly by the police; being treated unfairly at work). Non-Hispanic Black Sister Study participants were more likely to report having experienced everyday (75%) or major (51%) discrimination because of their race/ethnicity, relative to Non-Hispanic White (4% everyday, 2% major) or Hispanic/Latina participants (32% everyday, 16% major). While everyday discrimination was not associated with the risk of developing type 2 diabetes during follow-up, experiencing major discrimination was associated with an increased risk. This work provides evidence that anti-discrimination efforts may help mitigate racial/ethnic disparities in the risk of type 2 diabetes.
In a sample of Sister Study and Two Sister Study participants with breast cancer, we looked at measures of financial hardship after diagnosis. Among the 1628 breast cancer survivors who were employed at diagnosis, 27% reported employment disruption (15% stopped working; 12% had reduced hours), and 21% experienced financial hardship (16% had difficulty paying for care; 13% borrowed money or incurred debt; 2% filed for bankruptcy). These results demonstrate how women experiencing employment disruptions after breast cancer may be vulnerable to financial hardship and highlight the need to identify risk factors for employment disruption and ways to help mitigate financial consequences after cancer.
Learn more here:
Breast Cancer-Related Employment Disruption and Financial Hardship in the Sister Study. ![]()
Building off Sister Study research that showed various measures of body composition and physical activity ![]() were associated with a woman's "biological age", we wanted to see if alcohol intake also potentially contributed to aging. We did not find strong evidence that recent or lifetime alcohol use was associated with biological age. As a possible exception, women averaging approximately 1 drink/day for each year they drank alcohol had a biological age measure that was consistent with being about 9 months to one year older than their chronological age would suggest.
were associated with a woman's "biological age", we wanted to see if alcohol intake also potentially contributed to aging. We did not find strong evidence that recent or lifetime alcohol use was associated with biological age. As a possible exception, women averaging approximately 1 drink/day for each year they drank alcohol had a biological age measure that was consistent with being about 9 months to one year older than their chronological age would suggest.
Learn more here:
Alcohol Consumption and Methylation-Based Measures of Biological Age. ![]()
Over 31,000 (61.4%) Sister Study participants have completed the special COVID-19 survey. Many of you have also completed either your Annual Health Update (82.4%) or your Detailed Health Update (74.5%). You are truly a dedicated and remarkable group! We thought it would interest you if we shared a bit on what we have learned thus far from the COVID-19 surveys:
- About 6.7% of responders have had COVID-19.
- Of those who have had COVID, approximately 5.2% tell us they were hospitalized as a result. Of those hospitalized, about 9.7% required rehab.
Thank you for helping our researchers learn how COVID-19 is impacting our Sister Study participants!
NIEHS post-doctoral fellow, Dr. Kaitlyn Lawrence, recently won an award for her research on the link between higher neighborhood deprivation and accelerated biological aging measures in the Sister Study. Congrats to Kaitlyn!
Learn more here:
Scientific Journeys: From summer intern to award-winning researcher. ![]()
The Sister Study contributed to a landmark study that examined how some of the genes with known links to cancer impact breast cancer risk in the general population. Most of the current information we have on risk associated with these genes comes from clinical studies of high risk patients and their families, not women in the general population. Variations in the BRCA1 and BRCA2 genes were associated with the highest risk of breast cancer, followed by variations in PALB2. Variations in the genes BARD1, RAD51C, and RAD51D were associated with increased risk of estrogen receptor negative and triple-negative breast cancer. This work helps us understand the overall impact of these rare mutations on women's risks of developing breast cancer.
Learn more here:
A Population-Based Study of Genes Previously Implicated in Breast Cancer. ![]()
We recently published a study ![]() that looked at the association between type 2 diabetes, metformin use, and breast cancer risk. This newly published commentary further discusses these findings, which showed that while type 2 diabetes may increase the risk of developing breast cancer, the widespread use of metformin appears to counteract the hazards of long-term metabolic changes associated with type 2 diabetes.
that looked at the association between type 2 diabetes, metformin use, and breast cancer risk. This newly published commentary further discusses these findings, which showed that while type 2 diabetes may increase the risk of developing breast cancer, the widespread use of metformin appears to counteract the hazards of long-term metabolic changes associated with type 2 diabetes.
Read the cpmmentary here:
Making sense of associations between type 2 diabetes, metformin, and breast cancer risk. ![]()
This summer, the Sister Study will be welcoming 8 students into our (virtual) summer internship program. These undergraduate and graduate level students live all over the country and will be working with NIEHS investigators for 8-12 weeks, focusing on specific research questions that can be studied using Sister Study data. Students will be exploring how the following factors are related to breast cancer risk: thyroid diseases and treatment with radioactive iodine, history of gynecologic surgery (hysterectomy and oophorectomy), sedentary behavior (time spent sitting), and redlining (residential racial segregation due to lending and mortgage discrimination). Other students will consider how vitamin D supplement use is related to COVID-19 infections and severity; how wood smoke is related to lung cancer and cardiovascular disease; how blood iron levels are related to breast tumor size among women with breast cancer; and how sleep is related to insulin resistance measures. Please stay tuned for updates on their research.
Collaborators at the University of Wisconsin - Milwaukee examined the association between measures of childhood socioeconomic status and depression in adulthood. Approximately 17% of Sister Study participants reported being diagnosed with depression between age 30 and when they enrolled in the study. Those who perceived their families as relatively disadvantaged during their childhood were more likely to have reported depression. The relationship was less clear when the researchers considered the relationship between parents' education levels (more objective measures of socioeconomic status) and depression, noting that the relationship may vary across birth year and time.
Learn more here:
Objective and subjective childhood socioeconomic disadvantage and incident depression in adulthood: a longitudinal analysis in the Sister Study. ![]()
Inflammation and oxidative stress may promote breast and other cancers. The role of diet is still uncertain, however. In this study, Sister Study authors examined how the Dietary Inflammatory Index (DII) ![]() and dietary oxidative-balance scores (D-OBS)
and dietary oxidative-balance scores (D-OBS) ![]() may be related to breast cancer. They found that diet may indeed be associated with an increased risk of both overall and especially triple-negative breast cancer. The greatest risk was seen in diets with the poorest pro-inflammatory and pro-oxidative scores combined. These results suggest that modifying dietary lifestyle factors may help reduce the risk of breast cancer.
may be related to breast cancer. They found that diet may indeed be associated with an increased risk of both overall and especially triple-negative breast cancer. The greatest risk was seen in diets with the poorest pro-inflammatory and pro-oxidative scores combined. These results suggest that modifying dietary lifestyle factors may help reduce the risk of breast cancer.
Learn more here:
Dietary inflammatory potential, oxidative balance score, and risk of breast cancer: Findings from the Sister Study. ![]()
Some African-American/ Black Sister Study participants were included in a large, collaborative study of genetic risk factors for breast cancer among women with African ancestry. The lead investigators were interested in understanding how summary measures of genetic risk, called polygenic risk scores
, would be associated with breast cancer in Black women. They found that the scores were strongly associated with breast cancer risk in women of African descent, though they were better predictors of risk in women of European, Asian or Latino descent. These results demonstrate that while there are many genetic similarities across these populations, more research is needed to identify variants that better predict risk among women of African ancestry.
Learn more here:
Evaluating Polygenic Risk Scores for Breast Cancer in Women of African Ancestry. ![]()
With the Sister Study, we are trying to understand how shared genetics and life experiences can affect the health of our participants whose sisters were diagnosed with breast cancer. But, we know these sisterly bonds are much stronger and deeper than anything our science can capture. Many of you joined our study to honor your sister who experienced breast cancer, and you have continued to convey your love for your sisters by remembering them and sharing their experiences here on our Facebook page. Today, on National Siblings Day we pause to think of your sisterly bonds and express our appreciation for what it brings to cancer research and future generations. Thank you for your dedication to your sisters and our study!
Past research ![]() from the Sister Study showed that women with a higher "biological age", as measured by changes to certain genetic markers, appeared to be at increased risk for breast cancer. This finding made us wonder: what factors are associated with biological aging? In a recent analysis, Sister Study researchers found that women with a higher body mass index, waist-to-hip ratio, or waist circumference had higher biological ages. Fortunately, researchers also found that increasing physical activity was associated with lower biological age, especially among women with larger body sizes. These findings are exciting because they help us understand what factors might contribute to how our bodies age and how that may relate to breast cancer risk.
from the Sister Study showed that women with a higher "biological age", as measured by changes to certain genetic markers, appeared to be at increased risk for breast cancer. This finding made us wonder: what factors are associated with biological aging? In a recent analysis, Sister Study researchers found that women with a higher body mass index, waist-to-hip ratio, or waist circumference had higher biological ages. Fortunately, researchers also found that increasing physical activity was associated with lower biological age, especially among women with larger body sizes. These findings are exciting because they help us understand what factors might contribute to how our bodies age and how that may relate to breast cancer risk.
Learn more here:
Associations of Body Composition and Physical Activity Level With Multiple Measures of Epigenetic Age Acceleration. ![]()
Puberty is a period of rapid hormonal changes and breast development. Earlier age at menarche (a woman's first menstrual period) is known to be associated with increased breast cancer risk. In a recent analysis, Sister Study investigators examined whether early onset of breast development, also known as thelarche, is also associated with breast cancer risk. They found that earlier age at thelarche and earlier age at menarche were each associated with increased breast cancer risk, and that experiencing both early menarche (before age 12) and early thelarche (before age 10) together was associated with a greater increase in risk than either factor on its own. This work helps us better understand how early life factors may influence adult breast cancer risk.
Learn more here:
Pubertal timing and breast cancer risk in the Sister Study cohort. ![]()
We previously posted that the Environmental Protection Agency routinely measures potentially toxic chemicals in the air ![]() across the United States. This includes metals, including arsenic, cadmium, chromium, cobalt, lead, manganese, mercury, nickel, selenium, and antimony. In a recent Sister Study analysis, we looked at whether these metals are associated with hypertension (high blood pressure). We observed that those whose residential addresses were located in areas of high estimated arsenic, lead, chromium, cobalt, or manganese were more likely to have hypertension, but that those potentially exposed to high levels of airborne selenium were less likely to have hypertension. This study adds to the evidence that environment you live in can affect health.
across the United States. This includes metals, including arsenic, cadmium, chromium, cobalt, lead, manganese, mercury, nickel, selenium, and antimony. In a recent Sister Study analysis, we looked at whether these metals are associated with hypertension (high blood pressure). We observed that those whose residential addresses were located in areas of high estimated arsenic, lead, chromium, cobalt, or manganese were more likely to have hypertension, but that those potentially exposed to high levels of airborne selenium were less likely to have hypertension. This study adds to the evidence that environment you live in can affect health.
Learn more here:
Airborne metals exposure and risk of hypertension in the Sister Study. ![]()
We hope you and your family are staying healthy in these challenging times. We are so relieved that COVID-19 rates are decreasing and that the vaccine is available for many of you. Whether you have had COVID-19 or not, we encourage you to take a few minutes each day to log your health status in the COVID-19 symptom tracker. Your data is useful, even if you have been vaccinated, as it may help us understand how effective the different vaccines are in protecting us against infections or in preventing serious disease. Thank you if you are already tracking! The secure app is free to download and many large studies, including the Sister Study, are asking participants to use the app so that researchers and public health officials can get good information on the spread of this disease and its symptoms. If you enroll as a member of a cohort study and select The Sister Study, we will later be able to link the data you enter in the tracker with data you already gave us to identify factors that affected the likelihood of developing COVID-19 and learn if the virus has any long-term health impacts. The tracker collects data that complements what we are collecting with our own COVID questionnaire and because some people report daily, the APP provides data that can be used to track the spread of COVID in your community. Your friends and family can download the app and participate too, even if they are not involved in the Sister Study.
Learn more here:
COVID Symptom Study. ![]()
Over 20,000 (40%) Sister Study participants have completed the special COVID-19 survey. Many of you have also completed either your Annual Health Update (57%) or your Detailed Health Update (50%). You are truly a dedicated and remarkable group! We thought it would interest you if we shared a bit on what we have learned thus far from the COVID-19 surveys:
- Roughly 6% of responders have had COVID-19.
- Of those who have had COVID, approximately 5% tell us they were hospitalized as a result. Of those hospitalized, about 10% required rehab.
Thank you for helping our researchers learn how COVID-19 is impacting our Sister Study participants!
Since we began analyzing the data provided by our generous Sister Study sisters, our researchers have published over 200 scientific papers! These findings contribute to improvements in our understanding of the environmental and genetic causes of breast cancer and other important issues in women's health. We are proud of what we have accomplished together with our study sisters! Thank you for sticking with us!
To view Sister Study findings:
Research Articles. ![]()
Previous research ![]() by Sister Study researcher Dr. Alexandra White demonstrated that air pollution may be associated with breast cancer, but that the association may vary by geographic region. This variability is attributed to differences in the types of airborne particles (called "particulate matter") more common in each region. Dr. White pursued this research further with a second study of air pollution and breast cancer, this time in the Black Women's Health Study, a large cohort of Black women living throughout the US. In this newly published work, air pollution was associated with breast cancer in the Midwest, where the particulate matter was composed of chemicals associated with industrial processes. Taken together with our findings in Sister Study, this work underscores the importance of considering air pollution composition when evaluating health effects.
by Sister Study researcher Dr. Alexandra White demonstrated that air pollution may be associated with breast cancer, but that the association may vary by geographic region. This variability is attributed to differences in the types of airborne particles (called "particulate matter") more common in each region. Dr. White pursued this research further with a second study of air pollution and breast cancer, this time in the Black Women's Health Study, a large cohort of Black women living throughout the US. In this newly published work, air pollution was associated with breast cancer in the Midwest, where the particulate matter was composed of chemicals associated with industrial processes. Taken together with our findings in Sister Study, this work underscores the importance of considering air pollution composition when evaluating health effects.
Learn more here:
Air pollution and breast cancer risk in the Black Women's Health Study. ![]()
Women may apply powder to the genital area to help manage excess moisture and odor. However, powders often contain talc and other substances that potentially irritate and inflame tissues and promote carcinogenesis in female reproductive organs. We previously published a study of powder use and ovarian cancer ![]() with inconclusive findings. In a new publication, Sister Study investigated possible associations between powder use and uterine cancer using data on more than 209,000 women in four prospective cohorts, including the Sister Study. Analyses show that overall, 37 percent of women reported ever using genital powder, and 3272 invasive uterine cancers were documented across the study cohorts. Uterine cancer risk was not associated with genital powder use, with the possible exception of a slightly elevated risk among long-term users.
with inconclusive findings. In a new publication, Sister Study investigated possible associations between powder use and uterine cancer using data on more than 209,000 women in four prospective cohorts, including the Sister Study. Analyses show that overall, 37 percent of women reported ever using genital powder, and 3272 invasive uterine cancers were documented across the study cohorts. Uterine cancer risk was not associated with genital powder use, with the possible exception of a slightly elevated risk among long-term users.
Learn more here:
Genital powder use and risk of uterine cancer: A pooled analysis of prospective studies. ![]()
A few years ago, as part of a special survey of cancer survivors, we asked women who had been diagnosed with breast cancer to answer questions about their breast cancer and their current health and quality of life. Among the 1675 women who were employed at the time of their diagnosis, the 17% who were not employed at the time the special survey was administered were older and more likely to have peripheral neuropathy, lack sick leave, have later stage at diagnosis, have a recurrence or a new cancer, have problems with memory or attention, or have poor general health. These findings ![]() highlight some of the challenges cancer survivors face if they try to remain in the workforce after their diagnosis.
highlight some of the challenges cancer survivors face if they try to remain in the workforce after their diagnosis.
Learn more here:
Employment After Breast Cancer Diagnosis and Treatment Among Women in the Sister and the Two Sister Studies. ![]()
A study of 44,541 women has found that there appears to be no association between type 2 diabetes and developing breast cancer overall. This may be because most women in the study with type 2 diabetes were taking metformin, a medication widely used to treat type 2 diabetes, whose actions may help to reduce the risk of developing estrogen receptor positive breast cancer. While type 2 diabetes was not associated with increased risk of estrogen receptor positive breast cancer in this study, it was associated with a small increase in risk for estrogen receptor negative and triple negative breast cancer.
Press release:
Metformin may affect risk of breast cancer in women with type 2 diabetes. ![]()
Article:
A prospective study of type 2 diabetes, metformin use, and risk of breast cancer. ![]()
The Sister Study contributed to a landmark study that examined how some of the genes with known links to cancer impact breast cancer risk in the general population. Most of the current information we have on risk associated with these genes comes from clinical studies of high risk patients and their families, not women in the general population. Variations in the BRCA1 and BRCA2 genes were associated with the highest risk of breast cancer, followed by variations in PALB2. Variations in the genes BARD1, RAD51C, and RAD51D were associated with increased risk of estrogen receptor negative and triple-negative breast cancer. This work helps us understand the overall impact of these rare mutations on women's risks of developing breast cancer.
Learn more here:
A Population-Based Study of Genes Previously Implicated in Breast Cancer. ![]()
Iron is essential to life, but also potentially toxic at higher levels. In the Sister Study, we looked at the association between breast cancer risk and levels of iron in the blood. We found little evidence to support an association between higher blood iron levels and breast cancer risk.
Learn more here:
Association Between Serum Iron Biomarkers and Breast Cancer. ![]()
In addition to trying to better understand the causes of breast cancer, Sister Study researchers are interested in learning more about breast cancer survivors, including what factors might influence their health-related quality of life. In a recent study ![]() of 2,453 breast cancer survivors, we found that those with higher cancer stages, more concurrent conditions, surgical complications, or who were dissatisfied with their breast surgery or experienced breast cancer recurrences or new tumors had lower quality of life scores. Those with lower scores were more likely to die from their disease, even after controlling for disease stage and other factors. This research helps identify what areas are most important for improving care and survival rates of those diagnosed with breast cancer.
of 2,453 breast cancer survivors, we found that those with higher cancer stages, more concurrent conditions, surgical complications, or who were dissatisfied with their breast surgery or experienced breast cancer recurrences or new tumors had lower quality of life scores. Those with lower scores were more likely to die from their disease, even after controlling for disease stage and other factors. This research helps identify what areas are most important for improving care and survival rates of those diagnosed with breast cancer.
Learn more here:
Health-related quality of life outcomes among breast cancer survivors. ![]()
Puberty is a period of rapid hormonal changes and breast development. Earlier age at menarche (a woman's first menstrual period) is known to be associated with increased breast cancer risk. In a recent analysis, Sister Study investigators examined whether early onset of breast development, also known as thelarche, is also associated with breast cancer risk. They found that earlier age at thelarche and earlier age at menarche were each associated with increased breast cancer risk, and that experiencing both early menarche (before age 12) and early thelarche (before age 10) together was associated with a greater increase in risk than either factor on its own. This work helps us better understand how early life factors may influence adult breast cancer risk.
Learn more here:
Pubertal timing and breast cancer risk in the Sister Study cohort. ![]()
Ann Von Holle is a postdoctoral fellow in the Biostatistics and Computational Biology Branch at NIEHS and member of the Sister Study team. She completed her doctorate in epidemiology at UNC Chapel Hill in 2018. Since coming to NIEHS, she has been studying factors related to breast cancer incidence, including a study looking at whether sisters with breast cancer were diagnosed at similar ages, and a study considering how BMI, age and menopausal status act together to affect breast cancer risk. In other work, Ann is studying how blood iron levels may be related to breast cancer risk.
Learn more here:
More about Dr. Von Holle's research. ![]()
We introduced you to Dr. Ann Von Holle (here), a postdoctoral fellow in the Biostatistics and Computational Biology Branch at NIEHS and member of the Sister Study team. Dr. Von Holle is lead author on a recently published paper pointing to evidence for familial clustering in breast cancer age of onset. If sisters with breast cancer tend to get diagnosed around the same age, there could be important implications for both personalized screening and understanding the causes of breast cancer. With data from the Sister Study, we explored whether breast cancer risk was higher around the age at which an older sister was diagnosed and found evidence to support this hypothesis. If confirmed in additional studies, personalized screening for those who have a sister previously affected by the disease could account for how close they are to the age at which their sister was diagnosed.
Learn more here:
Evidence for Familial Clustering in Breast Cancer Age of Onset. ![]()
Some of you may have heard about California's decision to ban certain chemicals from personal care products. We thought you'd like to know that a Sister Study paper on hair products and increased risk of breast cancer is often cited as one of the reasons for creating this law!
Learn more:
California Ban - New California law banning toxic chemicals in cosmetics will transform industry ![]()
Sister Study Paper - Hair dye and chemical straightener use and breast cancer risk in a large US population of black and white women ![]()
Because they are so rare, researchers often include peritoneal (from the abdominal cavity membrane) and fallopian tube cancers in studies of ovarian cancer. The Sister Study contributed to a large collaborative effort to tease apart potential differences in risk factors by tumor site. The results of this study showed that most associations did not vary by location, ![]() providing evidence that these three types of cancer likely have similar causes.
providing evidence that these three types of cancer likely have similar causes.
Learn more:
Ovarian Cancer Risk Factor Associations by Primary Anatomic Site: The Ovarian Cancer Cohort Consortium ![]()
Earlier age at menopause is thought to be associated with a lower risk of breast, endometrial and ovarian cancer but increased risk of other chronic diseases such as heart disease. In a recent analysis, Sister Study investigators examined whether exposure to certain metals, as measured in toenail specimens collected from participants at enrollment, was associated with age at menopause. They found that while no individual metal was strongly associated with onset of menopause, lower overall metal levels, particularly essential metals such selenium, zinc, and manganese, were associated with earlier age at menopause.
Learn more here:
Toenail metal concentrations and age at menopause,
A prospective study. ![]()
At enrollment, 22% of Sister Study participants reported a history of periodontal disease, or chronic infection and inflammation of the gums. Periodontal disease is thought to be associated with oral, lung and gastrointestinal cancers, possibly because these tissues have an inflammatory response to bacteria spreading from the gums. The association with breast cancer is not known. In a recent collaboration with investigators from the National Cancer Institute, we did not see a clear association between periodontal disease and overall breast cancer risk, though there was some suggestion that periodontal disease is associated with lower risk of ductal carcinoma in situ but a higher risk of invasive disease. More research is needed to understand this discrepancy.
Learn more here:
The Association Between Periodontal Disease and Breast Cancer in a Prospective Cohort Study. ![]()
Dr. Jacob Kresovich is a Sister Study researcher and post-doctoral fellow in the Epidemiology Branch at NIEHS. His research explores how a naturally occurring chemical modifications to DNA, called DNA methylation, are related to aging and disease risk. He previously showed that a higher "biological age", as measured changes to DNA methylation, was associated with increased likelihood of developing breast cancer. Currently, he is studying how biological aging is affected by modifiable lifestyle factors such as physical activity and alcohol use.
There are likely some differences in the underlying causes of breast cancer diagnosed before or after menopause. The "Two Sister Study" was an initiative led by Dr. Clarice Weinberg in which we collected information from some of your sisters who had young-onset disease, thereby giving us the opportunity to study risk factors for breast cancer diagnosed before age 50. We recently used data from this companion study to look at whether features of your mother's pregnancy with you and your birth might affect risk of developing breast cancer at a young age. We observed that having a mother with pre-eclampsia (a serious form of pregnancy-related high blood pressure) was associated with increased risk of developing young-onset disease. We also observed a positive association between higher birth weight and young-onset breast cancer.
Learn more here:
Perinatal and postnatal exposures and risk of young-onset breast cancer ![]()
We have known for a long time that there are many different types of breast cancer and that each subtype likely has some unique risk factors. However, because hormone receptor positive breast cancer is the most common, it has been much easier to identify factors associated with that subtype. In a recently published international collaboration, researchers pooled data to examine genetic risk factors for each subtype separately. They identified 32 previously unknown markers! This information will be useful for understanding the genetic origins of some of the rarer subtypes, including triple-negative disease, and for developing genetic risk scores to predict what individuals are at the highest risk of developing one or more breast cancer subtypes.
Learn more here:
Genome-wide association study identifies 32 novel breast cancer susceptibility loci from overall and subtype-specific analyses. ![]()
Researchers from Dartmouth recently conducted ![]() a study comparing mercury levels in toenail samples from select Sister Study participants to those taken from individuals with amyotrophic lateral sclerosis (ALS). They observed that ALS patients were more likely to have very high mercury concentrations (above the 90th percentile) than our participants. The Sister Study toenail measurements were from an earlier study
a study comparing mercury levels in toenail samples from select Sister Study participants to those taken from individuals with amyotrophic lateral sclerosis (ALS). They observed that ALS patients were more likely to have very high mercury concentrations (above the 90th percentile) than our participants. The Sister Study toenail measurements were from an earlier study ![]() where we showed that toenail metal concentrations were not associated with young-onset breast cancer. Thank you for all you have shared with the Sister Study so researchers can continue to make an impact.
where we showed that toenail metal concentrations were not associated with young-onset breast cancer. Thank you for all you have shared with the Sister Study so researchers can continue to make an impact.
Learn more here:
Keratinous biomarker of mercury exposure associated with amyotrophic lateral sclerosis risk in a nationwide U.S. study. ![]()
Toenail-Based Metal Concentrations and Young-Onset Breast Cancer. ![]()
As many of you know, we are asking our participants to report any symptoms (or lack thereof) through the COVID-19 symptom study and app ![]() . Thank you for continuing to use the symptom tracker and for encouraging others to also use it!
. Thank you for continuing to use the symptom tracker and for encouraging others to also use it!
A few things that we really like about the app are:
- It can help identify emerging outbreaks by capturing data quickly and in real-time. You and millions of others are contributing to this research just by logging in and reporting your symptoms every day.
- It helped identify anosmia (loss of sense of smell) as a good predictor of having a coronavirus infection.
- We have already collected a lot of information about your existing health conditions, medication use, and genetics. With the data collected from the app, we will be able to look out how these factors might be related to whether or not you get infected or how serious your symptoms are.
- We are able to do all of this while still protecting your privacy. The app developers and other scientists involved will have access to the data that you enter into the app, but we will not share any of the data that we collected specifically for the Sister Study.
If you'd like a more scientific look at how this app can contribute to public health, we recommend checking out these recently published articles:
- The COronavirus Pandemic Epidemiology (COPE) Consortium: A Call to Action

- Rapid implementation of mobile technology for real-time epidemiology of COVID-19

Your friends and family can download the app and participate too, even if they are not involved in the Sister Study.
Please visit https://covid.joinzoe.com/us ![]() for more information.
for more information.
Congratulations to Sister Study researcher Dr. Chandra Jackson who received an award jointly funded by the National Institutes of Environmental Health Sciences and National Institute of Aging. With this award, Dr. Jackson will study how neighborhood environments and sleep health are related to cardiometabolic function. This work builds on her published research on sleep and metabolic disorders, including a study showing that not getting enough sleep or having insomnia may be associated with certain metabolic disorders in the Sister Study.
Learn more:
Multiple poor sleep characteristics and metabolic abnormalities consistent with metabolic syndrome among white, black, and Hispanic/Latina women: modification by menopausal statusDr. Jennifer Woo is the first graduate of the PhD in Epidemiology program at the University of Wisconsin-Milwaukee, Joseph J. Zilber School of Public Health. Using data from the Sister Study, her dissertation focused on how early life trauma may affect adult health, including breast cancer risk and biological markers of stress and aging. Dr. Woo is joining Dr. Dale Sandler's group as a post-doctoral fellow at the National Institute of Environmental Health Sciences and will be continuing to do research using data from the Sister Study. She hopes to learn more about how trauma and other early life experiences affect the body and influence individuals' risks of developing autoimmune or other chronic diseases.
Dr. Mary V. Díaz Santana received her Master's degree in Epidemiology from the University of Puerto Rico, Medical Science Campus and later completed a PhD in Epidemiology at the University of Massachusetts-Amherst. Her doctoral work focused on the role of acculturation in cancer screening among Hispanic women as well as the role of phthalate (a family of chemicals that are used in cosmetics as solvents and to make PVC plastic more flexible) exposure in breast cancer risk and weight change. As a postdoctoral fellow and Sister Study researcher, Dr. Díaz Santana is currently studying prenatal risk factors for breast cancer and diabetes. Dr. Díaz Santana is most interested in lessening the burden of chronic diseases among Hispanics, and plans to examine risk factors for breast cancer subtypes in Hispanic women participating in the Sister Study.
We hope you and your family are staying healthy in these challenging times. As you may know, COVID-19 has proven difficult to track. Whether you have COVID-19 or not, we encourage you to take a few minutes each day to log your health status in the new COVID-19 symptom tracker ![]() . The secure app is free to download and many large studies, including the Sister Study, are asking participants to use the app so that researchers and public health officials can get good information on the spread of this disease and its symptoms. If you enroll as a member of a cohort study and select The Sister Study, we will later be able to link the data you enter in the tracker with data you already gave us to identify factors that affected the likelihood of developing COVID-19 and learn if the virus has any long-term health impacts. Your friends and family can download the app and participate too, even if they are not involved in the Sister Study.
. The secure app is free to download and many large studies, including the Sister Study, are asking participants to use the app so that researchers and public health officials can get good information on the spread of this disease and its symptoms. If you enroll as a member of a cohort study and select The Sister Study, we will later be able to link the data you enter in the tracker with data you already gave us to identify factors that affected the likelihood of developing COVID-19 and learn if the virus has any long-term health impacts. Your friends and family can download the app and participate too, even if they are not involved in the Sister Study.
Please visit https://covid.joinzoe.com/us ![]() for more information.
for more information.
In a pooled analysis lead by Sister Study researchers, we observed a small, positive, but not statistically significant association between self-reported use of powder on the genital area and risk of ovarian cancer. Altogether, the study included 252,745 women from 4 large observational studies, 2168 of whom developed ovarian cancer. The observed positive association may be limited to women with intact reproductive tracts (i.e., women who have not had a hysterectomy or tubal ligation). We did not observe an association between duration or frequency of genital powder use and ovarian cancer risk. Though the results are not definitive, this is the largest study of the topic to date. It also improves upon some of the design limitations of earlier studies, which had previously suggested there is a modest, positive association between genital powder use and ovarian cancer risk.
Learn more here:
Association of Powder Use in the Genital Area With Risk of Ovarian Cancer ![]()
More than 3,000 papers were published by National Institute of Environmental Health Sciences researchers or grantees in 2019. The institute's leaders selected 26 for special recognition as Papers of the Year, including 3 Sister Study papers: "DNA methylation changes occur years before breast cancer develops", "Artificial light while sleeping may lead to obesity in women" and "Study finds eating processed meat increases colorectal cancer risk in women". Thanks to all of our longtime participants for your continued commitment to the Sister Study!
A recent study, ![]() looked at whether living in an area with higher levels of a type of air pollution - fine particulate matter (PM2.5) - was associated with genetic changes in certain inflammation-related genes. The researchers looked at two inflammation-related pathways [tumor necrosis factor-alpha (TNFa) and toll-like receptor-2 (TLR-2)], While PM2.5 was not associated with changes to the TLR-2 gene, high levels may be associated with chemical changes (i.e. "methylation") of the TNFa gene. These changes could affect how that gene is expressed in the body. This work is very preliminary, but could help us understand how air pollution affects the risk of inflammation-related chronic diseases, such as cardiovascular disease and cancer.
looked at whether living in an area with higher levels of a type of air pollution - fine particulate matter (PM2.5) - was associated with genetic changes in certain inflammation-related genes. The researchers looked at two inflammation-related pathways [tumor necrosis factor-alpha (TNFa) and toll-like receptor-2 (TLR-2)], While PM2.5 was not associated with changes to the TLR-2 gene, high levels may be associated with chemical changes (i.e. "methylation") of the TNFa gene. These changes could affect how that gene is expressed in the body. This work is very preliminary, but could help us understand how air pollution affects the risk of inflammation-related chronic diseases, such as cardiovascular disease and cancer.
Learn more here:
Long-term ambient fine particulate matter and DNA methylation in inflammation pathways: results from the Sister Study ![]()
Previous research has suggested that poor sleep may be a risk factor for type 2 diabetes. Sister Study researchers found evidence to support this hypothesis, showing that women who reported frequent napping and other markers of poor sleep were more likely to develop diabetes in the future. Because women in racial or ethnic minority groups were more likely to experience both poor sleep and type 2 diabetes than Non-Hispanic white women, these findings underscore the importance of understanding how early life factors contribute to overall health and health disparities.
In a sample of participants from the Sister Study, we measured biologic age, a DNA-based estimate of a woman's age. We were interested in studying the association between biologic age and number of live births, as having children is thought to be protective against breast cancer risk. Our study showed for every live birth a woman reported, her biologic age increased by about 3 months. In other words, childbearing may lead to very slight increases in biologic age.
Learn more here:
Reproduction, DNA methylation and biological age ![]()
Air pollution has been linked to a number of diseases, including cardiovascular disease and death, but less is known about air pollution's role in breast cancer. We evaluated whether air pollution concentrations at the residential level were associated with breast cancer risk. Because the make-up of air pollution varies, we also considered geography and looked at patterns of air pollution composition. We found that among women in the western US and with certain patterns of particulate matter composition, greater exposure to air pollution was associated with higher risk of breast cancer. This research helps to emphasize the importance of continuing to reduce air pollution levels nationwide.
Processed meat has been classified as a cause of colorectal cancer, ![]() and red meat is also thought to be a risk factor for the disease. In a recent Sister Study analysis, researchers sought to further investigate the influence of specific meat products and meat cooking practices on colorectal cancer incidence. Over an average of 9 years of follow-up, 216 women developed colorectal cancer. As expected, we observed a positive association between overall consumption of processed meats and colorectal cancer, with high intake of breakfast sausages and bacon associated with the largest increases in risk. There was also some evidence of a positive association between colorectal cancer and consumption of barbecued or grilled red meat.
and red meat is also thought to be a risk factor for the disease. In a recent Sister Study analysis, researchers sought to further investigate the influence of specific meat products and meat cooking practices on colorectal cancer incidence. Over an average of 9 years of follow-up, 216 women developed colorectal cancer. As expected, we observed a positive association between overall consumption of processed meats and colorectal cancer, with high intake of breakfast sausages and bacon associated with the largest increases in risk. There was also some evidence of a positive association between colorectal cancer and consumption of barbecued or grilled red meat.
Learn more here:
A Prospective Analysis of Red and Processed Meat Consumption and Risk of Colorectal Cancer in Women ![]()
Please take a look at the newly published Sister Study findings on hair dyes and straighteners. As always, for individualized application of study results, please consult your health care provider.
Read more about it here:
Permanent hair dye and straighteners may increase breast cancer risk. ![]()
We examined the association between having experienced childhood trauma and multiple measures of sleep quality. 55% of women in the Sister Study reported experiencing some type of childhood trauma, including a natural disaster, major accident, household dysfunction, sexual trauma, physical trauma, and/or psychological/emotional trauma. We found that women who experienced childhood trauma reported getting less sleep at night, taking longer to fall asleep, waking up more often at night, and taking more naps.
Read more about it here:
Traumatic childhood experiences and multiple dimensions of poor sleep among adult women. ![]()
Sister Study staff scientist, Dr. Katie O'Brien, recently received a grant from the Office of Dietary Supplements to study the association between vitamin D supplement use, blood levels of vitamin D, and breast cancer risk among African-American women enrolled in the Sister Study. The link between vitamin D and breast cancer is not well understood, though findings from some studies suggest that regular supplement use and high blood levels are associated with small reductions in risk. However, these studies have included few African-American women, despite the fact that African-Americans are less likely than other racial/ethnic groups to take vitamin D supplements and more likely to have low vitamin D blood levels. Dr. O'Brien will also investigate how some genetic factors may influence vitamin D blood levels in African-American women.
We would like to introduce you to Dr. Mandy Goldberg, a new post-doctoral fellow and Sister Study researcher. Dr. Goldberg recently received her PhD in Epidemiology from Columbia University, where she studied how early-life experiences may affect age at onset of puberty, breast density and benign breast disease. In her new position, Dr. Goldberg is looking forward to studying early-life risk factors for breast cancer in the Sister Study, including how environmental exposures during your mother's pregnancy and your childhood and adolescence may affect both the timing of puberty and breast cancer risk. Dr. Goldberg is also interested in understanding how family history of breast cancer may influence these relationships.
Working with a summer student from Columbia University, Sister Study researchers found that increasing consumption of red meat was associated with increased risk of invasive breast cancer. Women who consumed the highest amount of red meat had a 23% higher risk compared with women who consumed the lowest amount. Conversely, increasing consumption of poultry was associated with decreased invasive breast cancer risk: women with the highest consumption had a 15% lower risk than those with the lowest consumption. Importantly, the analysis suggested that breast cancer incidence could be reduced if women who eat meat substitute poultry for red meat.
Learn more here:
Study finds a possible link between Meat Consumption and Risk of Breast Cancer ![]()
For the investigation in the link below, we collected information from young breast cancer survivors (diagnosis age less than 45) about their experiences with fertility counseling and treatment. Although 20% of those surveyed said that they were interested in future fertility at the time of their diagnosis, most did not discuss fertility treatment options with their doctor and far fewer actually pursued treatment (only 10% of those who reported interest in future fertility). It is our hope this research will help facilitate communication between oncologists and young patients who may be interested in discussing fertility treatments.
Learn more here:
Fertility-related experiences after breast cancer diagnosis in the Sister and Two Sister Studies ![]()
Meet our Sister Study Operations and Retention team! This group tends to the day-to-day operations of the study. They specialize in operationalizing data collection efforts such as the yearly health update questionnaire, among many other efforts to retrieve information from participants. The team also tends to participants' individual needs and work to reduce burden so participants continue to remain in the study.
In addition to breast and other cancers, Sister Study researchers are interested in studying risk factors for cardiovascular disease. We recently published a study showing that while higher leisure-time physical activity levels are associated with reduced risk of stroke and transient ischemic attacks, higher levels of occupational physical activity may be associated with an increased risk of experiencing these events.
Read more about it here:
Occupational and leisure-time physical activity differentially predict 6-year incidence of stroke and transient ischemic attack in women. ![]()
The human microbiome, the many microbes that live within our body, is thought to play a role in health and disease. Taking antibiotics for a long period of time could change our microbiome. We looked to see whether taking an oral antibiotic at least three times a week for three months or longer was associated with weight change, finding that chronic penicillin use may be associated with increased risk of obesity. The association between other types of antibiotics and weight was less clear. Though this work suggests that antibiotic use could have long-lasting impacts on weight, we consider it very preliminary and hope that future research will be better able to account for the reason antibiotics were prescribed. Please see the link below for more on these findings thanks to our dedicated Sister Study participants. As always, please check with your health care provider for guidance on how these findings may apply to you.
Read more about it here:
Chronic antibiotic use during adulthood and weight change in the Sister Study. ![]()
While the main goal of the Sister Study is to research environmental and genetic causes of breast cancer, we have the opportunity to study other cancers that are important to women. We recently examined two possible risk factors for uterine/endometrial cancer: douching and use of talcum powder in the genital area. Though we did not observe an association between douching and uterine cancer, we saw some evidence that genital talcum powder use may be associated with an increased risk. We consider this work preliminary and are planning to do additional research using data from other large cohorts. As always, please contact your health care provider for help with applying these findings to yourself.
Read more about it here:
Perineal Talc Use, Douching, and the Risk of Uterine Cancer. ![]()
Many Sister Study participants reported exposure to artificial light while sleeping, including having a small nightlight or light from clock radios on in the room (40%), light from outside the room (31%) or a light or television on inside the room (12%). Exposure to any of these was associated with being overweight or obese upon study enrollment, with stronger associations seen for those reporting lights or television on in the room while sleeping. Women who had exposure to artificial light while sleeping were also more likely to gain weight after baseline. Though we cannot confirm that the relationship is causal, our findings provide evidence that lowering exposure to light while sleeping may be a useful intervention for obesity prevention.
Learn more here:
Sleeping with lights on and weight gain in women linked in new study. ![]()
Sleeping with Artificial Light at Night Associated with Weight Gain in Women. ![]()
Association of Exposure to Artificial Light at Night While Sleeping With Risk of Obesity in Women. ![]()
We previously posted about our findings that higher 'biological age', which is determined by measuring molecular changes to the genome (genetic material), was associated with increased breast cancer risk. In an effort to understand what factors might influence biological age, Sister Study investigators looked for differences in biological age between those who reported doing shift work (7% of participants) versus those who did not. Those who reported doing shift work tended to have a biological age that was older than their age in calendar years, especially if they worked night shifts. On average, those who worked for more than 10 years in a job that included night shifts were 3 years "older" than their chronological age. This research helps us understand some of the chemical processes that may explain previously observed associations between shift work and chronic diseases like breast cancer.
For those interested in learning more about the association between shift work and breast cancer, the National Toxicology Program recently released a report stating that "There is strong, but not sufficient, evidence from cancer epidemiology studies that persistent night shift work (e.g., frequent and long-term, or working a large number of night shifts over a lifetime, especially in early adulthood) causes breast cancer in women."
Read more about it here:
Shift work, DNA methylation and epigenetic age. ![]()
We would like to introduce you to Dr. Nicole "Nikki" Niehoff, a new post-doctoral fellow and Sister Study researcher. Dr. Niehoff has already made major contributions to the Sister Study through her work as a doctoral student in Epidemiology at the University of North Carolina, studying air pollutants, pesticides, and physical activity in relation to breast cancer risk. In her post-doctoral position, Dr. Niehoff will continue to study environmental risk factors for breast cancer, including how obesity and other metabolic factors affect the relationship between the environment and cancer, and how multiple pollutants together influence risk.
When we talk about genetic risk factors for breast cancer, we are usually referring to how the genes we are born with can influence our risk of getting breast cancer. However, breast cancer may also be affected by change to our genes that occur after birth. Epigenetics is a term that refers to biologic changes that can affect DNA, including "DNA methylation", which can affect which genes can be "read" and turned into proteins. In a recent publication, Sister Study authors discuss how they examined more than 400,000 known DNA methylation markers, measured in DNA from blood samples given at study enrollment. The researchers identified several thousand methylation markers associated with breast cancer. Since the associations were stronger for breast cancer diagnosed shortly after study enrollment, they hypothesize that many of these markers may be indicators of early disease. These results could help develop tools for detecting invasive breast cancer at an early stage.
Read more about it here:
Blood DNA methylation and breast cancer: A prospective case-cohort analysis in the Sister Study. ![]()
As previously discussed, even though the DNA you inherit from your parents is generally not modifiable, biological changes within cells over time can affect how the body reads and processes your genetic information. Sister Study investigators are very interested in learning about what environmental and lifestyle factors might affect DNA methylation, a type of genetic alteration that serves as an indicator of which genes are turned "on" or "off". In a recent study, we identified many such markers that may be associated with high alcohol consumption, which is a known risk factor for breast cancer and other diseases. These results may help explain how alcohol affects the body and increases disease susceptibility.
Read more about it here:
Alcohol and DNA Methylation: An Epigenome-Wide Association Study in Blood and Normal Breast Tissue. ![]()
In a recently published study, Sister Study researchers found that women who ate breakfast every morning were less likely to be or become obese, compared to women who irregularly ate breakfast (3-4 days a week). On the other hand, women who never ate breakfast were also less likely to be obese than those who irregularly ate breakfast. We interpret this to mean that a regular breakfast consumption habit, whether it be eating breakfast every day or never eating breakfast, may be important for maintaining a healthy weight.
Read more about it here:
Day-to-day regularity in breakfast consumption is associated with weight status in a prospective cohort of women. ![]()
The DNA you inherit from your parents is largely fixed and unchangeable. However, outside factors can alter how your body reads and uses the information coded in the genes. One such example is DNA methylation, where the presence of certain molecules (a "methyl" group) on the strand of DNA can affect whether the gene is turned "on" (i.e. it can be read) or "off". We recently found that Sister Study participants who were born to older mothers had different DNA methylation patterns than those with younger mothers. We do not yet know what this means in terms of health or breast cancer risk, specifically, but it could be a clue as to why some conditions or diseases are more common in individuals born to older mothers.
Read more about it here:
Persistent epigenetic changes in adult daughters of older mothers. ![]()
In a recently published study led by Sister Study investigators Symielle Gaston and Chandra Jackson, women who averaged less than 7 hours of sleep per night and who had difficulty falling or staying asleep were more likely to have metabolic disorders like high blood pressure and obesity. These associations were usually stronger in premenopausal women than postmenopausal women. Because sleep and metabolic disorders were measured at the same time, we could not assess which occurred first. However, this work helps us to understand the biological relationship between sleep and metabolic disorders and to identify possible approaches to prevent metabolic disorders in women. As always, please consult your health care provider to tailor these findings individually.
All paper surveys and other forms you complete and return to the Sister Study are handled by this team. Your responses are securely processed into our system in preparation for their eventual analysis by our researchers. We are grateful for your diligence in completing your health update surveys! Those responses directly inform the research findings we share with you in this Facebook group. Thanks to what you share with us, researchers have published over 100 articles.
Please visit our website to view these articles:
Sister Study articles
Thanks to our Sister Study participants' continued dedication to the study, researchers are able to publish such important findings as the ones described in this news release. We encourage you to read about "if a woman's biologic age is older than her chronologic age, she has an increased risk of developing breast cancer."
Read more about it here:
Older biologic age linked to elevated breast cancer risk. ![]()
Anti-Müllerian hormone (AMH), like estrogen, is a marker of ovarian function. Levels decrease as women approach menopause. AMH levels are thought to correspond with how many egg cells remain in the ovaries, so the measure has implications for fertility. Like estrogen, higher levels may be associated with breast cancer risk. But unlike estrogen, AMH has the advantage that levels do not change across the menstrual cycle, making it easier to use in research studies. Sister Study investigators measured AMH in blood samples collected at enrollment from a subgroup of participants who had not yet gone through menopause, and looked at how dietary factors might be related to levels. The results indicated that dietary fat intake may be associated with lower AMH, but that other factors, including protein and alcohol intake were not related to AMH levels. Please check with your health care provider about applying these results individually.
Read more about it here:
Dietary factors and serum Anti-Müllerian hormone concentrations in late premenopausal women. ![]()
You may find this article on testing for BRCA1 and BRCA2 interesting and helpful. As always, please consult your health care provider to interpret and apply specifics to your own health.
Read more about it here:
Taking the Uncertainty Out of Interpreting BRCA Variants. ![]()
Fruits and vegetables contain nutrients called antioxidants, which may counteract cell damage caused by harmful substances. Green and black tea contain some types of antioxidants, but their specific health benefits are not fully understood. In a small study that included 889 Sister Study participants, we looked at whether consumption of black or green tea was associated with biologic measures of oxidative stress, a measure of the balance between the body's potentially harmful (oxidative) and potentially beneficial (antioxidant) chemicals. We found that while black tea may be associated with lower levels of oxidative stress, green tea was not. Related research is looking at whether tea consumption is related to breast cancer risk.
Read more about it here:
Tea consumption and oxidative stress: a cross-sectional analysis of 889 premenopausal women from the Sister Study. ![]()
Did you know that the average age of women in the Sister Study is now 67 years of age? Our youngest Sister participant is just 44 years young and our "wisest" participant is going strong at 89!
Research has shown that engaging regularly in exercise reduces breast cancer risk generally, but it was not clear whether the benefit would also apply to women with a family history of breast cancer. Our research in the Sister Study, where all women have a family history of breast cancer, showed that being more physically active was associated with a reduction in postmenopausal breast cancer, but not premenopausal breast cancer. Please check with your health care provider about applying these results individually.
Read more about the research here:
Adult Physical Activity and Breast Cancer Risk in Women with a Family History of Breast Cancer. ![]()
Heart disease is the leading cause of death for women in the United States. Over the years, we have asked you questions about your cardiovascular health and disease history. We are excited to let you know that we are working with cardiovascular disease experts to study environmental contributors to stroke, heart attack, and congestive heart failure. As part of that effort, in October we started requesting medical records to confirm diagnoses and obtain needed details about reported heart conditions such as results of tests performed and disease subtypes. Our goal is to identify preventable environmental causes of cardiovascular disease. We have reached out to some of you for more information about your health history. If you were contacted and returned your authorization forms, we thank you! But if you haven't yet done so we encourage you to sign and mail your forms soon. Thank you again for your contributions to the Sister Study. We couldn't do this research without your willingness to participate!
We would like to introduce you to Dr. Symielle Gaston, a post-doctoral research fellow working with the Sister Study. Dr. Gaston is interested in studying how the physical and social environments contribute to racial/ethnic and socioeconomic disparities in cardiovascular health. For instance, how living in neighborhoods with social and physical disorder may negatively affect cardiovascular health. She recently received a grant to support this research. In the Sister Study, she has several ongoing projects, including a study of the association between racial/ethnic discrimination and poor sleep, an understudied contributor to cardiovascular health and other health conditions.
Read more here:
Postdoc awards reflect strong research potential ![]()
We would like to announce that Dr. Alexandra White joined the Sister Study as a Stadtman Tenure-Track Investigator. ![]() Dr. White's research will focus on identifying environment and lifestyle risk factors for cancer and understanding the biologic mechanisms that allow cancer to develop. She has already worked for three years as a post-doctoral fellow on the Sister Study, publishing research on factors that may influence breast cancer risk, such as alcohol consumption, smoking, physical activity, and obesity. She is particularly excited to expand her research to examine the effects of exposure to toxic metals and air pollution on breast density and breast cancer risk.
Dr. White's research will focus on identifying environment and lifestyle risk factors for cancer and understanding the biologic mechanisms that allow cancer to develop. She has already worked for three years as a post-doctoral fellow on the Sister Study, publishing research on factors that may influence breast cancer risk, such as alcohol consumption, smoking, physical activity, and obesity. She is particularly excited to expand her research to examine the effects of exposure to toxic metals and air pollution on breast density and breast cancer risk.
In the first study to make use of the data from the "Sisters Changing Lives" sub-study, we measured the concentrations of 16 trace elements in each of two sets of toenail samples; the first collected at enrollment and the second in 2013-2014. We found that concentrations of most of the elements decreased over time, with the biggest decreases seen for lead, cadmium and chromium. This was true for women who were diagnosed with breast cancer between enrollment and 2013 and women who were not. This work was led by Drs. Katie O'Brien and Clarice Weinberg, both NIEHS investigators.
Read more about it here:
Do Post-breast Cancer Diagnosis Toenail Trace Element Concentrations Reflect Prediagnostic Concentrations? ![]()